Archives
-
Join 346 other subscribers
KSWFoodWorld
Blog Stats
- 448,579 Views

Posted in Campylobacter, Campylobacter jejuni, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk
Reported by Mr. Kenneth Yung, Research Officer,
Risk Assessment Section, Centre for Food Safety
Fish is an important part of many types of cuisine that we savour. However, the consumption of fish and fish products containing high level of histamine may cause scombrotoxin fish poisoning (SFP), also called histamine poisoning. In Hong Kong, the Centre for Health Protection of the Department of Health recorded a total of 26 local SFP cases, affecting 45 persons from 2009 to 2018. In this article, we discuss how histamine is formed and the ways to control level of histamine in fish and fish products..

Examples of fish which contain elevated levels of naturally occurring histidine: (a) mackerel, (b) sardine, (c) tuna and (d) anchovy. Some of their respective products have also been found to contain high levels of histamine.
Histamine is a toxic metabolite produced by histamine-producing bacteria during spoilage and fermentation of fish and fish products. Many histamine-producing bacteria are part of the natural microflora of the skin, gills and gut of freshly caught fish. Histidine decarboxylase (HDC) enzymes, synthesized by histamine-producing bacteria when they multiply, convert the amino acid histidine that are naturally present in fish into histamine.
The level of histamine in fish and fish products mainly depends on species of fish and time-temperature control. Certain fishes like mackerel, sardine, tuna and anchovy naturally contain high amount of histidine and have been associated with SFP cases in Hong Kong and/or other places.
Time and temperature control is the most effective method for ensuring food safety for fish species prone to histamine production. In the absence of proper time-temperature control such as refrigeration and freezing, formation of histamine may occur at any point throughout the supply chain. Previous study conducted jointly by the Food and Environmental Hygiene Department and the Consumer Council revealed that high levels of histamine (up to 2600 mg/kg) that can cause SFP were detected in opened canned fish samples that were left at room temperature for 24 hours. However, histamine was not detected in samples that were kept at 2°C for up to 168 hours.
SFP is caused by the ingestion of food containing high levels of histamine i.e. consuming a serving size of 250g fish or fish product with histamine level exceeding 200 mg/kg may cause symptoms in healthy individuals. Symptoms of SFP include tingling and burning sensation around the mouth, facial flushing and sweating, nausea, vomiting, headache, palpitations, dizziness and rash. Exacerbation of asthma and more serious cardiac manifestations were reported in more severe cases. The onset of symptoms is within a few hours after consumption and these symptoms will normally disappear in 12 hours without long term effect.
High levels of histamine can build up in fish and fish products before any signs of spoilage (e.g. bad smell or taste) develop. Therefore, measures for control of histamine should be taken along the food chain from harvest to consumption.
Care should be taken that the cold chain is maintained at or below 4°C along the supply chain, including points of transfer such as offloading of fish from the vessel and processing procedures. Frozen fish and fish products should be kept at or below -18°C. Transport vehicles or vessels should be adequately equipped to keep fish cold and pre-chilled before loading fish where applicable. Adequate heat treatment (e.g. cooking, hot smoking) can kill histamine-producing bacteria and inactivate HDC enzymes, but cannot destroy pre-formed histamine. Recommendations in the Code of Practice for Fish and Fishery Products (CAC/RCP 52-2003), issued by Codex Alimentarius Commission, should be observed to ensure food safety.
