FDA
The FDA and CDC, in collaboration with state and local partners, have completed the investigation on two of three multistate outbreak of E. coli O157:H7 infections in the U.S. this fall.
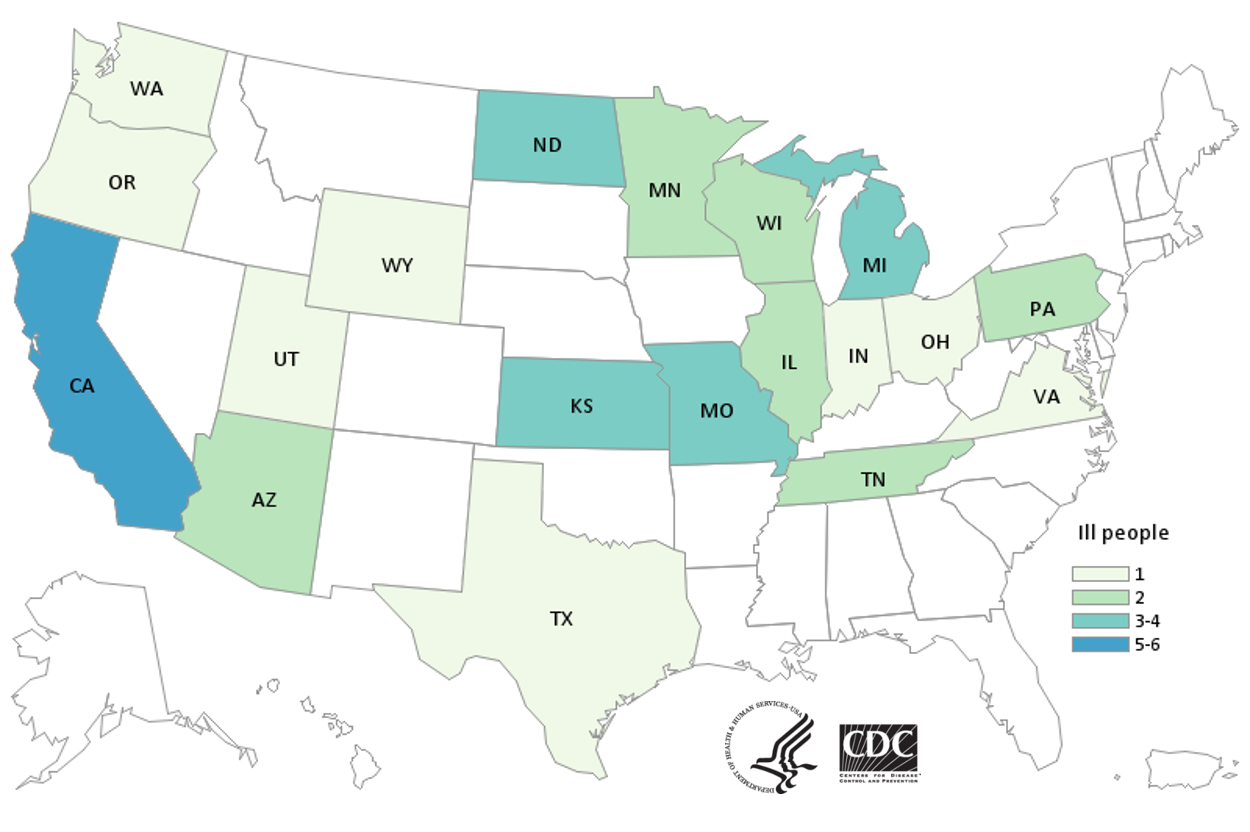
One of these investigations, Outbreak Unknown Source 3, identified 18 reported illnesses in nine states: California, Colorado, Illinois, Michigan, New York, Ohio, Pennsylvania, Virginia, Washington.
FDA completed a traceback investigation of several potential food vehicles identified in patient interviews and although no single farm was identified as a common source of the outbreak, FDA and state partners also conducted on-site investigations on farms of interest. However, information and samples collected in these inspections did not link these farms to the outbreak. The investigation of a farm does not mean that the farm is linked to an outbreak. The results of an investigation into a farm may well lead to that firm being ruled out of the investigation. On 12/18/2020, the CDC announced that this outbreak had ended.
The other completed outbreak investigation, Outbreak Unknown Source 1, identified 32 reported illnesses in 12 states: California, Illinois, Louisiana, Maryland, Michigan, Montana, New Jersey, Ohio, Utah, Virginia, Washington, Wisconsin. This strain of E. coli is genetically similar to a strain linked to a romaine outbreak that occurred in the spring of 2018, though a food was not linked to the current outbreak. FDA completed a traceback investigation and was unable to determine a common source of the outbreak. FDA and state partners also conducted on-site inspections on farms of interest, though information collected in these inspections did not link these farms to the outbreak. On 12/18/2020, the CDC announced that this outbreak had ended.
Investigations of a third E. coli outbreak of Unknown Source 2 continue.
Recommendation
Consumers, restaurants, and retailers, were advised not to eat, sell, or serve recalled Tanimura & Antle, Inc. brand packaged single head romaine lettuce with a pack date of 10/15/2020 or 10/16/2020.
The recalled products are now well beyond expiration and likely no longer on the market or in consumers’ homes.