Main points for 2019
The main points of the 2019 report are:
1. A total of 539 confirmed cases of Shiga toxin-producing Echerichia coli (STEC) O157 were reported in England and Wales in 2019.
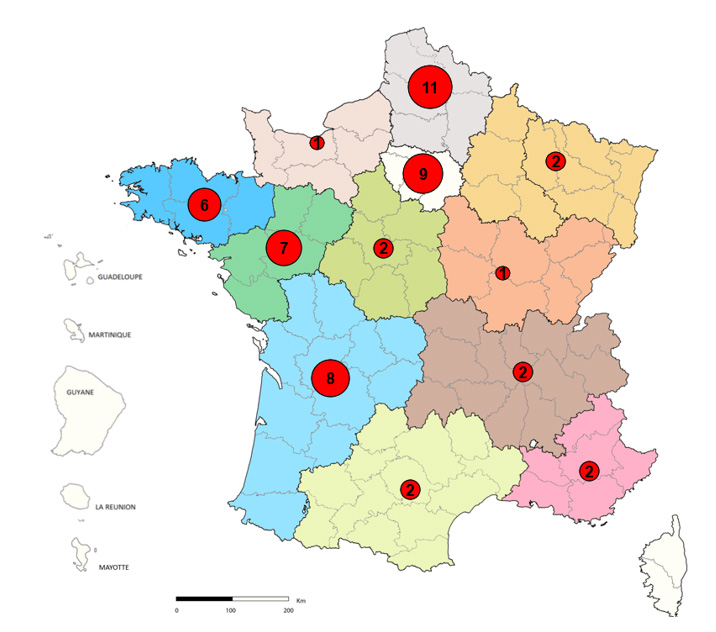
2. The lowest incidence of STEC O157 was in the East Midlands region (0.56 per 100,000 population) and the highest in the Yorkshire and Humber region (1.51 per 100,000 population).
3. Children aged 1 to 4 years had the highest incidence of infection (3.28 per 100,000 population, CI 95% 2.63–4.04).
4. Nearly one-third of confirmed STEC O157 cases in England were hospitalised and 3% were reported to have developed haemolytic ureamic syndrome (HUS).
5. In England and Wales, detection of non-O157 STEC increased in line with the growing number of NHS labs implementing gastrointestinal (GI) diagnostics using polymerase chain reaction (PCR); in 2019, 768 culture-positive non-O157 STEC cases (655 in England, 113 in Wales) were reported.
6. A further 347 specimens in England and 66 in Wales were positive for Shiga toxins (stx) genes on PCR at the Gastrointestinal Bacteria Reference Unit (GBRU) but an organism was not cultured.
7. The most commonly isolated non-O157 STEC serogroup was STEC O26 (England: n=109/655, 17% and Wales: n=28/113, 25%).
8. Five outbreaks of STEC involving 65 cases in England were investigated in 2019.
Cases of STEC in England and Wales in 2019
In 2019, 1,720 confirmed cases of STEC were reported in England and Wales; these comprised 539 culture-confirmed cases of STEC serogroup O157 (515 cases in England and 24 in Wales) and 768 cases (655 in England, 113 in Wales) where a serogroup other than O157 was isolated (non-O157). For a further 413 cases, samples were confirmed as STEC by testing positive by PCR for stx genes, but STEC was not cultured (347 in England, 66 in Wales).
Five confirmed cases were infected with multiple serogroups:
- O157 and O26
- O26 and O103
- O76 and O113
- O91 and O128ab
- O146 and O91
There were 13 probable cases with serological evidence of STEC infection, with antibodies detected to O157 lipopolysaccharides in 11 cases (England: 10, Wales: 1), for O111 lipopolysaccharides in one case, and for O26 lipopolysaccharides in another case.
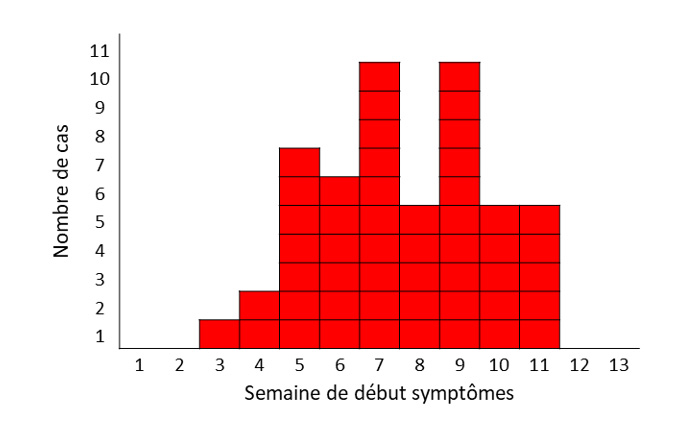
The crude incidence rate of confirmed STEC O157 in England and Wales was 0.91 per 100,000 cases (95% CI 0.83–0.99), continuing the downward trend observed since 2015 (Figure 1). It is the lowest number of cases reported annually since 1996, when testing began in England for STEC O157 on all faecal specimens from patients with suspected gastrointestinal infection (7).
Non-O157 STEC cases in England and Wales
Historically, cases of non-O157 STEC have been under ascertained, with 89 cases of STEC non-O157 reported between 2009 and 2013, prior to PCR being implemented.
Following the increase in recent years in frontline laboratories using PCR, there has been a significant increase in the detection of non-O157 STEC in England. It is not possible to estimate a denominator for incidence calculations for non-O157 STEC because details of contract arrangements for referral of samples from primary care and catchment areas of each diagnostic laboratory using PCR are not known.
In 2019, of 5,760 samples received at GBRU for STEC testing, 1,002 non-O157 STEC cases were confirmed in England. Of the 1,002 non-O157 cases, 655 culture positive cases of 72 different serogroups were confirmed. For 21 isolates, a serotype could not be identified as the genes encoding the somatic O antigen did not match any known sequence in the database. Specimens for a further 347 cases in England were positive for stx genes on PCR at GBRU but an organism was not cultured (PCR positive-culture negative).
In Wales, 113 non-O157 cases of 40 different serotypes were confirmed and a further 66 were PCR positive-culture negative. The most common non-O157 serogroups isolated in 2019 were O26 (28/113, 25%), O146 (15/113, 13%), O128ab (10/113, 9%) and O91 (8/113, 7%) followed by O111 (4/113, 4%), O113 (4/113, 4%) and O156 (4/113, 4%).