Update on April 25, 2022 on the grouped cases of haemolytic-uremic syndrome and E. coli infections producing shiga-toxin and the consumption of frozen pizzas from the Fraîch’Up range of the Buitoni® brand.
Public Health France and the National Reference Center (CNR) E. coli and its associated laboratory (Institut Pasteur, Paris, and Microbiology Laboratory of the Robert Debré Hospital, Paris), in conjunction with the Directorate General for Food, the Directorate General for Competition, Consumer Affairs and Fraud Prevention, and in coordination with the Directorate General for Health, have been investigating since 02/10/2022 an increase in the number of cases of haemolytic uremic syndrome (HUS) pediatric infections and Shiga toxin-producing Escherichia coli (STEC) infections.
The epidemiological, microbiological and traceability investigations carried out since that date have confirmed a link between the occurrence of these grouped cases and the consumption of frozen pizzas from the Buitoni brand Fraîch’Up range contaminated with STEC bacteria. On 03/18/2022, the company proceeded with the withdrawal-recall of all the pizzas in the Fraîch’Up range, marketed since June 2021 and the authorities asked the people who hold these pizzas not to consume them and to destroy them.
The total number of HUS cases linked to the consumption of these pizzas seems to have stabilized since the withdrawal-recall.
Case of SHU in France: update on 04/25/22
As of 04/25/2022, 55 confirmed cases have been identified, of which 53 are linked to STEC O26 strains, and 2 to STEC O103 strains.
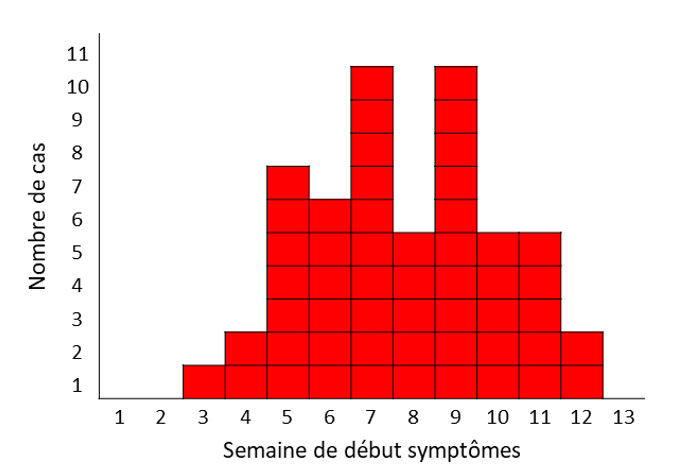
These 55 cases occurred in 54 children and 1 adult, who presented symptoms between 18/01/2022 (week 3) and 25/03/2022 (week 12) (Figure 1). The epidemic peak is in week 7 (14/02 to 20/02) and week 9 (28/02 to 06/03), with 10 cases each of these weeks.
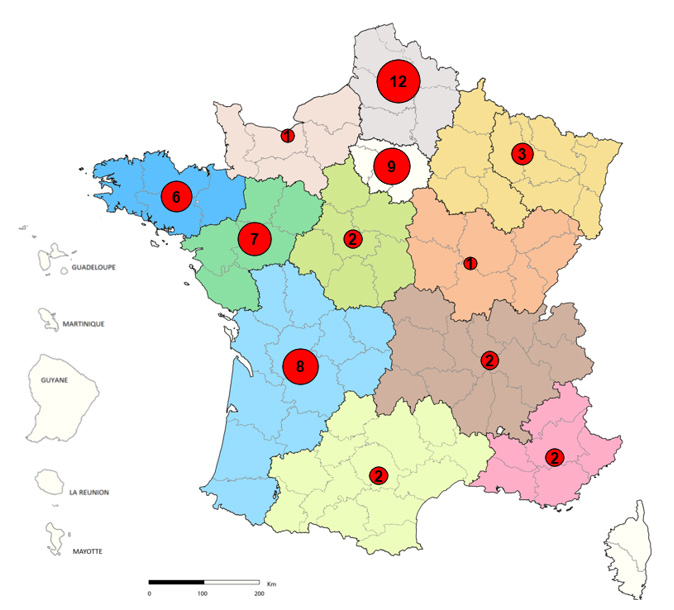
These 55 cases occurred in 12 regions of metropolitan France: Hauts-de-France (12 cases), Ile-de-France (9 cases), New Aquitaine (8 cases), Pays de la Loire (7 cases), Brittany ( 6 cases), Grand Est (3 cases), Auvergne-Rhône-Alpes (2 cases), Occitanie (2 cases), Provence-Alpes-Côte d’Azur (2 cases), Center Val-de-Loire (2 cases) , Bourgogne Franche-Comté (1 case) and Normandy (1 case) (figure 2).
The 54 sick children are aged from 1 to 17 years with a median age of 7 years; 24 (44%) are female; 47 (87%) presented with HUS, 7 (13%) with STEC gastroenteritis. Two children died. The adult did not present with HUS.
Figure 1 – Epidemic curve: number of confirmed cases of HUS and STEC infections, by week of onset of symptoms – Metropolitan France, weeks 3 to 12, 2022 (N=53: week of onset of symptoms not specified for 2 cases )
Figure 2 – Geographical distribution of confirmed cases of HUS and STEC infections (N=55) linked to the consumption of Buitoni® brand Fraîch’Up pizzas, by region of residence in metropolitan France, weeks 3 to 12, 2022