Archives
-
Join 346 other subscribers
KSWFoodWorld
Blog Stats
- 451,349 Views
Category Archives: Microbiology Risk
Research – Lactic Acid Bacteria and Bacteriocins: Novel Biotechnological Approach for Biopreservation of Meat and Meat Products
Meat and meat products are perishable in nature, and easily susceptible to microbial contamination and chemical deterioration. This not only results in an increased risk to health of consumers, but also causes economic loss to the meat industry. Some microorganisms of the lactic acid bacteria (LAB) group and their ribosomal-synthesized antimicrobial peptides—especially bacteriocins—can be used as a natural preservative, and an alternative to chemical preservatives in meat industry. Purified or partially purified bacteriocins can be used as a food additive or incorporated in active packaging, while bacteriocin-producing cells could be added as starter or protective cultures for fermented meats. Large-scale applications of bacteriocins are limited, however, mainly due to the narrow antimicrobial spectrum and varying stability in different food matrixes. To overcome these limitations, bioengineering and biotechnological techniques are being employed to combine two or more classes of bacteriocins and develop novel bacteriocins with high efficacy. These approaches, in combination with hurdle concepts (active packaging), provide adequate safety by reducing the pathogenicity of spoilage microorganisms, improving sensory characteristics (e.g., desirable flavor, texture, aroma) and enhancing the shelf life of meat-based products. In this review, the biosynthesis of different classes of LAB bacteriocins, their mechanism of action and their role in the preservation of meats and meat products are reviewed.
Posted in Bacteriocin, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk
Mycotoxins – New EU maximum limits for Ochratoxin A in certain foodstuffs
On August 8th was published the Commission Regulation (EU) 2022/1370 of 5 August 2022 amending Regulation (EC) No 1881/2006 as regards maximum levels of Ochratoxin A in certain foodstuffs.
Ochratoxin A (OTA) is a naturally occurring foodborne mycotoxin produced by various fungi of the genus Aspergillus and Penicillium, and it can be found in a wide variety of agricultural commodities, such as grains, seeds and beans, dried fruits, spices, and roots.
OTA is formed during sun drying and storage of crops, and, due to its stability under moderate heating, it can persist along the food production chain. However, losses ranging up to 90% have been observed at temperatures above 180°C.
Several toxic effects associated with OTA have been reported over the years.
The International Agency for Research on Cancer has included OTA in its Group 2 carcinogens, due to its kidney carcinogenicity, even if the mechanisms of genotoxicity are still unclear.
In 2006 the European Food Safety Authority performed a first risk assessment for OTA. In agreement with this assessment, the European Commission established in Regulation (EC) 1881/2006 maximum admissible levels of OTA for human consumption in many foodstuffs, such as cereals, coffee, grapes, grapefruit, dried vine fruits, wine, spices, and liquorice.
In recent years, further findings of high levels of Ochratoxin A were observed in food products for which no maximum levels were set at EU level, this raised questions regarding the necessity of setting new maximum levels for OTA in these foods.
In May 2020, EFSA published a revision of the OTA risk assessment, taking into account the new scientific evidence.
Based on this new risk assessment, the EU Commission established the Regulation (EU) 2022/1370, which revised the maximum levels for OTA present in Regulation (EC) 1881/2006 as follows:
• setting a maximum level for foods not yet included that contribute to human exposure to OTA;
• setting a level for non-alcoholic malt beverages and date syrup, pending the determination of a link with the OTA content of malt and dates;
• reducing the levels already set in certain foods (e.g. bakery products, dried vine fruit, roasted coffee and soluble coffee);
• the existing provisions for ochratoxin A in certain spices has been broadened to all spices.
For cheese and ham, it has been established that additional monitoring on the presence of ochratoxin A is appropriate before the setting of maximum levels.
The new Regulation will enter into force on the 28th of August 2022 and it shall apply from 1 January 2023.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Toxin, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Mould Toxin, Mycotoxin, Ochratoxin, Ochratoxin A, OTA
Research – Salmonella Typhimurium outbreak associated with frozen tomato cubes at a restaurant in western Finland, January to February 2021
On 2 February 2021, a local environmental health authority in western Finland notified the National Registry for Food and Waterborne Outbreaks about six cases of Salmonella infection suspected to be related to a local lunch restaurant in a region where there had been between one and three salmonellosis cases per month. More cases were soon discovered that were linked to food eaten at the same restaurant on the days 27–29 January 2021, and the Finnish Institute for Health and Welfare (THL) was informed of 44 outbreak-related cases. The estimated number of potentially exposed persons was 400. THL and the Finnish Food Authority joined the local outbreak investigation team to support and coordinate the epidemiological and microbiological investigations.
