Cases of TIAC suspected of being linked to the consumption of raw shellfish in mainland France have been reported since December 2019.
A collective food poisoning (TIAC) is defined by the appearance of at least 2 cases of illness with a similar symptomatology, generally gastrointestinal, the cause of which can be related to the same food or meal. Any person (doctor, manager of collective catering establishments, consumer, etc.) who is aware of an episode that may be a TIAC, must declare this suspicion of TIAC to the administration (Regional Health Agency (ARS) and / or the Departmental Directorate (for social cohesion) and for the protection of populations (DD (CS) PP). This declaration involves local information from the other structure (ARS or DD (CS) PP).
Since the beginning of December 2019, 179 compulsory declarations (DO) of collective food poisoning (TIAC) suspected of being linked to the consumption of raw shellfish, mainly oysters, have been sent to Santé publique France. The reports come from the majority of regions in mainland France (see Figure 1).

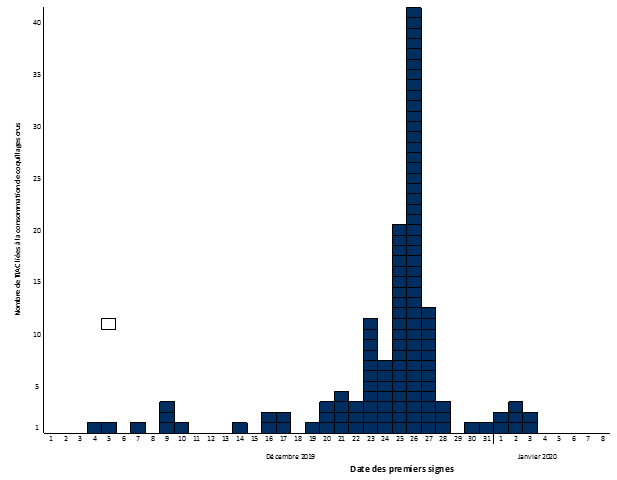
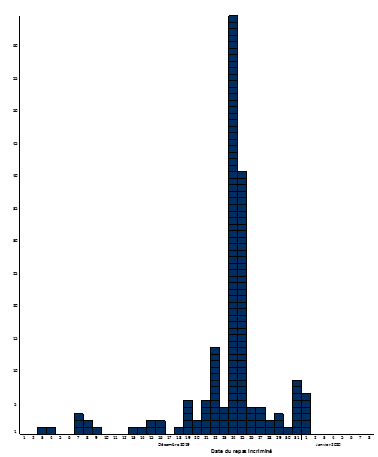
The vast majority (138/179, 77%) of these TIAC occurred from December 23 (Figures 2 and 3). A peak of patients is observed around December 25-27 (Figure 2). The offending meals are grouped around December 24-25 (Figure 3).
A total of 1,033 people were sick, of whom 21 (2%) were hospitalized. Most of them are people over the age of 15. Of the 595 patients with age information, 19 (3.1%) were children under the age of 15. The symptoms, mainly diarrhea and vomiting, as well as the incubation times, are compatible with infections with norovirus or other enteric viruses. Stool tests performed to date by the National Reference Center for Gastroenteritis Viruses have confirmed the presence of norovirus and other enteric viruses.
The number of TIAC suspected of being linked to the consumption of raw shellfish is significantly higher than in previous years. Each year between 25 and 120 TIAC suspected of being linked to the consumption of shellfish are reported to Public Health France, of which between 4 and 30 occurred during the December-January periods.
Following reports from TIAC suspected of being linked to the consumption of raw shellfish, the Directorate General for Food (DGAL) in conjunction with the Departmental Directorates in charge of protecting populations (DD (CS) PP) is carrying out an investigation traceability in order to trace back to the production area for suspected shellfish and confirmation analyzes are carried out on the areas concerned. To date, several areas have been closed due to contamination by noroviruses. Zone closings can be viewed on this site:
http://www.atlas-sanitaire-coquillages.fr/ (“Statutes” section)




