Archives
-
Join 346 other subscribers
KSWFoodWorld
Blog Stats
- 443,896 Views
Category Archives: Food Microbiology Research
Research – Characterization of the Toxigenic Potential of Bacillus cereus sensu lato Isolated from Raw Berries and Their Products
Bacillus cereus is estimated to be responsible for 1.4–12% of all food poisoning outbreaks worldwide. The objective of this study was to investigate the toxigenic potential of 181 isolates of B. cereus previously recovered from different types of berries and berry products (strawberries, raspberries, blackberries, and blueberries) by assessing the presence of enterotoxin genes (hblA, hblC, hblD, nheA, nheB, nheC, and cytK) and an emetic toxin cereulide synthetase gene (ces). The cytotoxic activity on Caco-2 cells was also evaluated for the two isolates containing the gene cytK. Twenty-three toxigenic profiles were found. The nheABC (91.7%) and hblACD (89.0%) complexes were the most prevalent among the isolates, while the cytK and ces genes were detected in low percentages, 1.1% and 3.3%, respectively. In addition, the nheABC/hblACD complex and ces genes were detected in isolates recovered throughout the production process of blackberries and strawberries. The cytotoxic activity on Caco-2 cells was also observed to be greater than 60% for isolates containing the cytK gene.
Germany – Germs in food – food-borne infections and how to prevent them
One of the most common sources of food-borne infections is chicken meat contaminated with Salmonella or Campylobacter pathogens. How these pathogens can be reduced in the barn and further along the food chain to the consumer is one of the central topics at a symposium on zoonoses and food safety, which the Federal Institute for Risk Assessment (BfR) is organising in Berlin-Marienfelde on 16 and 17 November 2023. “The number of reported illnesses caused by foodborne infections alone in Germany amounts to around one hundred thousand per year, and the number of unreported cases is likely to be much higher,” says Professor Dr Karsten Nöckler, Head of the Biological Safety Division at the BfR. “In order to combat such infections effectively, we need to know where the germs come from, at which point in the production process the food is contaminated and, of course, how this can be prevented.”
In a joint project funded by the Federal Ministry of Food and Agriculture (BMEL), researchers are investigating whether the bacterial load of chicken meat can be reduced using thermal processes. Tests show that even a short immersion in hot water (> 70 degrees Celsius) reduces the number of Salmonella and Campylobacter by an order of magnitude. Treatments with icy air – at minus 90 degrees Celsius – also reduce the Campylobacter load. The scientists, who will present their findings at the symposium, conclude that such thermal processes can usefully supplement existing measures to reduce the microbiological load.
Other topics include the control of Vibrio spp. in aquaculture and the occurrence of infectious agents in wild animals. The scientific contributions are of particular interest against the background of the current zoonosis monitoring report, which will also be presented at the conference and will highlight current developments in the fight against foodborne infections.
Presentations by scientists from other institutions in Germany and Europe, for example on insects as food, E. coli bacteria in flour and the hygienic aspects of taking food from containers, round off the wide range of topics covered at the event.
The two-day symposium is aimed at interested parties from scientific institutions, investigation offices, monitoring authorities and industry from German-speaking countries. In addition to scientific training, it is also intended to promote networking between participants and thus co-operation between the various institutions. For this reason, the conference will be organised exclusively as a face-to-face event.
You can find the programme and a registration form here:
https://www.bfr-akademie.de/deutsch/veranstaltungen/szl2023.html
Journalists are cordially invited to attend. Please register in advance at pressestelle@bfr.bund.de
France – Duck leg – Listeria monocytogenes

- Product category Food
- Product subcategory Meats
- Product brand name Poultry stall
- Model names or references Duck leg 350g
- Product identification
GTIN Batch Date 20336370 0253035554 Use-by date 10/19/2023 20336370 0253035554 Use-by date 10/21/2023 20336370 0253035554 Use-by date 10/23/2023 - Start/end date of marketing From 07/10/2023 to 23/10/2023
- Storage temperature Product to keep in the refrigerator
- Health mark FR 53 014 002 EC
- Geographical sales area Some LIDL stores see list
- Distributors LIDL
- List of points of sale List_of_supermarkets_concerned_Corrected.pdf
Posted in food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, Food Quality, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Safety Regulations, Food Testing, Listeria, Listeria France, Listeria monocytogenes
Research – Hepatitis A Outbreaks linked to Frozen Fruit are a problem
Hepatitis A outbreaks associated with fresh, frozen, and minimally processed produce, worldwide, from 1983 to 2016—adapted and expanded from Sivapalasingam et al., 2004 and Fiore, 2004. Italics indicate instances where the food was locally sourced with respect to the cases. The implicated foods were raw unless listed otherwise.