We report here a food-borne outbreak caused by a non-monophasic multidrug-resistant S. Typhimurium strain that was not detected in Finland before.
Posted in food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak
Research – Impregnation of the French population by mycotoxins. National Biomonitoring Program, Esteban 2014-2016

Mycotoxins are substances secreted by certain toxigenic strains of several species of molds (microscopic fungi) such as Aspergillus, Penicillium, Fusarium, Byssochlamys, Alternaria etc. which in particular contaminate cereals and plants before and or after harvest.
The toxicity of mycotoxins depends on the species and the nature of the toxin. They are generally thermostable, resistant to transformation processes and can be found in many foodstuffs and be responsible for acute or chronic poisoning in humans or animals.
Of the 300 to 400 known mycotoxins, about ten of them can cause animal or human pathologies: aflatoxins (AF), ochratoxin A (OTA), fumonisins deoxynivalenol (DON), T-2 and HT-2 toxins, trichotecenes (TC), zearalenone (ZEN) and patulins which contaminate fruits, especially apples. In 1993, the IARC (International Agency for Research on Cancer) classified aflatoxins in group 1, carcinogenic to humans; AFB1, considered one of the most potent natural genotoxic carcinogens, is classified in group 1 (IARC, 2002).
The target organ is the liver. As for OTA, it is considered possibly carcinogenic for humans and classified in group 2B (1993); in humans as in animals, the kidney is the main target organ. OTA would also have immunotoxic and neurotoxic effects. Due to their harmful effects, exposure to mycotoxins must remain as low as possible to protect the population. L’ WHO encourages the monitoring of mycotoxin levels in food because they represent a risk for human and animal health.
In France, data on the impregnation of the French population by mycotoxins are almost non-existent, with the exception of a study carried out in three French regions [1, 2]. The Esteban cross-sectional study (Health study on the environment, biomonitoring, physical activity and nutrition) made it possible to measure the levels of impregnation by aflatoxins and OTA of the population in mainland France aged 6 at 74 years old between April 2014 and March 2016.
The purpose of this note is to present the results of impregnation by AFs and OTA, and to analyze the determinants of exposure to OTA in adults . Aflatoxins B1, B2, G1, G2, M1 were not quantified, neither in children nor in adults. For OTA, the percentage of quantification was equal to 45.5% in children and 47.8% in adults. The geometric means of the levels of impregnation by the OTA were lower than the LOQ or not provided considering the important rate of censorship.
The search for the determinants of exposure by OTA, essentially dietary, in adults showed an increase in impregnation with the consumption of processed meats. Not all associations could likely be identified due to small sample size. A future biomonitoring study could make it possible to deepen the search for determinants of the impregnations observed and to broaden the knowledge of the
Author: Oleko Amivi, Hoang Phan, Fillol Clémence, Gane Jessica, Saoudi Abdessattar, Zeghnoun Abdelkrim
Year of publication: 2022
Pages: 35 p.
Collection: Studies and Surveys
Posted in Aflatoxin, Aflatoxin B1, aflatoxin m1, Animal Feed Mould Toxin, Aspergillus Toxin, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Toxin, Fusarium Toxin, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Mold Toxin, Mould Toxin, Mycotoxin, Ochratoxin, Ochratoxin A, Research, Toxin
Canada – Shigella outbreak in Edmonton Zone
EDMONTON – Alberta Health Services (AHS) is notifying the public about an ongoing investigation into a Shigella outbreak in the Edmonton Zone.
In August of this year, AHS identified a cluster of Shigella cases among the inner city population of Edmonton.
To date, we have identified 87 people with Shigella, 64 of those people required hospitalizations. The first person became ill on August 17, 2022. No deaths have been reported connected to this outbreak.
Shigella is a disease that’s commonly associated with diarrhea, as well as fever, nausea and stomach cramps. It can cause severe illness, resulting in hospitalization and it spreads when someone comes into contact with fecal matter from an infected person and also by eating food contaminated with the bacteria.
AHS has reached out to physicians and inner city shelters and partners to advise them of the situation and has provided advice for helping reduce the spread of illness while also ensuring that anyone who requires medical attention receives the care they need.
A task force led by AHS with representation from the City of Edmonton, Alberta Health, Alberta Community and Social Services, Edmonton area shelters and other partner organizations has been created with the goal of sharing resources and support to help stop the spread of this bacteria.
