CIDRAP
The latest data from a national surveillance system that monitors foodborne bacterial pathogens for antimicrobial resistance (AMR) shows some concerning changes in resistance patterns among serotypes of Salmonella.
The findings come from the National Antimicrobial Resistance Monitoring Systems (NARMS) 2019 Integrated Summary, which combines data from the Centers for Disease Control and Prevention (CDC), the Food and Drug Administration (FDA), and the US Department of Agriculture (USDA). The report provides a snapshot of resistance patterns found in bacteria isolated from humans, animals, raw meats from retail outlets (chicken, ground turkey, ground beef, and pork chops), and meat and poultry product samples collected at slaughtering facilities.
In addition to Salmonella, which causes an estimated 1.35 million illnesses and 26,500 hospitalizations each year, the NARMS report also includes resistance data on Campylobacter (1.5 million illnesses and 19,500 hospitalizations), Escherichia coli, and Enterococcus. NARMS monitors these bacteria to detect emerging resistance patterns to the antibiotics that are most important to human medicine, multidrug resistance, and specific resistance genes.
Increase in multidrug-resistant Salmonella serotype
Overall, the NARMS report shows that more than three fourths of the Salmonella isolates (78%) from humans were not resistant to any of the antibiotics tested, and that the overall level of resistance in humans remains relatively unchanged since 2018. However, the report also found rising resistance to ciprofloxacin—one of the three antibiotics used to treat severe Salmonella infections.
From 2018 to 2019, Salmonella with decreased susceptibility to ciprofloxacin increased from 9% to 11% in humans, from 18% to 31% in retail chicken, from 20% to 30% in chicken product samples, from 26% to 32% in chicken cecal content samples, and from 0% to 14% in retail pork samples.
The increase in resistance to ciprofloxacin among poultry isolates was primarily due to the increase in Salmonella Infantis, a multidrug-resistant (MDR) serotype that emerged in 2014.
The rise in Salmonella Infantis isolates was also behind an increase in MDR isolates found in retail chicken (from 20% to 32%) and in chicken product samples (22% to 29%). Up to 10 antimicrobial resistance (AMR) genes were found in some of the Salmonella Infantis isolates.
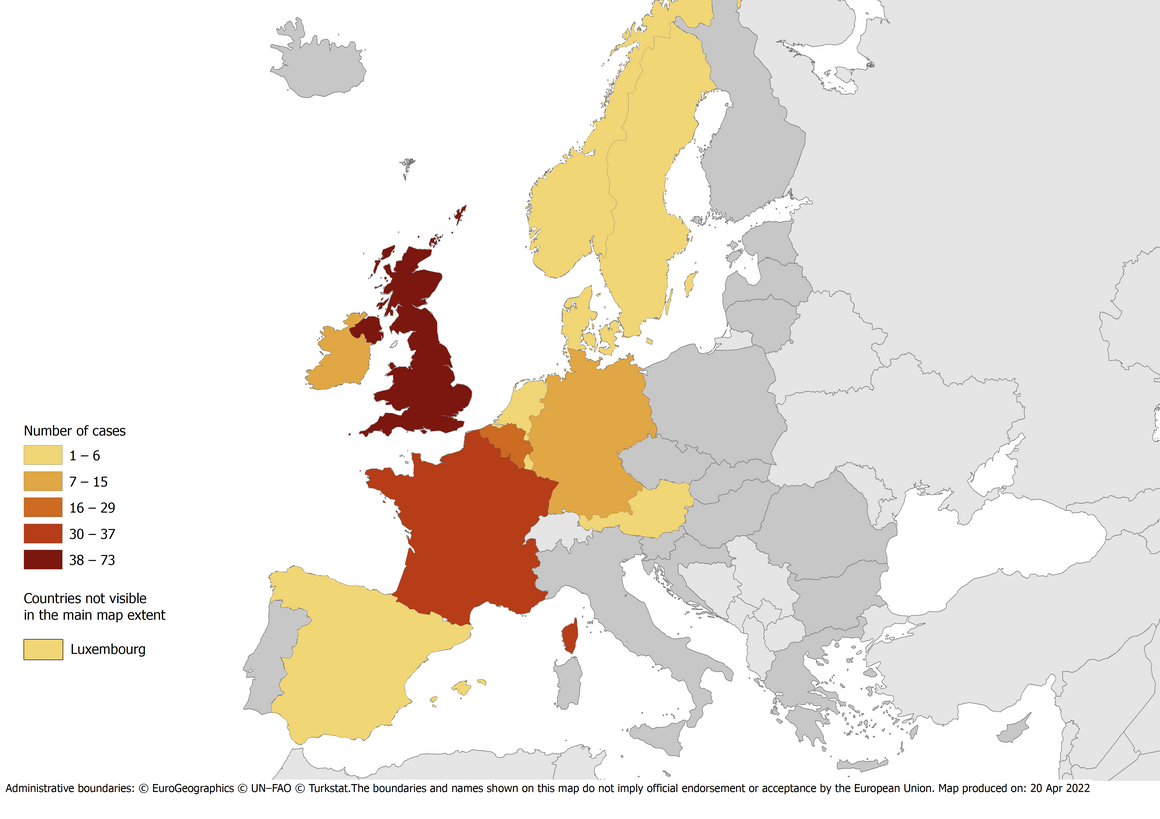
In addition, the NARMS report shows an increase in another MDR Salmonella serotype, I 4,[5],12:i:-, which is linked to pigs and has become an increasing public health concern in Europe and the United States. The percentage of MDR isolates from humans that are of the I 4,[5],12:i:- serotype rose from 7% in 2010 to 26% in 2019, and from 7% to 35% in swine samples.
NARMS data also show rising fluoroquinolone resistance in Campylobacter isolates. In humans, the proportion of ciprofloxacin-resistant Campylobacter isolates rose from 29% in 2018 to 34% in 2019 for Campylobacter jejuni and from 41% to 45% in C coli. Ciprofloxacin-resistant C jejuni isolated from chicken cecal contents (21% in 2018 to 26% in 2019) and chicken retail samples (20% to 22%) also rose.
Analysis of E coli isolates found increases in ceftriaxone resistance in sow cecal samples (3% in 2018 to 7% in 2019) and in retail pork (4% to 7%). Whole-genome sequencing of Salmonella and E coli from animals, animal products, and retail meats found that none harbored any of the MCR-1 through MCR-8 colistin-resistance genes.