See the table at the link above
Posted in food bourne outbreak, food contamination, food handler, Food Hazard, Food Hygiene, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Management, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Hepatitis A, Illness, outbreak
Research – USA -FDA -Cyclospora cayetanensis in Produce
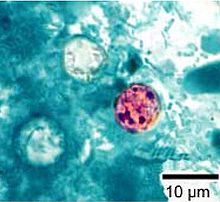
Executive Summary of Findings
Cyclospora cayetanensis (C. cayetanensis) is a coccidian protozoan parasite, belonging
to the phylum Apicomplexa, order Eucoccidiorida, family Eimeriidae, described between 1993 to 1994 as a newly identified human gastrointestinal pathogen.
Within the genus Cyclospora, only C. cayetanensis is known to infect humans. However, recent advances in genomics separated C. cayetanensis into 3 proposed species, with the two new proposed species also considered parasitic to humans (Cyclospora ashfordi sp. nov. and Cyclospora henanensis sp. nov.).
For the purpose of this document and to reflect the proposed status of the new
nomenclature “C. cayetanensis” refers to all three species of Cyclospora parasitic in humans.
The parasite produces oocysts that are resistant to harsh environmental conditions and many
chemical treatments commonly used to reduce the presence of bacterial pathogens in the
specialty crop production environment and in agricultural inputs (e.g., agricultural water). C.
cayetanensis is the etiologic agent of cyclosporiasis, its host range is limited to humans.
Detected in association with human illness in many parts of the world, C. cayetanensis
previously was considered to be a pathogen acquired during childhood in developing nations.
In the United States, cyclosporiasis was previously associated with international travel or
consumption of contaminated imported foods. In recent years, the U.S. has seen an increase in cases and positive samples associated with domestically grown produce, both as raw
agricultural commodities and fresh cut. Laborers with the history of recent travel to countries
where C. cayetanensis is endemic have not been ruled out as the sources of the pathogen in
these outbreaks. Since 2016, the number of cyclosporiasis cases has increased approximately
3-fold, often linked to the consumption of leafy herbs and ready-to-eat salads. Fecal
contamination from symptomatic or asymptomatic carriers is, ultimately, the only known source of C. cayetanensis. The hypothesis that C. cayetanensis has become endemic in the production regions of the U.S. remains to be robustly supported. The hypothesis that farm workers with a history of recent travel to areas where the parasite is common are the likeliest source of the pathogen has not been ruled out. C. cayetanensis likely spreads via the fecal-environment-oral route when sanitation controls break down. Efforts have been made to develop molecular detection methods for C. cayetanensis in both food and environmental samples.
However, due to the high degree of genome-level conservation between C. cayetanensis and its close relatives that are not pathogenic in humans, results of some environmental surveys that relied solely on the PCR-based detection of ribosomal RNA genes likely overestimated the prevalence of C. cayetanensis. There remain significant knowledge and data gaps that hamper the implementation of effective measures to prevent the contamination of produce with the oocysts of this parasite. Awareness of the factors that can contribute to C. cayetanensis contamination of domestically grown and imported produce is key to developing an effective prevention and management strategy.
What is ACOP L8 & What Does It Say About Controlling Legionella?

The Health and Safety Executive Approved Code of Practice L8 (ACOP L8) is a key document, offering essential direction and guidance to help business owners and those responsible for workplace safety manage the risks associated with legionella and Legionnaires’ disease.
In this guide the water safety specialists at Legionella Control International help to demystify the ACOP L8 to explain what it is, its special legal status, how to interpret it, and the role of the duty holder and responsible person.
A version of this guide to the HSEs ACOP L8 and how to interpret it first appeared in Legionella Control International’s newsletter. To get it in your inbox, sign up for free here.
Research – Safety Properties of Escherichia coli O157:H7 Specific Bacteriophages: Recent Advances for Food Safety
Abstract
Shiga-toxin-producing Escherichia coli (STEC) is typically detected on food products mainly due to cross-contamination with faecal matter. The serotype O157:H7 has been of major public health concern due to the severity of illness caused, prevalence, and management. In the food chain, the main methods of controlling contamination by foodborne pathogens often involve the application of antimicrobial agents, which are now becoming less efficient. There is a growing need for the development of new approaches to combat these pathogens, especially those that harbour antimicrobial resistant and virulent determinants. Strategies to also limit their presence on food contact surfaces and food matrices are needed to prevent their transmission. Recent studies have revealed that bacteriophages are useful non-antibiotic options for biocontrol of E. coli O157:H7 in both animals and humans. Phage biocontrol can significantly reduce E. coli O157:H7, thereby improving food safety. However, before being certified as potential biocontrol agents, the safety of the phage candidates must be resolved to satisfy regulatory standards, particularly regarding phage resistance, antigenic properties, and toxigenic properties. In this review, we provide a general description of the main virulence elements of E. coli O157:H7 and present detailed reports that support the proposals that phages infecting E. coli O157:H7 are potential biocontrol agents. This paper also outlines the mechanism of E. coli O157:H7 resistance to phages and the safety concerns associated with the use of phages as a biocontrol.
