Abstract
Posted in Bacillus, Bacillus cereus, Clostridium, Clostridium perfringens, Cronobacter sakazakii, cross contamination, D-Value, Decontamination Microbial, E.coli, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk
Clostridium perfringens bacteria are one of the most common causes of food poisoning. CDC estimates that the bacterium causes nearly 1 million foodborne illnesses in the United States every year.
C. perfringens makes spores, which are inactive forms of the bacterium that help it survive heat, dryness, and other environmental conditions. Under certain conditions, such as when food is kept at an unsafe temperature (between 40°F and 140°F), C. perfringens spores can transform into active bacteria, which multiply in the food. After someone eats food containing C. perfringens, it can produce a toxin (poison) that causes diarrhea.
Foods cooked in large batches and held at unsafe temperatures are typically involved in outbreaks of C. perfringens food poisoning. Specific foods commonly linked to C. perfringens food poisoning include
Outbreaks of C. perfringens food poisoning tend to happen in settings where large groups of people are served and keeping food at proper temperatures may be difficult—for example, hospitals, school cafeterias, prisons, nursing homes, and large events with catered food.
Most of these outbreaks happen in November and December. Many of them have been linked to popular holiday foods, such as turkey and roast beef.
Posted in Clostridium, Clostridium perfringens, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Uncategorized
It would be a crime for your whānau and friends to come down with foodborne illness this festive season – so New Zealand Food Safety and the Chicken Scene Investigators have got your back.
“Each year, over our summer, there is a rise in cases of foodborne illness and hospitalisations,” says New Zealand Food Safety deputy director-general Vincent Arbuckle.
“The most commonly reported illness is campylobacteriosis – caused by Campylobacter bacteria – with our youngest and oldest having the highest rates of infection.
“There were 5,729 confirmed cases of campylobacteriosis in 2021, with 846 people needing hospital treatment, up from 718 in 2020. And 2022 looks set to follow a similar trajectory, with more than 5,300 cases nationally so far.
“The most common source of Campylobacter from food is raw or undercooked chicken.
“So, one big thing you can do this festive season to keep your whānau and friends healthy is to make sure you handle raw chicken safely. Cook it properly and use separate utensils and chopping boards, and, as with all food, don’t leave it out in the heat of the day, both before cooking and after you’ve finished eating.”
To help you with this, New Zealand Food Safety today launches a new food safety campaign. In a series of videos, our 2 Chicken Scene Investigators invite you to join them to spot the chicken-handling crime.
“Campylobacteriosis symptoms are nasty. They include diarrhoea, fever, headache, muscle aches, abdominal pain, and vomiting. It may also develop into more severe illness such as Guillain-Barré Syndrome, a disorder in which the body’s immune system attacks its nerves, sometimes resulting in permanent paralysis,” says Mr Arbuckle.
If you have symptoms, you can call Healthline for free anytime on 0800 61 11 16, or contact your doctor or practice nurse for advice.
“So, wherever you’re gathering – from BBQs to work do, beach parties to kai at the marae, Christmas lunch or potluck dinner – make sure you don’t contaminate your plate this summer.”
Te Whatu Ora medical officer of health Jay Harrower adds: “Every year thousands of people are diagnosed as being infected with Campylobacter, and for some it can be very serious. Across New Zealand Campylobacter cases are spiking once again this summer, but there are simple steps everyone can take to reduce the risk to them and their whānau.”
Chicken Scene Investigator tips to keep your whānau and friends safe:
Campylobacter infection: symptoms and advice
Posted in Campylobacter, campylobacter coli, Campylobacter jejuni, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Safety, Food Safety Management, food safety training, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk
After an extensive outbreak investigation, cucumber from a Spanish supplier stands out as the likely source of infection in a salmonella outbreak that started in November. No new cases of illness have been reported in recent weeks, which may indicate that there are no longer any contaminated products on the market and that the outbreak is probably over.
There are now 72 people registered who have become ill from the gastrointestinal bacterium Salmonella Agona. The peak of infection in Norway was in mid-November, and the last reported case of the disease came on 2 December. Cases of the same outbreak strain have also been reported in Sweden and the Netherlands, in the same period.
– It is not always possible to find the source of infection in such outbreaks, but now some batches of cucumber from a Spanish supplier have been identified as the most likely, says Catherine Svindland, senior adviser at the Norwegian Food Safety Authority.
These batches of cucumber are no longer on the market. The Norwegian importers of cucumbers from the supplier have intensified the sampling of cucumbers as an additional safety measure. Salmonella was not found in these samples. The Norwegian Food Safety Authority has notified the Spanish authorities and other countries in the EU about the suspicion.
The contaminating cucumbers have probably not been on the market since November.
The outbreak investigation continues to, if possible, definitively establish that these cucumbers are the source of infection. This can be challenging, as the polluting products are likely to be out of the market and people’s fridges.
Posted in food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Salmonella
Nestlé has been given permission to partially reopen a plant in France where pizzas behind a serious E. coli outbreak were made.
French officials from the Nord area of the country in the Hauts-de-France region gave the green light this past week for operations to restart at the Buitoni factory in Caudry.
Approval only applies to production of pizzas with cooked dough. The line making pizzas with no re-baking of dough, such as the Fraîch’Up range, will not restart yet.
Fraîch’Up frozen pizzas were the source of the largest E. coli-HUS outbreak ever documented in France.
One element of the plan to restart has included the dismantling and cleaning of 19,000 parts on the production line.
Posted in Decontamination Microbial, E.coli, food bourne outbreak, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, foodborne outbreak, foodbourne outbreak, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak

The COVID-19 pandemic has impacted surveillance activities for multiple pathogens. Since March 2020, there was a decline in the number of reports of norovirus and Campylobacter recorded by England’s national laboratory surveillance system. The aim is to estimate and compare the impact of the COVID-19 pandemic on norovirus and Campylobacter surveillance data in England.
