UKHSA

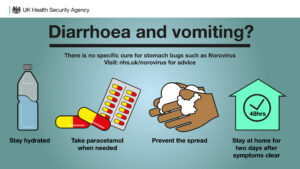
Norovirus, commonly known as the winter vomiting bug, is a stomach bug that causes sickness and diarrhoea. Following lower levels than normal throughout the COVID-19 pandemic, we have started to see an increase in norovirus activity as we head into the winter period.
Norovirus is able to spread easily through communities and so outbreaks are common in settings where individuals have close contact such as hospitals, care homes, schools and nurseries.
For most people this is an unpleasant, short-lived illness and they make a full recovery within 2-3 days without needing any medicine. However, some groups, including young children, the elderly or those with weakened immunity, are at risk of suffering more serious and prolonged illness which may require medical treatment.
Stopping the spread
Norovirus is easily transmitted through contact with people with the infection and any surfaces or objects which have been contaminated with the virus. Symptoms include sudden onset of nausea, projectile vomiting and diarrhoea but can also include a high temperature, abdominal pain and aching limbs.
The incubation period of norovirus is 12-48 hours, which is the time between catching the virus and developing symptoms. Individuals are most infectious when symptomatic, but it is possible to pass on norovirus or shed the virus, thereby contaminating surfaces, objects or even food, both before developing symptoms and after symptoms have stopped.
Good hand hygiene is important to stop norovirus spreading. To avoid catching norovirus or passing it on to others wash your hands frequently and thoroughly with soap and warm water. This is most important following an episode of illness, after using the toilet, before eating or preparing food as well as cleaning up vomit or diarrhoea. Alcohol-based hand sanitisers are not effective against norovirus.