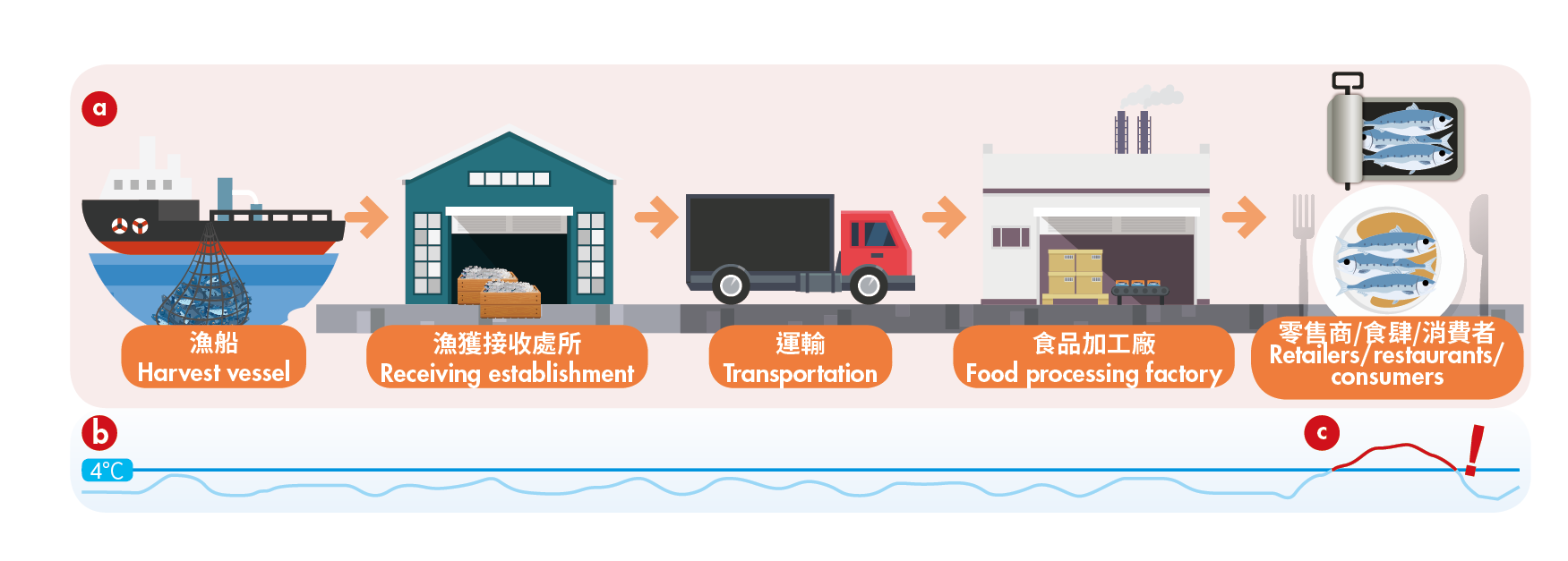
(a) Cold chain should be maintained throughout the whole supply chain. (b) Refrigerated fish and fish products should be kept at or below 4°C. (c) The time which fish products are kept under ambient temperature should be minimised.
At the consumer level, fish should be chilled rapidly after purchase. For pre-packaged fish and fish products, store according to the instructions of the manufacturer (e.g. keep refrigerated). If cooked fish and ready-to-eat fish products (e.g. tuna fish sandwiches and opened canned fish) are placed at room temperature all day long, they can be re-contaminated and histamine can form. Therefore, if these foods are not being eaten immediately, they should be kept under refrigeration and be finished as soon as possible.
Posted in CFS, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Histamine, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Scombroid, scombroid poisoning
A Salmonella contamination incident cost candy producer Barry Callebaut $77 million, according to the company’s full-year results.
The impact of the problem was CHF 76.9 million Swiss Francs ($77.3 million) in the fiscal year 2021/22, which ended on Aug. 31, 2022.
The Salmonella incident at the Wieze factory in Belgium and temporary production stoppage, followed by a gradual ramp-up toward the end of the fiscal year, had a “notable impact” on volume and profit in Europe, the Middle East, and Africa region. There was a loss because operations were paused at the factory.
As of October, cleaning of the factory was nearing completion and it began operating again at normal capacity after production was stopped in late June.
Posted in Decontamination Microbial, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Salmonella, Salmonella in Chocolate
At least 90 people have been affected and three have died in a major Listeria outbreak in Italy.
The Ministry of Health (Ministero della Salute) said the most recent patient was reported in mid-September.
Deaths occurred in December 2021 and March and June 2022 in Lombardy, Piedmont, and Emilia Romagna. The patients were immunocompromised or particularly vulnerable to infection. One woman lost her baby in the outbreak.
Patients live in Piedmont, Lombardy, Veneto, Emilia Romagna, Liguria, Umbria, Tuscany, Calabria, Lazio, Puglia, Valle D’Aosta and Abruzzo.
Posted in Decontamination Microbial, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, Foodborne Illness Death, foodborne outbreak, foodbourne outbreak, Illness, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak
Nestlé reportedly found E. coli in flour at the Buitoni pizza factory in France linked to a fatal outbreak this year back in August 2021.
French TV programme Envoyé Spécial has claimed an internal document shows the bacteria was picked up in flour at the Caudry site seven months before the Swiss giant recalled almost 1m pizzas and halted production.
