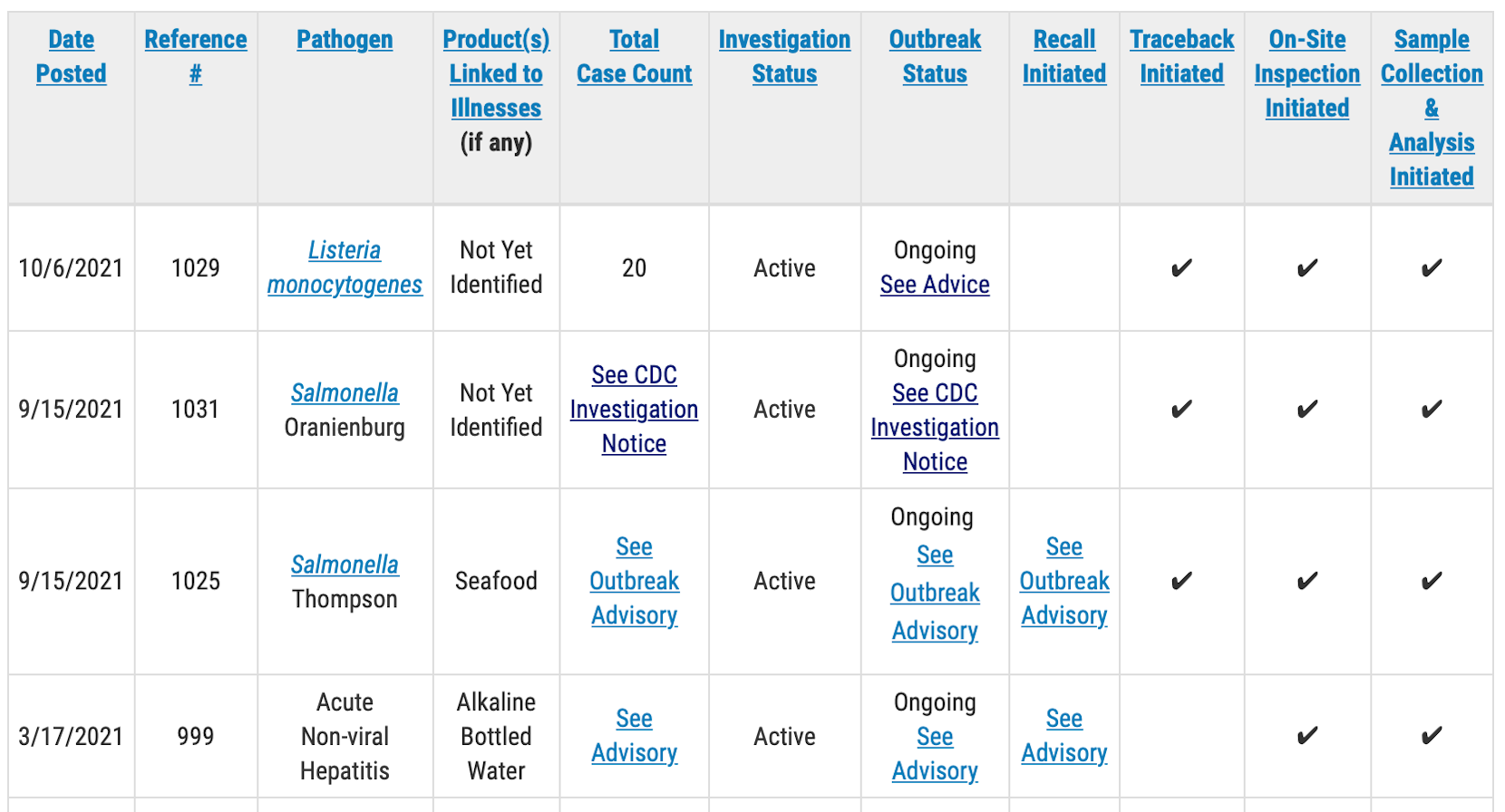
he U.S. Department of Agriculture’s Food Safety and Inspection Service (FSIS) today announced that it is mobilizing a stronger, and more comprehensive effort to reduce Salmonella illnesses associated with poultry products. The agency is initiating several key activities to gather the data and information necessary to support future action and move closer to the national target of a 25% reduction in Salmonella illnesses.
“Far too many consumers become ill every year from poultry contaminated by Salmonella,” said Agriculture Secretary Tom Vilsack. “We need to be constantly evolving in our efforts to prevent foodborne illness to stay one step ahead of the bad bugs. Today we’re taking action to help prevent Salmonella contamination throughout the poultry supply chain and production system to protect public health.”
Despite consistent reductions in the occurrence of Salmonella in poultry products, more than 1 million consumer illnesses due to Salmonella occur annually, and it is estimated (PDF, 1.4 MB) that over 23% of those illnesses are due to consumption of chicken and turkey.
“Reducing Salmonella infections attributable to poultry is one of the Department’s top priorities,” said USDA Deputy Under Secretary Sandra Eskin, who is leading the initiative. “Time has shown that our current policies are not moving us closer to our public health goal. It’s time to rethink our approach.”
USDA intends to seek stakeholder feedback on specific Salmonella control and measurement strategies, including pilot projects, in poultry slaughter and processing establishments. A key component of this approach is encouraging preharvest controls to reduce Salmonella contamination coming into the slaughterhouse. The data generated from these pilots will be used to determine if a different approach could result in a reduction of Salmonella illness in consumers.
The effort will leverage USDA’s strong research capabilities and strengthen FSIS’ partnership with the Research, Education and Economics (REE) mission area to address data gaps and develop new laboratory methods to guide future Salmonella policy. Meanwhile, the National Advisory Committee for Microbiological Criteria in Foods, an independent federal advisory committee, will be asked to advise on how FSIS can build on the latest science to improve its approach to Salmonella control. Since it is not just the presence or absence of Salmonella, but the quantity of bacteria that can impact the likelihood of illness, FSIS will examine how quantification can be incorporated into this approach. Moreover, with emerging science suggesting that not all Salmonella are equally likely to cause human illness, FSIS will focus on the Salmonella serotypes and the virulence factors that pose the greatest public health risk.
Moving forward, this initiative will require collaboration and ongoing dialogue with stakeholders — industry, consumer groups, and researchers alike. USDA looks forward to working closely with stakeholders on informing and implementing key activities of this framework in the very near future.
USDA touches the lives of all Americans each day in so many positive ways. In the Biden-Harris Administration, USDA is transforming America’s food system with a greater focus on more resilient local and regional food production, fairer markets for all producers, ensuring access to safe, healthy and nutritious food in all communities, building new markets and streams of income for farmers and producers using climate smart food and forestry practices, making historic investments in infrastructure and clean energy capabilities in rural America, and committing to equity across the Department by removing systemic barriers and building a workforce more representative of America. To learn more, visit www.usda.gov.