Brand : Pascoli Italiani
Denomination : Fontina DOP
Reason for reporting : Recall due to microbiological risk
Publication date : 18 October 2022

Brand : Pascoli Italiani
Denomination : Fontina DOP
Reason for reporting : Recall due to microbiological risk
Publication date : 18 October 2022

Posted in food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Toxin, STEC, STEC E.coli
WASHINGTON, October 13, 2022 – The U.S. Department of Agriculture’s Food Safety and Inspection Service (FSIS) is issuing a public health alert due to concerns that a specific ground beef product may be contaminated with E. coli O103. A recall was not requested because the products are no longer available for purchase.
The raw ground beef items were produced on October 4, 2022. The following product is subject to the public health alert view labels:
The establishment’s retail store location in Hudson, Wyoming sold the affected product directly to consumers. FBS Hudson is actively attempting to contact consumers who may have purchased 14 packages of ground beef product subject to the public health alert.
The problem was discovered when FBS Hudson alerted FSIS that its routine microbial testing results found Shiga toxin-producing E. coli (STEC) O103 in a sample of the ground beef. There have been no confirmed reports of illness due to consumption of these products.
Many clinical laboratories do not test for non-O157 STEC, such as O103 because it is harder to identify than STEC O157:H7. People can become ill from STECs 2-8 days (average of 3-4 days) after consuming the organism.
Most people infected with STEC O103 develop diarrhea (often bloody) and vomiting. Some illnesses last longer and can be more severe. Infection is usually diagnosed by testing of a stool sample. Vigorous rehydration and other supportive care is the usual treatment; antibiotic treatment is generally not recommended. Most people recover within a week, but, rarely, some develop a more severe infection. Hemolytic uremic syndrome (HUS), a type of kidney failure, is uncommon with STEC O103 infection. HUS can occur in people of any age but is most common in children under 5 years old, older adults and persons with weakened immune systems. It is marked by easy bruising, pallor and decreased urine output. Persons who experience these symptoms should seek emergency medical care immediately.
Posted in E.coli, E.coli O103, E.coli O157, E.coli O157:H7, food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Toxin, STEC, STEC E.coli

| GTIN | Batch | |
|---|---|---|
| 3246992137004 | 0015/041022 | |
Posted in food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Toxin, Salmonella, STEC, STEC E.coli
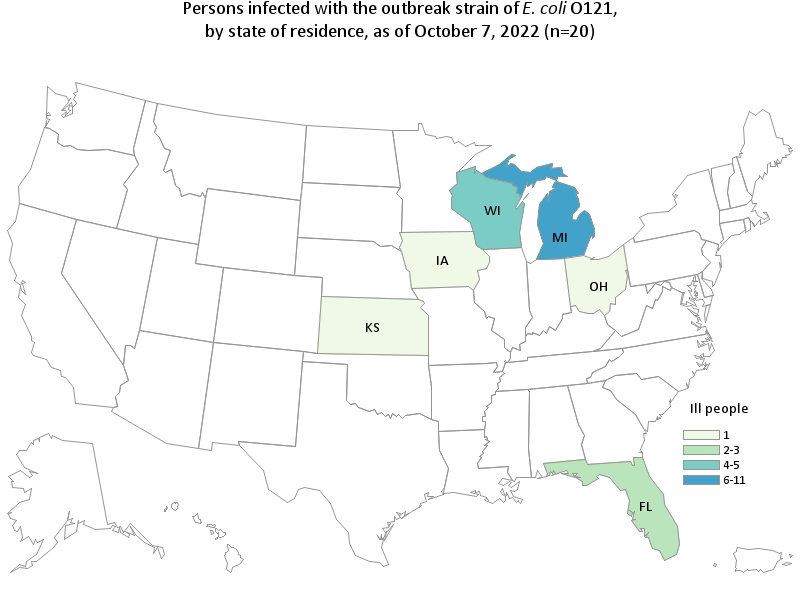
The FDA, along with CDC and state and local partners, are investigating a multistate outbreak of E. coli O121:H19 infections linked to Earth Grown frozen falafel.
Based on epidemiologic information provided by CDC and interviews conducted by state and local public health officials, of 18 people interviewed, 15 reported shopping at ALDI stores. Among these 15 people who reported shopping at ALDI stores, 6 reported eating Earth Grown brand frozen falafel purchased from ALDI in the week before getting sick.
On October 6, 2022, the manufacturer of Earth Grown frozen falafel, Cuisine Innovations, initiated a voluntary recall. Recalled products include Earth Grown vegan traditional falafel and garlic & herb falafel distributed and sold exclusively by ALDI. Additional information on recalled products is available in the firm’s recall notice.
On October 6, 2022, ALDI removed any remaining Earth Grown frozen falafel from stores.
FDA’s investigation is ongoing. Updates to this advisory will be provided as they become available.
Consumers, restaurants, and retailers should not eat, sell, or serve recalled Earth Grown Traditional Falafel or Garlic & Herb Falafel sold exclusively by ALDI after June 24, 2021.
These items are no longer available for sale but were sold frozen and have a long shelf-life of 18 months, so consumers should check their freezers for these products. If you have recalled frozen falafel in your freezer, do not eat or serve them.
Posted in E.coli, E.coli O121, food bourne outbreak, food contamination, food handler, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Toxin, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, outbreak, STEC, STEC E.coli


Cuisine Innovations Unlimited, LLC of 180 Lehigh Avenue, Lakewood, NJ, is voluntarily recalling its Earth Grown Vegan Traditional Falafel and Garlic & Herb Falafel Distributed & Sold Exclusively by Aldi, Batavia, IL due to the possible presence of Shiga toxin-producing E. coli.
Shiga-toxin-producing E. coli is an organism that can cause foodborne illness in a person who eats a food item contaminated with it. Symptoms of infection may include stomach cramps, diarrhea, and vomiting. The illness primarily impacts elderly individuals, children, and people with weakened immune systems. Most healthy adults and children rarely become seriously ill.
The voluntarily recalled Earth Grown Vegan Traditional Falafel And Garlic & Herb Falafel Distributed & Sold Exclusively by Aldi, Batavia, IL were distributed in ALDI retail stores in the following states: Alabama, Arizona, Arkansas, California, Connecticut, Delaware, District of Columbia, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nebraska, New Hampshire, New Jersey, New York, North Carolina, North Dakota, Ohio, Oklahoma, Pennsylvania, Rhode Island, South Carolina, South Dakota, Tennessee, Texas, Virginia, West Virginia, and Wisconsin.
The product comes in a bag in a box marked with any of the following Lot numbers: 1472, 1481, 1531, 1532, 1541, 1552, 1561, 1581, 1601, 1611, 1612, 1661, 1682, 1732, 1752, 1762, 1782, 1802, and 1812, and would have been shipped to stores after June 24, 2021. The lot number can be found in the “Best if used by” area on the outside flap of the box. There has been no further production of this product.
There have been 20 reported cases in six (6) states (FL, IA, KS, MI, OH and WI) with onset dates reported between July 24, 2022 and September 19, 2022 with 5 hospitalization and no deaths.
Consumers who have purchased Earth Grown Vegan Traditional Falafel and Garlic & Herb Falafel Distributed & Sold Exclusively by Aldi, Batavia, IL with any of the above lot numbers after June 24, 2021, are urged to return them to the place of purchase for a full refund. Consumers with questions may contact the company Monday through Friday, 8:00 a.m. to 4:00 p.m. Eastern Time at 1-201-439-1036, Ext. 26.
Posted in FDA, food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Safety Management, Food Testing, Food Toxin, STEC, STEC E.coli
Public Health is investigating an outbreak of Shiga toxin-producing E. coli (also known as STEC) associated with diarrhea and abdominal pain at Torero’s Mexican Restaurant in Renton.
The investigation is ongoing. At this time, we have not identified how STEC was spread within the restaurant. This is not uncommon for STEC outbreaks, because the bacteria can spread through contaminated food items, environmental surfaces, and from person to person.
Since September 5, 2022, 3 people from 3 separate meal parties reported becoming ill after eating food from Torero’s Mexican Restaurant in Renton on September 3, 2022 and September 7, 2022. All of the people developed one or more symptoms consistent with STEC, including diarrhea (often bloody), abdominal cramping, nausea, and vomiting. We have not identified any ill employees.
Posted in Decontamination Microbial, E.coli, food bourne outbreak, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, foodborne outbreak, foodbourne outbreak, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, STEC, STEC E.coli
Federal officials have declared that an outbreak of E. coli O157:H7 infections related to romaine lettuce on Wendy’s sandwiches has ended.
The Centers for Disease Control and Prevention is reporting that the total number of confirmed patients is 109, up from the 97 reported in its most recent update on Sept. 1. About half — 52 — of the patients have been so sick they had to be admitted to hospitals. Thirteen of the patients developed hemolytic uremic syndrome (HUS), a serious often life-threatening condition that can cause kidney failure. No one had died as of this evening.
As of the report tonight from the CDC the specific source of the E. coli could not be 100 percent confirmed. However, 83 percent of 82 patients for whom the information was available reported eating at Wendy’s before becoming ill.
“The true number of sick people in this outbreak is likely much higher than the number reported, and the outbreak may not have been limited to the states with known illnesses. This is because many people recover without medical care and are not tested for E. coli,” according to the CDC statement.
Posted in Decontamination Microbial, E.coli O157, E.coli O157:H7, food bourne outbreak, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Poisoning, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Poisoning, STEC, STEC E.coli
There was a big fall in the number of Shiga toxin-producing E. coli (STEC) infections in Europe in 2020, according to recently published data.
In 2020, 4,824 confirmed STEC infections were reported. This is down from 8,339 in 2019. STEC infection is mainly acquired through consumption of contaminated food or water and contact with animals or their feces.
Data on STEC infections were reported by 29 countries. Notification is voluntary in Belgium, France, Luxembourg, and Spain or based on another type of system in Italy.
Germany with 1,409 and Ireland with 734 had the most infections, accounting for 44 percent of all cases. The highest country-specific notification rates were in Ireland, Malta, Denmark, and Norway.
Posted in Decontamination Microbial, E.coli, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, HUS, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research, Shigatoxin, STEC, STEC E.coli

Posted in bacterial contamination, Contaminated water, cross contamination, Decontamination Microbial, E.coli, food contamination, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research, Salmonella, STEC, STEC E.coli, Water, water microbiology, Water Safety