CFS
Recently, the Centre for Food Safety (CFS) collected a soybean milk sample from a local food shop when following up on a food complaint. The sample was later found containing a bacterium known as Bacillus cereus (B. cereus) in an amount that exceeded the limit in the CFS’ Microbiological Guidelines for Food and was consided unsatisfactory. Soybean milk produced by local retail shops, such as soybean product shops and congee shops, usually has a short shelf life and requires stringent temperature control to maintain its safety. In this article, we will look into how the bacterium finds its way to survive in soybean milk production and how to prevent it.
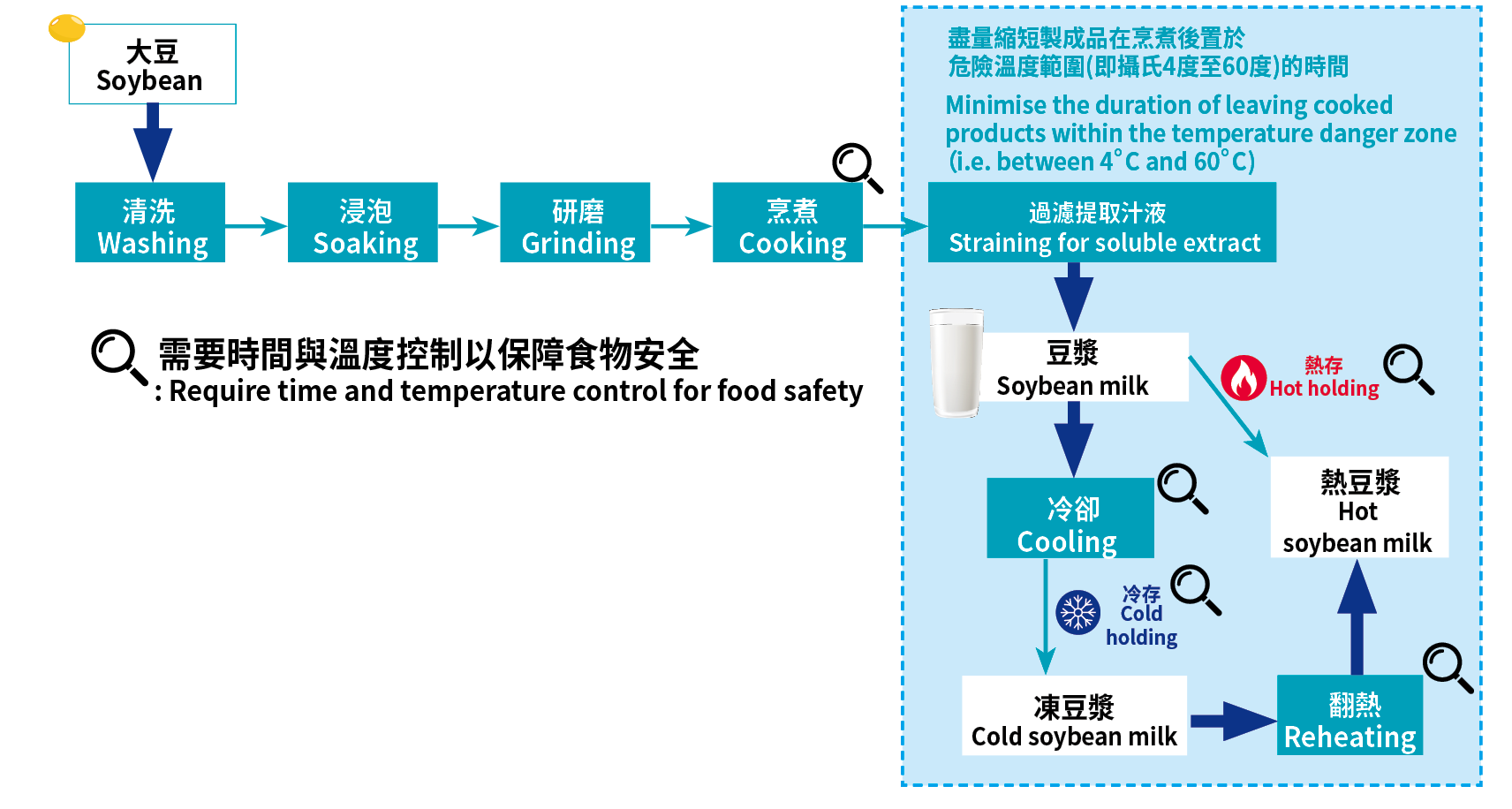
Figure 1: Highlights of processes requiring time and temperature control during production of soybean milk
Bacillus cereus Surviving Heat Treatment
B. cereus is a spore-forming bacterium and is ubiquitous in the environment. It is naturally present in soils, plants, agricultural products, etc. Hence, soybeans used in the production of soybean milk (see Figure 1) may contain B. cereus.