The majority of the cases to date are within the city’s inner city population, so the risk to the general public remains low. However, we would like to remind people that proper hand hygiene helps to prevent the spread of many illnesses, including Shigella.
Anyone experiencing symptoms that might be related to Shigella or anyone with questions or concerns about their health is encouraged to speak with their healthcare provider or call Health Link at 811.
Alberta Health Services is the provincial health authority responsible for planning and delivering health supports and services for more than four million adults and children living in Alberta. Its mission is to provide a patient-focused, quality health system that is accessible and sustainable for all Albertans.
RASFF Alerts – Animal Feed – Mold/Mould – Sunflower Meal – Complementary Feed for Horses
Mould in complementary feed to horses in Sweden
Mold – post-extraction sunflower meal from Ukraine in Poland
Posted in Animal Feed, Animal Feed Mould Toxin, Animal Feed Testing, Decontamination Microbial, Food Micro Blog, Food Microbiology Blog, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, RASFF
RASFF Alerts – Animal Feed – Enterobacteriaceae – Dog Chews
High count of Enterobacteriaceae in dog chews from China in Sweden
Too high count of Enterobacteriaceae in dog chews from Turkey in Germany
Enterobacteriaceae in dog chews from Turkey in Germany
Posted in Animal Feed, Animal Feed Salmonella, Animal Feed Testing, Decontamination Microbial, Enterobacteriaceae, Food Micro Blog, Food Microbiology Blog, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Pet Food, Pet Food Enterobacteriaceae, Pet Food Testing
RASFF Alerts – Animal Feed – Salmonella – soy Cake – Soya Bean Meal – Poultry Meal – Lamb Meal
Salmonella in organic soy cake in Denmark and Sweden
Salmonella Orion in Soya bean meal, gmo from Germany in Switzerland and Finland
Salmonella in poultry meal from Germany in Belgium
Salmonella in lamb meal from Italy in the Czech Republic
Posted in Animal Feed, Animal Feed Salmonella, Animal Feed Testing, Food Micro Blog, Food Microbiology Blog, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Pet Food, Pet Food Salmonella, Pet Food Testing, RASFF
USA – Outbreak Investigation of Salmonella: Seafood (October 2022)
The FDA, along with CDC and state and local partners, is investigating a multistate outbreak of Salmonella Litchfield infections linked to fresh, raw salmon supplied to restaurants in California and Arizona by Mariscos Bahia, Inc.
Based on epidemiologic information provided by CDC and interviews conducted by state and local public health officials, of 16 people interviewed, 12 reported eating sushi, sashimi, or poke. Of those interviewed, 11 people remembered details about the type of fish consumed and 9 report eating raw salmon before getting sick. The FDA’s investigation traced the distribution of fresh, raw salmon back to Mariscos Bahia, Inc.
In addition, the FDA collected an environmental sample that included multiple swabs at Mariscos Bahia, Inc. (Pico Rivera, CA). Multiple environmental swabs collected at the facility are positive for Salmonella and subsequent Whole Genome Sequencing (WGS) analysis is ongoing. The WGS completed to date indicates the Salmonella detected in at least one of the swabs from the facility matches the outbreak strain. While epidemiological evidence indicates that ill people consumed fresh, raw salmon processed at this firm, the presence of Salmonella in the processing environment indicates that additional types of fish processed in the same area of the facility could also be contaminated which includes fresh, raw halibut, Chilean seabass, tuna, and swordfish. Salmon, halibut, Chilean seabass, tuna, and swordfish processed in Marisco Bahia Inc.’s Pico Rivera, CA, facility could have also been sent to the Mariscos Bahia, Inc. facilities in Phoenix, AZ and then sent to restaurants.
The firm is cooperating with the FDA investigation and has agreed to initiate a voluntary recall. As a part of the firm’s voluntary recall, the firm will contact its direct customers who received recalled product.
The FDA’s investigation is ongoing. Updates to this advisory will be provided as they become available.
Recommendation
According to Mariscos Bahia, Inc., seafood was only sold directly to restaurants in California and Arizona and would not be available for purchase by consumers in stores.
Restaurants should check with their suppliers and not sell or serve salmon, halibut, Chilean seabass, tuna, and swordfish received fresh, not frozen from Mariscos Bahia, Inc. (Pico Rivera, CA and Phoenix, AZ) on or after June 14, 2022. If restaurants received these fish and then froze it, they should not sell or serve it. Restaurants should also be sure to wash and sanitize locations where these fish from Mariscos Bahia, Inc. were stored or prepared.
