The FDA, along with CDC and state and local partners, investigated a multistate outbreak of E. coli O157:H7 infections in the fall of 2020. The epidemiology and traceback investigation have determined that the outbreak was linked to leafy greens. The epidemiological and traceback investigations were not able to determine a specific type of leafy green linked to illnesses. On 12/22/2020, the CDC announced that this outbreak appears to be over. This outbreak, announced by FDA and CDC on October 28, 2020, was caused by a strain of E. coli that is genetically related to a strain linked to the fall 2019 romaine outbreak.
The FDA completed a traceback investigation of multiple types of leafy greens identified in patient interviews. Although no single ranch was identified as a common source of the leafy greens, FDA and state partners also conducted on-site investigations on farms of interest.
Teams were deployed to dozens of ranches in the region to conduct large scale environmental sampling. Additionally, no Shiga toxin-producing E. coli were found on leafy greens.
At this time, FDA’s investigational activities, including sample analysis are ongoing. A detailed report of FDA’s findings in the investigation will be released in early 2021, following the conclusion of investigational activities.
Recommendation
CDC has declared this outbreak to be over. There is no recommendation for consumers, retailers, or suppliers.
Case Count Map Provided by CDC
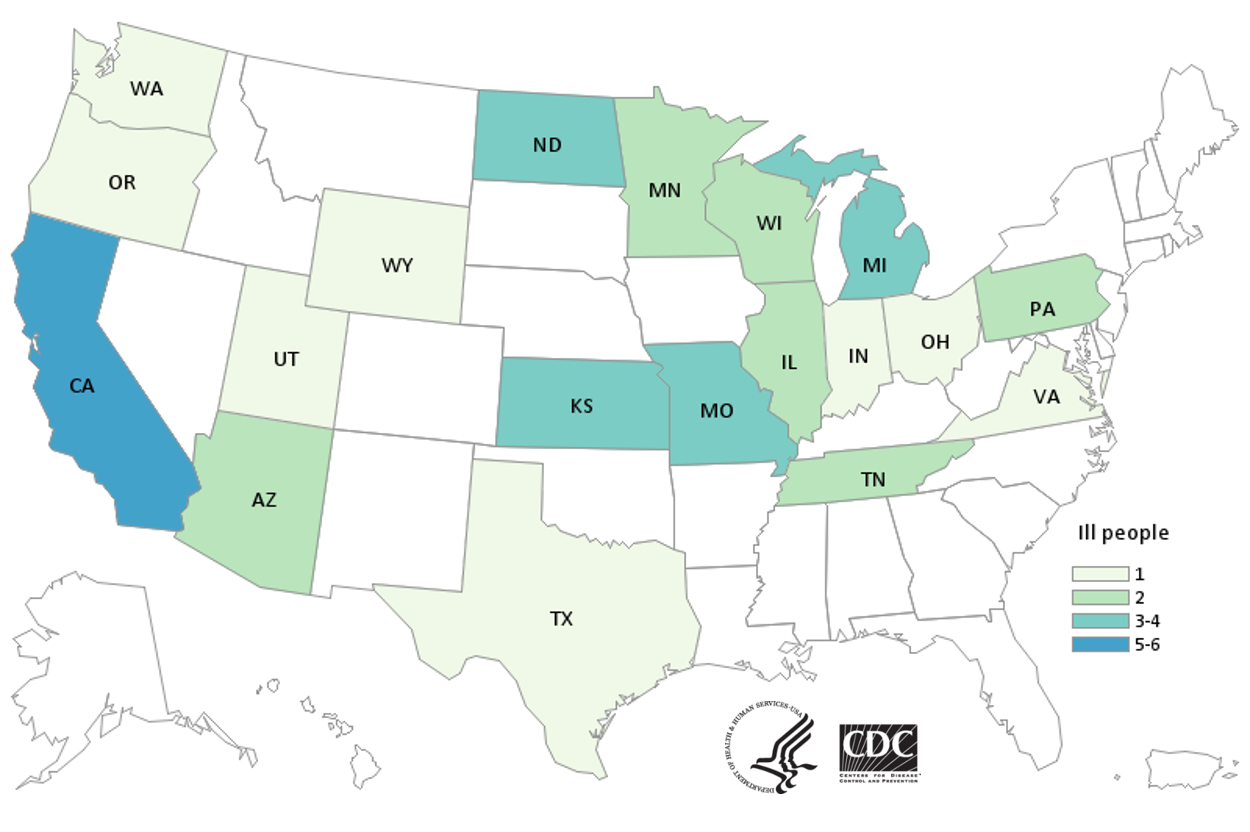
Case Counts
Total Illnesses: 40
Hospitalizations: 20 (4 Cases HUS)
Deaths: 0
Last Illness Onset Date: October 31, 2020
States with Cases: AZ (2), CA (6), IL (2), IN (1), KS (4), MI (3), MN (2), MO (3), ND (4), OH (1), OR (1), PA (2), TN (2), TX (1), UT (1), VA (1), WA (1), WI (2), WY (1)
*States with confirmed distribution; product could have been distributed further