Similarly to many other countries across the globe, several floods have been recorded in Italy throughout the last few decades, including those of catastrophic magnitude that occurred in the Emilia-Romagna and Tuscany regions last May and a few weeks ago, respectively. This, once again, underscores the increasingly growing probability, in the current “
Anthropocene Epoch”, of global warming-related, extreme weather phenomena. Indeed, the last 8 years (2015–2022) have been characterized by the highest average temperatures ever recorded on Earth throughout the last 140 years [
1].
Within such a challenging and alarming scenario, the land-to-sea transfer of a huge (and progressively increasing) number of infectious agents appears to be a matter of relevant concern [
3,
4]. This especially applies to bacterial microorganisms shed into the external environment via the fecal route, such as
Salmonella spp.,
Escherichia coli,
Vibrio cholerae and
Listeria monocytogenes, alongside protozoan pathogens like
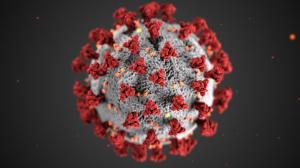
Toxoplasma gondii and/or viral agents like the one causing hepatitis A and, last but not least, the pandemic SARS-CoV-2 betacoronavirus. As a matter of fact, evidence of viral fecal shedding has been documented for a median duration of 22 days in 59% of subjects from a cohort of SARS-CoV-2-infected patients in China [
5]. Once transferred into sea and ocean waters by flood-derived mud and debris, fecally excreted microbial pathogens may be ingested by edible bivalve mollusks like mussels, an organism in which a single individual is able to filter over 100 liters of water on a daily basis, thus potentially hosting inside its body tissues significant amounts of biological and chemical environmental pollutants [
6]. Within this context, it is worth mentioning a
V. cholerae infection outbreak linked to the consumption of raw, non-sterilized mussels which diffusely involved the human population from the cities of Naples and Bari during the summer and early autumn months of 1973 [
7]. Moreover, the land-to-sea transfer of infectious agents may additionally involve free-ranging cetaceans, whose health and conservation
status appear to be increasingly threatened by a long and progressively expanding list of both natural and anthropogenic factors. This holds particularly true for “inshore” species like bottlenose dolphins (
Tursiops truncatus), which are more prone to acquire infections caused by “terrestrial” pathogens like
T. gondii [
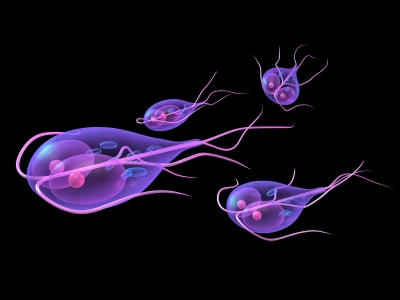
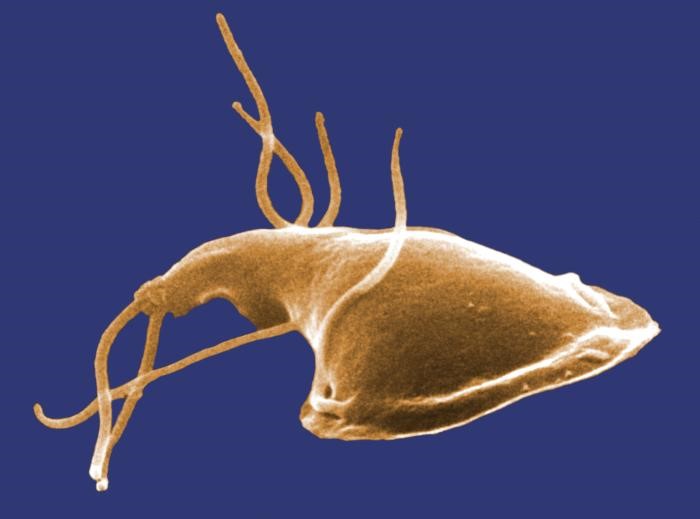
8] while being simultaneously able to accumulate and “biomagnify” inside their body tissues consistent amounts of human-made, persistent, immunotoxic, neurotoxic and endocrine-disrupting environmental pollutants, based upon their well-known position of “apex predators” within the marine and oceanic food chains. Furthermore, the proven capability of micro-nanoplastics—exceedingly contaminating global seawaters—to behave as “attractors and concentrators” for the aforementioned anthropogenic xenobiotics should also be taken into serious account, together with the demonstrated interaction of micro-nanoplastics in marine and oceanic ecosystems with zoonotic protozoan pathogens like
T. gondii,
Cryptosporidium parvum and
Giardia enterica [
9]. This scenario, which already appears to be quite intricate and complex by itself, is made even more alarming by the fact that micro-nanoplastics may also host and carry a wide range of antibiotic-resistant bacteria, from which an active and powerful exchange of antimicrobial resistance genes may additionally occur, through horizontal gene transfer, with several environmental bacterial species colonizing the same plastic substrates [
10].