SSI
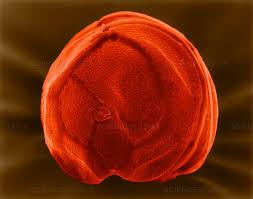
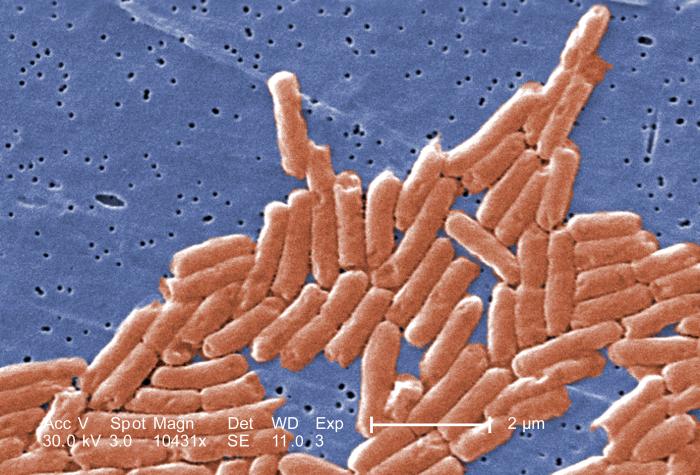
The Statens Serum Institut and the Danish Veterinary and Food Administration are currently investigating a disease outbreak in a company with a microorganism that has so far not been registered as a cause of disease outbreaks in Denmark. It is a species of microsporidia, Enterocytozoon bieneusi. It is believed that the infection occurred through food.
In October, a company in the metropolitan area reported more than 70 cases of diarrhea among their employees.
The Statens Serum Institut (SSI) has so far found samples from 11 people positive for Enterocytozoon bieneusi, which is a species of microsporidia. It is not a microorganism that we often detect in Denmark, and we have not previously seen disease outbreaks with it.
The infection can cause severe and prolonged diarrhea, abdominal pain and nausea. In addition, there may be symptoms such as fever, headache, muscle aches and fatigue (flu-like). The infection occurs from feces from infected people with poor hygiene to other people either directly or through food and drink.
“There are no registered persons outside the company who should have been infected with E. bieneus. But we urge the country’s physicians to pay attention to patients with prolonged diarrhea for no apparent reason. Especially if it is about immunocompromised people and with particularly long-lasting symptoms, ”says ward doctor Lasse Skafte Vestergaard, SSI. Read more about the disease outbreak with microsporidia (EPI-NEWS – week 52a – 2020)
Microsporidia are protozoan parasites belonging to the phylum Microsporidia within which exist over 1000 species classified into approximately 100 genera. These eukaryotic obligate intracellular protozoans have been described infecting every major animal group, especially insects, fish, and mammals (Wittner 1999). Microsporidia have been increasingly recognized as opportunistic pathogens of immunodeficient patients (Weber et al. 1994), especially in Aids patients but it is also becoming increasingly common in immunocompetent individuals (Gainzarain et al. 1998, Lores et al. 2001).
Although during the last decade numerous data related to the epidemiology of this infection in humans and animals have been accumulated, implying a zoonotic nature of these parasites, direct evidence of transmission from animals to humans are still lacking (Deplazes et al. 2000).
Encephalitozoon cuniculi is probably the most extensively studied mammalian microsporidian and has been reported to infect a wide range of hosts, including common laboratory rodents as well as human and non-human primates. This is the first microsporidian species infecting humans that has been considered a zoonosis (Deplazes et al. 1996, Didier et al. 1996) .
The first identification of E. intestinalis in mammals other than humans was reported by Bornay et al. (1998) in the faeces of donkeys, dogs, pigs, cow, and goat suggesting that E. intestinalis might also be of zoonotic origin.
Enterocytozoon bieneusi is the most frequent microsporidian found in humans, especially in Aids patients. It has been associated mainly with chronic diarrhoea, although it has been diagnosed in patients with other forms of immunosuppression and in immunocompetent travellers with self-limited diarrhoea (Weber & Bryan 1994, Sobottka et al. 1995). In addition, this pathogen has recently been detected in other natural hosts such as pigs (Deplazes et al. 1996, Breitenmoser et al. 1999, Rinder et al. 2000), cows, goats, pigs, chickens, cats, turkeys (Bornay et al. 1998), rabbits, dogs (del Aguila et al. 1999), and in simian immunodeficiency virus-inoculated monkeys (Tzipori et al. 1997, Mansfield et al. 1997). Consequently, this microsporidian infection may be more common than previously suspected.