Salmonella in poultry meal from the United Kingdom in Netherlands and Belgium
Salmonella Isangi in feed materials from Germany in Norway
Salmonella in poultry meal from the United Kingdom in Netherlands and Belgium
Salmonella Isangi in feed materials from Germany in Norway
Posted in Animal Feed, Animal Feed Salmonella, Animal Feed Testing, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, RASFF, Salmonella
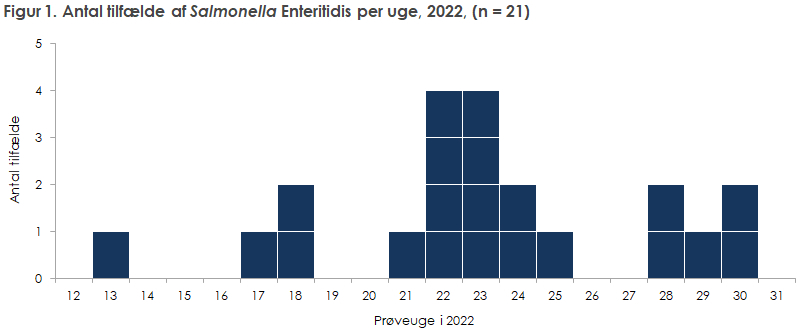
Since 31 March 2022, 21 cases of Salmonella Enteritidis have been registered at the Statens Serum Institut. In the current outbreak, the source of infection remains unknown, but an investigation is underway.
Between 31 March 2022 and 30 July 2022, 21 people have been registered at the Statens Serum Institut who have been infected with the same type of Salmonella Enteritidis (figure 1). Among the sick are 15 men and 6 women. The patients are between 8-59 years old (median age is 28 years). The patients primarily live in the Capital Region and Zealand Region (table 1).
The Statens Serum Institut is working together with the Danish Veterinary and Food Administration and the Norwegian Food Institute DTU on this outbreak to identify the source of infection.
| Region | Number of patients |
| The capital | 13 |
| Zealand | 5 |
| Central Jutland | 2 |
| Southern Denmark | 1 |
| Northern Jutland | 0 |
| Total | 21 |
The bacteria is of the type Salmonella Enteritidis. When whole-genome sequencing of the bacteria isolated from the patients shows that they are very closely related and belong to sequence type 11.
Salmonella is found in animals and can infect humans through food contaminated with the bacteria. Salmonella is a frequent and well-known cause of bacterial intestinal infections in Denmark. There are more than 2,500 different types of salmonella.
The time that passes from being infected to getting symptoms varies from 6-72 hours. Usually 12-36 hours before symptoms appear.
Infection with salmonella typically causes general malaise, diarrhoea, stomach ache, possibly nausea, vomiting and/or fever. The infection is often accompanied by joint pain, muscle pain and headache. Plenty of fluids are important to prevent and treat dehydration from diarrhea and vomiting. In the event of severe diarrheal disease, a doctor should be consulted.
Posted in food bourne outbreak, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, foodborne outbreak, foodbourne outbreak, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Salmonella
| Date Posted |
Ref |
Pathogen |
Product(s) Linked to Illnesses (if any) |
Total Case Count |
Status |
| 8/17/
2022 |
1081 | E. coli O157:H7 |
Not Yet Identified | See CDC Investigation Notice | Active |
| 8/17/
2022 |
1087 | Salmonella Senftenberg |
Not Yet Identified | 19 | Active |
| 8/17/
2022 |
1095 | Salmonella Typhimurium |
Not Yet Identified | 44 | Active |
| 8/3/
2022 |
1080 | Cyclospora | Not Yet Identified | 6 | Active |
| 7/27/
2022 |
1084 | Cyclospora | Not Yet Identified | 98 | Active |
| 6/29/
2022 |
1076 | Not Yet Identified | Frozen Food | See Outbreak Advisory |
Active |
| 6/22/
2022 |
1075 | Salmonella Braenderup |
Not Yet Identified | 74 | Active |
| 6/22/
2022 |
1072 | Salmonella Paratyphi B var. L(+) tartrate+ |
Not Identified | 14 | Closed |
| 6/15/
2022 |
1070 | Listeria monocytogenes |
Not Identified | 12 | Closed |
| 6/8/
2022 |
1068 | E. coli O157:H7 |
Not Identified | 10 | Closed |
| 6/1/
2022 |
1066 | Hepatitis A Virus | Strawberries | See Outbreak Advisory |
Closed |
| 5/25/
2022 |
1067 | Salmonella Senftenberg |
Peanut Butter | See Outbreak Advisory | Closed |
| 4/20/
2022 |
1064 | Not Yet Identified |
Dry Cereal | 558 adverse event reports |
Active |
| 4/13/
2022 |
1057 | Listeria monocytogenes |
Ice Cream | See Outbreak Advisory | Active |
| 3/30/
2022 |
1060 | None Identified |
Meal Replacement Drink |
6 adverse event reports |
Closed |
| 3/16/
2022 |
1055 | Salmonella Saintpaul |
Not Identified | 60 | Closed |
| 2/17/
2022 |
1056 | Cronobacter sakazakii |
Powdered Infant Formula |
See Advisory |
Active (IMG) |
| 2/9/
2022 |
1040 | Listeria monocytogenes |
Not Identified | 20 | Closed |
| 2/2/
2022 |
1054 | Enteroinvasive E. coli O143:H26 |
Not Identified |
16 | Closed |
| 1/10/
2022 |
1050 | E. coli O121:H19 |
Romaine | 4 | Closed |
Posted in Cronobacter sakazakii, Cyclospora, Cyclosporiasis, E.coli O121, E.coli O157, E.coli O157:H7, FDA, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, Foodborne Illness Death, foodborne outbreak, foodbourne outbreak, Hepatitis A, Illness, Listeria, Listeria monocytogenes, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, O143:H26, outbreak, Salmonella

Raw Oysters are High-risk Foods
Oysters are filter feeders. They constantly draw in water and accumulate materials from water, including pathogens such as Vibrio bacteria, norovirus and hepatitis A virus. These pathogens can infect people who eat oysters raw or undercooked. In addition, bacteria like Vibrio can continue to grow in oysters after harvesting if oysters are not maintained at low enough temperatures from harvest through to consumption. Food poisoning outbreaks related to raw oysters have been reported locally from time to time. Although the illness is usually mild and self-limiting, causing symptoms such as diarrhoea, abdominal cramps and vomiting, they can also cause severe health consequences especially for susceptible individuals.
