Tribune 242
THERE have been four confirmed cases of conch poisoning and as many as six unconfirmed cases, Health Minister Duane Sands announced yesterday.
According to Dr Sands, the exposure took place in the previous 72 to 96 hours with a number of the patients affected having eaten at Potter’s Cay.
Noting that an outbreak of conch poisoning is something the country can “ill afford” right now, Dr Sands was adamant the issue can be easily mitigated if proper hygiene is maintained.
Four cases have been confirmed via laboratory testing but Dr Sands said there are a number of unconfirmed cases – “possibly as many as six” awaiting laboratory results. He added the affected people are being treated at both Doctors Hospital and Princess Margaret Hospital, and so far, all the self-identified patients are Bahamian.
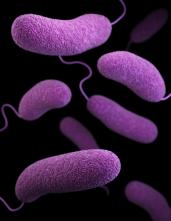
Conch poisoning is caused by vibrio parahaemolyticus, a bacteria which requires salt water to live. According to Dr Sands, when ingested, vibrio bacteria can cause watery diarrhoea, which is usually accompanied by abdominal cramping, vomiting, fever, nausea, and chills.
These symptoms often occur within 24 hours of ingestion and last about three days. He added that severe illness is “rare” and typically occurs in people with a “weakened” immune system.
The last major outbreak of conch poisoning occurred in the 1990s, around 1991 and 1999, Dr Sands said. He added that there were more than 1,100 cases of vibrio parahaemolyticus poisoning during that era.
The health minister was also adamant the issue is not with the conch meat itself.
“Vibrio is not an issue of the meat itself. Vibrio is a bacteria that ordinarily lives in seawater and is a part of the surface of the conch. The conch meat itself is not infected with vibrio parahaemolyticus. So you can wash it off. So, testing the conch meat itself is not the issue.