Consumers eating salmon, halibut, Chilean seabass, tuna, and swordfish at a restaurant in California or Arizona should ask whether the fish is from Mariscos Bahia, Inc and was received fresh, not frozen.
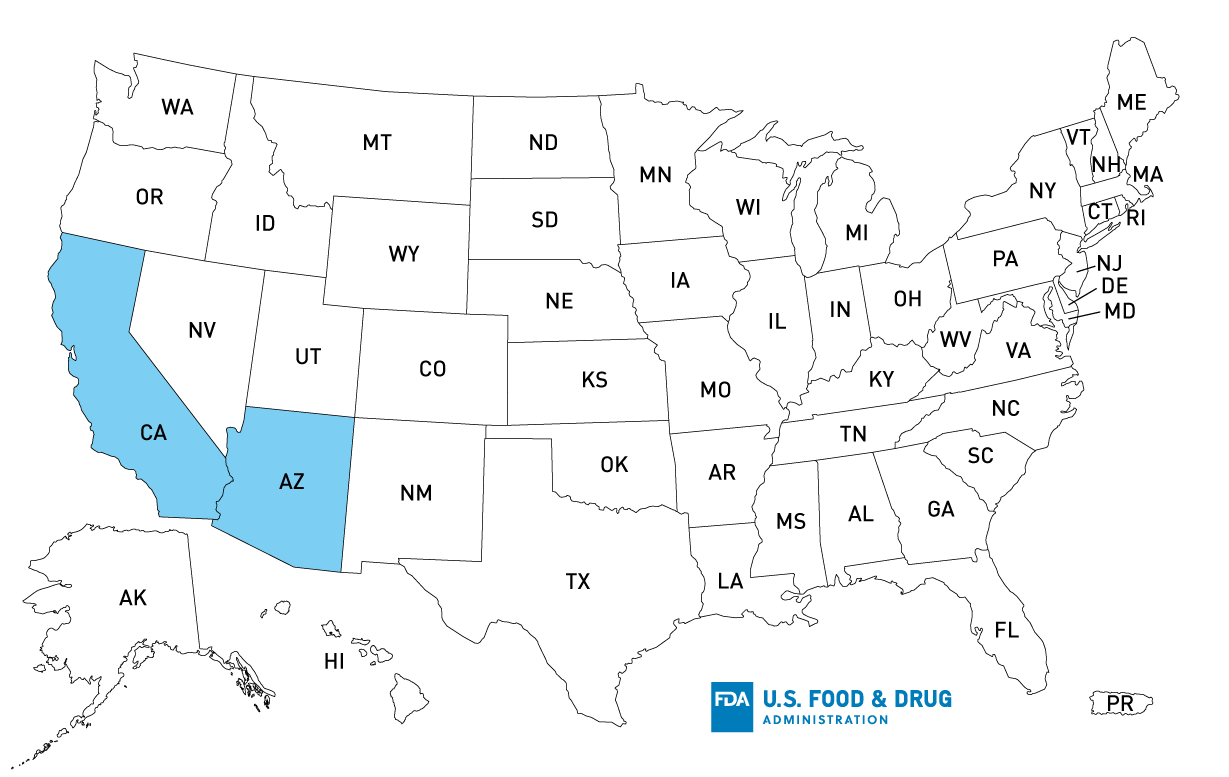
Map of U.S. Distribution
Case Count Map Provided by CDC
Case Counts
Total Illnesses: 33
Hospitalizations: 13
Deaths: 0
Last illness onset: September 18, 2022
States with Cases: AZ (11), CA (21), IL (1)
Product Distribution*: AZ, CA
*Distribution has been confirmed for states listed, but product could have been distributed further, reaching additional states
Posted in CDC, Decontamination Microbial, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Salmonella, WGS
USA – FDA Core Outbreak Table
What’s New
- For the outbreak of E. coli O121:H19 linked to Frozen Falafels (reference #1115), FDA has initiated traceback and sample collection and analysis.
- For the outbreak of E. coli O157:H7 in an unidentified product (reference #1081), the FDA investigation has closed.
- For the outbreak of Salmonella Senftenberg in an unidentified product (reference #1087), the case count has increased from 33 to 34 cases.
- For the outbreak of Cyclospora cayetanensis in an unidentified product (reference #1084), the case count has increased from 42 to 43 case.
Posted in Cyclospora, Cyclosporiasis, Decontamination Microbial, E.coli O121, E.coli O157, E.coli O157:H7, FDA, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Salmonella