Around fifty children fell sick, cases that have been linked to eating Buitoni Fraîch’Up pizzas. Two children died.
A norovirus outbreak sickened 173 people at D. C. Cobb’s restaurant in McHenry, Illinois in August 2022, according to an investigation by the McHenry County Department of Health (MCDH). Two of those patients were hospitalized. The last time this investigation was updated was on September 16, 2022, when it was reported that 16 people were sick after eating at that restaurant. The restaurant is located at 1204 North Green Street in McHenry.
Posted in Decontamination Microbial, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Virus, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Norovirus, outbreak, Virus
Posted in Aflatoxin, Aflatoxin B1, Animal Feed Mould Toxin, Aspergillus Toxin, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Toxin, Fusarium Toxin, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Mold Toxin, Mould Toxin, Mycotoxin, Ochratoxin, Ochratoxin A, Pet Food Aflatoxin, Research, Toxin
Between 18 August and 13 October 2022, five cases of Listeria monocytogenes have been registered at the Statens Serum Institut . The Statens Serum Institut, the Danish Veterinary and Food Administration and the Norwegian Food Institute DTU are investigating the disease outbreak.
Between 18 August and 13 October 2022, the Statens Serum Institut registered five people who are infected with the same type of Listeria monocytogenes (figure 1). Among the sick are 2 men and 3 women. The patients are between 6-83 years old (median age is 75 years). The patients are infected throughout the country (table 1).
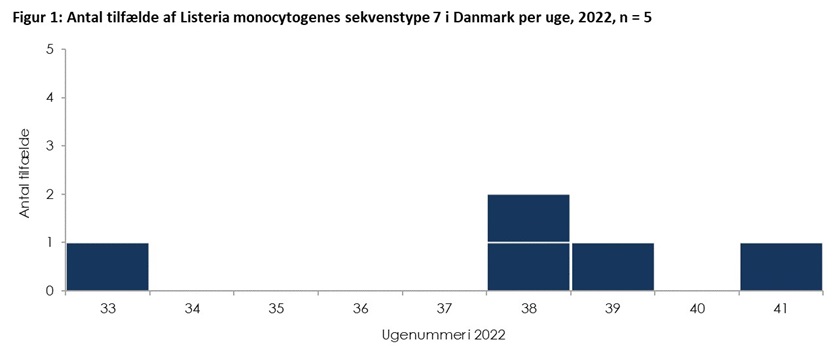
Table 1. Patients with the same type of Listeria monocytogenes in Denmark, August to October 2022, per region (n=5)
Region |
Number of patients |
| The capital | 1 |
| Central Jutland | 1 |
| Northern Jutland | 0 |
| Zealand | 1 |
| Southern Denmark | 2 |
| Total | 5 |
The outbreak is handled by the Central Outbreak Group, which consists of SSI, the Danish Veterinary and Food Administration and the DTU Food Institute. SSI stands for whole-genome sequencing of listeria isolates from the patients and interviews with patients or relatives with a view to identifying a possible source of infection.
The bacteria is of the type Listeria monocytogenes . By whole-genome sequencing of the Listeria monocytogenes bacteria isolated from the patients, it can be seen that they are very closely related and belong to sequence type 7.
Posted in Decontamination Microbial, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak
In winter, an increase in norovirus cases can be expected, as the infection is called the winter plague in some languages (eg vinterkräksjuka in Swedish). The main symptoms of norovirus infection are malaise, vomiting, diarrhea, fever and abdominal pain.
The virus is highly contagious and only a few viruses are needed to cause infection. Noroviruses can be transmitted through food from people who are ill or have recently been ill with norovirus. There are examples of norovirus being transmitted through food in Iceland and abroad, such as frozen raspberries, oysters and food from restaurants. Such infections can cause group infections.
For example, the consumption of frozen raspberries caused a widespread norovirus infection in Denmark a few years ago. Subsequently, the Danes established rules that frozen raspberries should be heated before consumption, and such instructions can often be seen on packaging.
But how can the virus be prevented from spreading to food at home, in canteens, restaurants and other food businesses?
The risk of norovirus being transmitted through food can be reduced if these guidelines are followed.
Posted in Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Virus, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Norovirus, Research, Virus
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Raw Milk, raw milk cheese, STEC, STEC E.coli