Posted in Campylobacter, campylobacter coli, Campylobacter jejuni, COVID-19, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Norovirus, Research, Retailer Campylobacter Survey
Between mid-August and December 2022, the Statens Serum Institut has registered 11 cases of Listeria monocytogenes . The Statens Serum Institut, the Danish Food Agency and the Danish Food Institute DTU have investigated the disease outbreak and identified fish cakes as the source.
Between mid-August and December 2022, the Statens Serum Institut registered 11 people who are infected with the same type of Listeria monocytogenes (figure 1). Among the sick are 4 men and 7 women. In relation to age, there is one child and 10 adults (median age is 77). The patients are infected throughout the country (table 1). Interviews with six patients showed that all had eaten fish cakes.
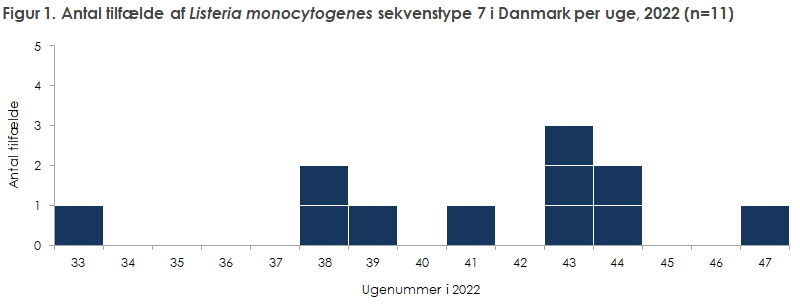
Table 1. Patients with the same type of Listeria monocytogenes in Denmark, August to December 2022, per region (n=11)
Region |
Number of patients |
| The capital | 4 |
| Central Jutland | 2 |
| Northern Jutland | 0 |
| Zealand | 2 |
| Southern Denmark | 3 |
| Total | 11 |
The outbreak is handled by the Central Outbreak Group, which consists of SSI, the Danish Veterinary and Food Administration and the DTU Food Institute. SSI stands for whole-genome sequencing of listeria isolates from the patients and interviews with patients or relatives with a view to identifying a possible source of infection. The outbreak investigation showed that fish meatballs were the cause of the disease outbreak. The fish meatballs were recalled from stores on November 8, 2022.
The bacteria is of the type Listeria monocytogenes . By whole-genome sequencing of the Listeria monocytogenes bacteria isolated from the patients, it can be seen that they are very closely related and belong to sequence type 7.
Posted in Decontamination Microbial, food bourne outbreak, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, foodborne outbreak, foodbourne outbreak, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak
December 17, 2022
There are a range of symptoms for listeriosis. Depending on the severity of the illness, symptoms may last from days to several weeks. Mild symptoms may include a fever, muscle aches, nausea, vomiting, and diarrhea. If the more severe form of listeriosis develops, symptoms may include headache, stiff neck, confusion, loss of balance, and convulsions. For the very young, the elderly, and the immune-compromised listeriosis can result in death.
People infected with L. monocytogenes may start to see symptoms in a few hours or as long as two to three days after eating contaminated food. More severe forms of listeriosis may take anywhere from three days to three months to develop.
Listeriosis can be particularly dangerous for pregnant women and their newborn babies, leading to serious complications with their pregnancy, including miscarriage and stillbirth. Babies born with a listeriosis infection may develop severe health complications that require immediate medical attention, lead to lifelong health problems, or result in death. Women who suspect they have symptoms of listeriosis (muscles aches, nausea, stiffness in neck, headaches, etc.) should seek medical care immediately and tell their health provider what they ate. Learn more about People at Risk of Foodborne Illness.
Due to the range in severity of illness, people should consult their health care provider if they suspect that they have developed symptoms that resemble a(n) L. monocytogenes infection.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Uncategorized
The Centers for Disease Control and Prevention (CDC), the U.S. Food and Drug Administration (FDA), the Texas Department of State Health Services, and other public health partners, are investigating a multistate outbreak of norovirus illnesses linked to raw oysters from Texas.
Illnesses: 211 illnesses* have been reported as of December 15, 2022.
States affected: Alabama (AL), Florida (FL), Georgia (GA), Louisiana (LA), Mississippi (MS) North Carolina (NC), Tennessee (TN), Texas (TX)
Recall: Yes DSHS Recalls Oysters Harvested in Area of Southeastern Galveston Bay | Texas DSHS
Investigation Status: Active
*This number is an estimate based on the information we have at this time. CDC is working with state and local partners and will update this number as more information is gathered.
If eaten raw, oysters and other filter-feeding shellfish can contain viruses and bacteria that can cause illness or death. Anyone who consumes raw shellfish is at risk of contracting norovirus. Children younger than five years old, the elderly, and those people with weakened immune systems are more likely to have severe infections. Food contaminated with norovirus may look, smell, or taste normal. To avoid food poisoning from oysters, cook them well to a temperature of at least 145 degrees F.
Do not serve or sell raw oysters harvested between 11/17/2022 and 12/7/2022 from harvest area TX 1, Galveston Bay, Texas:
Throw away any remaining oysters or return them to your distributor for destruction.
These oysters may be contaminated with norovirus. Follow these steps:
Do not eat any raw oysters from the areas listed above. If you have oysters at home from any of the areas listed above, throw them away. Clean any utensils or food preparation surfaces that may have touched the oysters.
If you think you might have gotten sick from eating possibly contaminated raw oysters, talk to your healthcare provider and report your illness to your local health department.
Posted in food bourne outbreak, food contamination, food handler, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Virus, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Norovirus, Norovirus Oysters, outbreak, Virus