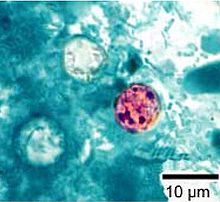
The parasite, Cyclospora, continues to provide illness and intrigue.
Florida-based Southeastern Grocers has issued a voluntary recall for its “SE Grocers Naturally Better Organic Fresh Cut Basil” following the detection of Cyclospora.
The company says the product was delivered through all of its distribution centers and sold in all its stores, including Winn-Dixie, BI-LO, Fresco y Más and Harveys Supermarkets. The basil comes in a 0.5-ounce container with UPC code 6-07880-20230-4.
The latest recall follows a summer outbreak of Cyclospora in the U.S. linked to Fresh Express and private label brand salad products produced at its Streamwood, IL facility that contain iceberg lettuce, red cabbage, and/or carrots.
690 people with laboratory-confirmed Cyclospora infections and who reported eating bagged salad mix before getting sick weren reported from 13 states (Georgia, Illinois, Iowa, Kansas, Massachusetts, Minnesota, Missouri, Nebraska, North Dakota, Ohio, Pennsylvania, South Dakota, and Wisconsin).
Illnesses started on dates ranging from May 11, 2020 to July 20, 2020.
37 people were hospitalized. No deaths were reported.