Research – Two successive outbreaks of acute gastroenteritis due to Norovirus GII.6 in a holiday camp house

Abstract
When two outbreaks occur in the same institution within a short period of time, an important health and social concern is generated. Two gastroenteritis outbreaks occurring a week apart in the same facility were reported in Lleida, Spain, in 2018. The objective of this study was to describe the clinical, epidemiological and microbiological investigation carried out and to determine the risk factors. Demographic data, food consumption and symptoms were collected. Health inspections of the facility were carried out. Risk ratio and their 95% confidence intervals were estimated for the implication of each food consumed. The attack rate was 89.7% in the first outbreak and 69.6% in the second outbreak. The most frequent symptoms in the first and second outbreak were abdominal pain (88.5% and 100%, respectively), vomiting (80.8% and 87.5%, respectively) and nausea (69.2% and 81.3%, respectively). The first outbreak was associated with the consumption of a salad and the second with a cheese omelet. Norovirus GII.6 was detected by RT-PCR and sequenced in both groups of students and in the food handlers who prepared the meals. These results highlight the importance of exclusion from work of food handlers with gastroenteritis, the adequate availability of mechanisms for correct hand washing and the correct cleaning of surfaces.
Posted in Food Microbiology Research, Norovirus, Research
Research – Survival of Foodborne Pathogens in Low and Nonalcoholic Craft Beer
Abstract
Breweries and beverage companies have recently been interested in creating innovative beer varieties that deviate from traditional beer styles, with either low-alcohol content <2.5% alcohol by volume (ABV) or the absence of alcohol altogether (<0.5% ABV). Traditional beers (up to 10% ABV) contain numerous intrinsic and extrinsic factors preventing pathogens from proliferation or propagation. Physiochemical properties such as a low pH, presence of ethanol and hop acids, limited oxygen, and specific processing techniques, including wort boiling, pasteurization, filtration, cold storage, and handling, all contribute to microbial stability and safety. The potential change or absence in one or more of these antimicrobial hurdles can render the final product susceptible to pathogen survival and growth. In this study, the effect of pH, storage temperature, and ethanol concentration on the growth or die-off of foodborne pathogens in low and nonalcoholic beers was evaluated. pH and ethanol concentrations were adjusted from their initial values of 3.65 and <0.50% ABV to pHs 4.20, 4.60, and 4.80; and 3.20 ABV, respectively. The samples were inoculated with individual five-strain cocktails of E. coli O157:H7, S. enterica, and L. monocytogenes, then stored at two different temperatures (4 and 14°C) for 63 days. Microbial enumeration was performed using selective agar with incubation at 35°C. Results showed that nonalcoholic beers allowed for pathogen growth and survival, as opposed to the low-alcoholic ones. E. coli O157:H7 and S. enterica grew approximately 2.00 log at 14°C, but no growth was observed at 4°C. L. monocytogenes was more susceptible and fell at, or below, the detection limit rapidly in all the conditions tested. The results show that storage temperature is critical in preventing the growth of pathogens. pH did not appear to have a significant effect on the survival of pathogens (p < 0.05). This challenge study demonstrates the need for beverage manufacturers to prioritize and maintain food safety plans along with practices specific to low- and nonalcoholic beer manufacturers.
Research – Unveiling Fresh-Cut Lettuce Processing in Argentine Industries: Evaluating Salmonella Levels Using Predictive Microbiology Models
Abstract
A survey was performed to gather information on the processing steps, conditions, and practices employed by industries processing ready-to-eat (RTE) leafy vegetables in Argentina. A total of seven industries participated in the survey. A cluster analysis of the data obtained was performed to identify homogeneous groups among the participating industries. The data collected were used as inputs of two predictive microbiology models to estimate Salmonella concentrations after chlorine washing, during storage and distribution of final products, and to rank the different practices according to the final estimated Salmonella levels. Six different clusters were identified by evaluating the parameters, methods, and controls applied in each processing step, evidencing a great variability among industries. The disinfectant agent applied by all participating industries was sodium hypochlorite, though concentrations and application times differed among industries from 50 to 200 ppm for 30 to 110 s. Simulations using predictive models indicated that the reductions in Salmonella in RTE leafy vegetables would vary in the range of 1.70–2.95 log CFU/g during chlorine-washing depending on chlorine concentrations applied, washing times, and vegetable cutting size, which varied from 9 to 16 cm2 among industries. Moreover, Salmonella would be able to grow in RTE leafy vegetables during storage and distribution, achieving levels of up to 2 log CFU/g, considering the storage and transportation temperatures and times reported by the industries, which vary from 4 to 14 °C and from 18 to 30 h. These results could be used to prioritize risk-based sampling programs by Food Official Control or determine more adequate process parameters to mitigate Salmonella in RTE leafy vegetables. Additionally, the information gathered in this study is useful for microbiological risk assessments.