While cooking is effective to kill vegetative cells of B. cereus, its spores are heat-resistant and can only be eliminated by high temperature treatment, e.g. 121°C for 3 minutes. In this regard, the cooking temperature of soybean milk production at retail shops is not sufficient to kill the spores. Instead, the heat of cooking can not only induce the spores to germinate and become vegetative cells, but also create a favourable environment for the cells to grow by eliminating other microorganisms competing for growth. As a result, if the soybean milk is left under ambient condition for a prolonged period of time after cooking, vegetative cells can proliferate into a large number.
The vegetative cells can then produce a heat-resistant emetic (i.e. causes vomiting) toxin. Even if contaminated soybean milk is reheated subsequently, it can still cause food poisoning that is characterised by causing the victim to vomit shortly after consumption.
Prevention by Time and Temperature Control
Despite the tenacious nature of B. cereus, soybean milk can still be safely produced. To prevent the microbiological hazard, certain production processes require time and temperature control (see Figure 1). First, the soybean slurry from grinding process has to be cooked thoroughly to kill B. cereus vegetative cells and other bacteria. The heat treatment can also denature soybean enzymes that affect digestion of consumers.
After cooking, it is important to minimise the duration of leaving cooked products within the temperature danger zone, i.e. between 4°C and 60°C, in order to prevent the growth of vegetative cells of B. cereus formed from surviving spores. Cooked soybean slurry is strained through cheese cloth for soluble extract, i.e. soybean milk. After straining, freshly made soybean milk can be held at above 60°C for hot serving. As for cold soybean milk, it has to be cooled as quickly as possible, i.e. cooling to 20°C within two hours, and then to 4°C within the next four hours or less. Cooled soybean milk can then be stored at or below 4°C for cold serving. At certain food service businesses, soybean milk in cold holding may be reheated for serving. In that case, it has to be reheated with temperature reaching at least 75°C.
Last but not least, the production environment and equipment have to be kept hygienic to reduce microbiological contamination. In particular, the equipment used after cooking processes, such as cheese cloth, container and dispenser, has to be cleaned after each use to minimise the building up of B. cereus which may contaminate cooked soybean milk of the next batch.
Key Points to Note
- Soybeans can be naturally contaminated with B. cereus. Normal cooking can kill vegetative cells of B. cereus, but not the spores and toxin of it.
- If cooked soybean milk is left at ambient temperature for too long, vegetative cells of B. cereus formed from surviving spores can produce toxin.
- It is important to minimise the duration of leaving soybean milk at a temperature range between 4°C and 60°C after cooking which favours the growth of B. cereus vegetative cells and toxin production.
Advice to the Trade
- Avoid over-production as soybean milk has a short shelf life.
- Speed up the cooling process by, for example, dividing soybean milk into small portions or using water bath or ice bath to cool bottled soybean milk.
- Minimise the storage time of soybean milk, preferably clearing the stock within one day after production.
Advice to the Public
- Consume soybean milk produced at retail shops as soon as possible.
- Refrigerate the soybean milk at 4°C or below if it is not to be consumed immediately.