Additional Risks in Shucked Oysters
Both physical and microbiological contamination are possible during the shucking of oysters. Physical removal of shellfish meat from the shell at the shucking table often exposes the product to dirt, mud and detritus. Shucked oysters should be rinsed or washed well to eliminate these contaminants and to reduce microbiological level of the products. Good hygiene practices should also be observed to minimise contamination from the workers and the working environment.
Before deshelling, oysters can stay alive even after long-haul shipping if kept under correct temperature and conditions. Once killed after shucking, raw oysters can deteriorate quickly if the temperature is not low enough to limit bacterial growth. Shucked oysters should be packed and chilled or frozen as soon as possible. Furthermore, an uninterrupted cold chain during transportation is critical to ensure safety and quality of the shellfish products.
Posted in Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, Hepatitis A, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Norovirus, Norovirus Oysters, Pathogen, pathogenic, Vibrio, Vibrio parahaemolyticus
With at least 18 ill in Ohio and nearly 100 ill in Michigan – not yet clear if the outbreaks from the two states are linked – the public is looking for information about this potentially deadly pathogen.
Read all about it at the link above
Posted in Decontamination Microbial, E.coli, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak
Almost 30 cases of E. coli infection have been linked to a nursery in Scotland.
NHS Lothian is part of a team investigating 28 cases of E. coli linked to Pear Tree Nursery on Church Street in Haddington. Officials previously said E. coli O157 had sickened a number of young people in the East Lothian area.
Cases are confined to the nursery, respective households, or other close contacts. The site has been closed while the investigation continues.
A number of confirmed patients have been hospitalized but all are in a stable condition. Most people had mild symptoms and did not require hospital treatment.
Some people at a partner nursery in the same town reported symptoms of vomiting and diarrhoea, which have resolved without medical treatment. Meadowpark Pear Tree Nursery in Haddington has also been closed.
Posted in E.coli O157, E.coli O157:H7, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, Illness, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, STEC, STEC E.coli
Public health officials in Guatemala have issued a warning as 40 people fell sick after eating dairy products.
The Ministry of Public Health and Social Assistance reported the food poisoning of 41 people after eating artisanal cheese in the town of Ciudad Vieja, in the department of Sacatepéquez.
The first cases were detected on Aug. 9. People with a history of consuming fresh cheese were treated for abdominal pain, nausea and vomiting.
Authorities advised local people to avoid consuming dairy products without knowing the origin and to check the label of the product to ensure it is made with pasteurized milk. These preventative steps should be in place at least until the investigations are completed to determine the origin of the current outbreak to stop more people from getting sick.
They also recommended that the public reinforce hygiene practices such as handwashing, the correct preparation, handling and storage of food, and to seek treatment if they feel unwell.
A three-year-old toddler in Kasese District died Sunday while 20 others from different families have been hospitalised over suspected poisoning.
The deceased child has been identified as Rosemary Kabugho, whose four other siblings are among the 20 people who are admitted to Kagando hospital and Katwe Health center III.
Mr Kamusede Masereka, the Katwe Health Center III focal person, confirmed the incident and said they are waiting for the final results from the Uganda Virus Research Institute in Kampala where the samples were taken to ascertain the cause of the death.
Roya’s correspondent reported that 15 people suffered from food poisoning, after eating shawarma on Friday.
According to 24 News, 16 people in Wood County have come down with E. coli in the past week, prompting the health department to begin investigating. From 2016 to 2020 the county only saw 27 cases altogether.
“Even a case or two is something we want to identify and respond to quickly so that if it is, in fact, something that could spread to others we have a chance to stop it,” said Benjamin Robison, the health commissioner for the Wood County Health Department.
Those who have fallen ill range from ages 13 to 60 years old and those who contract the virus can experience different levels of sickness and gastrointestinal symptoms.
The Wood County Health Department has sent lab samples to the Ohio Department of Health to learn whether or not the illnesses are connected. Results, and more information, are expected early next week.
“We are doing a comprehensive investigation to understand what the cause of this was. Until we know whether these diseases are being caused by the same strain, we really have to wait to understand what our next steps are going to be,” Robison said.
Posted in Decontamination Microbial, E.coli, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology Blog, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak