|
Key Take-Aways • Project focuses on period during romaine lettuce post-harvest cooling and refrigerated transport.
• Researchers will gauge pathogen physiological changes on inoculated romaine lettuce under lab-simulated post-harvest cooling.
• Researchers also will examine cooling’s impacts on E. coli O157:H7 persister cells — a form of dormancy.
• Goal is to develop an online tool to help the industry identify practices that reduce risk of E. coli O157:H7.
|
Category Archives: Research
Research – Project looks at E. coli risk during romaine post-harvest cooling
Posted in Decontamination Microbial, E.coli O157, E.coli O157:H7, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research, STEC, STEC E.coli
Research – Mycotoxins and Essential Oils—From a Meat Industry Hazard to a Possible Solution: A Brief Review
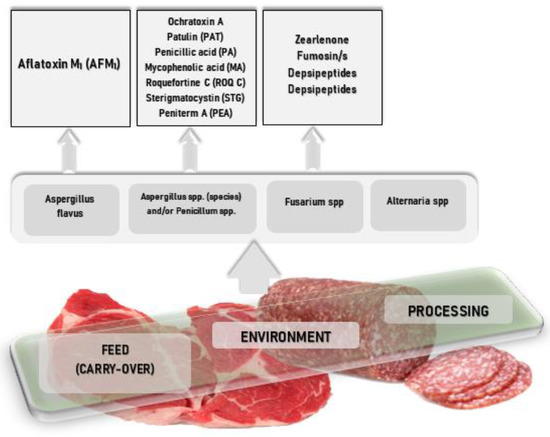
Abstract
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Technology, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Mould Toxin, Mould/Mold, Mycotoxin, Research, Technology
Research – Molecular Epidemiological Evidence Implicates Cattle as a Primary Reservoir of Campylobacter jejuni Infecting People via Contaminated Chickens

Abstract
Posted in Campylobacter, campylobacter coli, Campylobacter jejuni, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research
Research – Guidance for Controlling Listeria monocytogenes (Lm) in Retail Delicatessens – Best Practice Tips for Deli Operators
This guidance document provides specific recommendations for actions that retailers can take in the delicatessen (deli) area to control Listeria monocytogenes (Lm) contamination of ready-to-eat (RTE) meat and poultry products. This document is also available in PDF format. These materials highlight recommendations that are based on an evaluation of retail conditions and practices in the Interagency Risk Assessment–Listeria monocytogenes in Retail Delicatessens (Interagency Retail Lm Risk Assessment). In addition, FSIS has included information from the Food and Drug Administration (FDA) Food Code, scientific literature, other guidance documents, and lessons learned from Food Safety and Inspection Service (FSIS) verification sampling and review of sanitation programs for Lm in meat and poultry processing establishments.
This version of the guidance document replaces the previous version of the document which was issued and announced in the Federal Register (79 FR 22082; April 21, 2014). FSIS updated this guidance based on comments received during the public comment period, which closed on June 20, 2014. FSIS made the following changes in response to comments:
- Clarified that food processing equipment should be disassembled during cleaning and sanitizing.
- Added a recommendation that retailers scrub surfaces during cleaning to prevent biofilm formation.
- Clarified that retailers should rotate (change) sanitizers to help prevent Lm from establishing niches in the environment and forming biofilms.
Posted in food contamination, food handler, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Safety, Food Safety Management, food safety training, Listeria, Listeria monocytogenes, Research
Do You Know How to Use a Food Thermometer?
With the holidays approaching, it’s important to keep food safety in mind. One of the best ways to ensure that the food you make and serve is safe to eat it to use a food thermometer. But do you know how to use a food thermometer correctly?
First, you should know that there are several types of food thermometers. The most inexpensive and common is a dial thermometer. This has a dial on a stem that is attached to a probe. You can find these thermometers are most grocery stores. This thermometer is not always the most accurate, but it will give you a general reading.
The second type is an oven-proof thermometer that you use while the food is cooking. A probe goes into the meat roast or whole chicken or turkey, then a cord extends outside the oven to the dial that shows the reading. These can be digital or dial thermometers. You remove the food from the oven when it reaches the safe final internal temperature (or 5°F below that temperature with a 5-minute covered stand time).
Candy thermometers have larger temperature ranges, since the sugar solutions are often cooked to 300°F. These utensils look like a ruler, with a bulb at the bottom. They clip onto the side of a saucepan. To use when making candy or syrups, make sure that the bulb is in the sugar syrup but not touching the bottom of the saucepan.
Finally, instant-read digital thermometers consist of a probe that is attached to a plastic body and folds out. The digital reading is the most accurate, but these utensils can be expensive. You should know that the thermometer will usually time out after a few minutes. To restart it, just clip the probe back into the body and open it up again.
Read more at the link above.
Research – Attribution Analysis of Foodborne Disease Outbreaks Related to Meat and Meat Products in China, 2002–2017
Abstract

This study aimed to understand the epidemiological characteristics of foodborne disease outbreaks related to meat and meat products in China from 2002 to 2017. Data collected from the National Foodborne Diseases Surveillance System and searched databases were analyzed. From 2002 to 2017, China reported 2815 outbreaks caused by foodborne diseases related to meat and meat products, resulting in 52,122 illnesses and 25,361 hospitalizations, and 96 deaths. Outbreaks were markedly seasonal and concentrated from May to September, accounting for 66.93%. Outbreaks were concentrated mainly in China’s eastern coastal and southern regions. Unidimensional attribution analysis revealed that livestock meat was the most commonly implicated food category causing the outbreaks, accounting for 28.67%. Bacteria were the most common pathogenic cause of outbreaks, accounting for 51.94%. Clostridium botulinum was the most common pathogenic cause of death, accounting for 34.38%. Improper processing was the most common contributing factor, accounting for 27.89%. Households were the most common food preparation location causing the outbreak, accounting for 34.39%. Two-dimensional and multidimensional attribution analysis found that Salmonella contamination occurred in different locations and regions, mainly caused by various contributing factors and improper processing. Nitrite poisoning is caused by improper processing in households in East China. Bacterial causes were the commonest agents associated with foodborne diseases related to meat and meat products, and improving the safety and quality of meat and meat product should be a priority.
Posted in Clostridium, Clostridium botulinum, Decontamination Microbial, food bourne outbreak, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, foodborne outbreak, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Research, Salmonella
Research – UK food microbiology lab notes less contact with the EU
The United Kingdom leaving the European Union has resulted in reduced communication between UK and EU food networks, according to a new report.
The annual report covers work of the UK’s national reference laboratory (NRL) for food microbiology between April 2021 and March 2022.
The UK Health Security Agency (UKHSA) provides this service for the Food Standards Agency (FSA) for Listeria monocytogenes, coagulase-positive staphylococci, E. coli, Campylobacter, Salmonella and antimicrobial resistance.
USA – Stay Food Safe this Thanksgiving Holiday
Keep your stomach full of turkey and free from foodborne illness this Thanksgiving holiday. The U.S. Department of Agriculture (USDA) reminds us all that it’s important to remember the steps to food safety during America’s biggest meal.
“While the four steps to food safety — clean, separate, cook and chill — are important every day and at every meal, they are particularly significant on Thanksgiving,” said USDA Deputy Under Secretary Sandra Eskin. “There will likely be many guests and many delicious dishes at your holiday table, but you don’t want to invite any foodborne pathogens. Follow those four steps — in particular remember to use a food thermometer — and your Thanksgiving dinner will be a safe one.”
Keep your Thanksgiving celebration food safe by following the tips below.
Clean and Sanitize
Handwashing is the first step to avoiding foodborne illness. Wash your hands for at least 20 seconds with soap and water before, during, and after handling food. In a recent study, 97 percent of participants in a USDA test kitchen failed to wash their hands properly. Make sure to follow these handwashing steps:
- Wet your hands with clean, running water.
- Lather your fingers with soap.
- Scrub soapy hands and fingers thoroughly for at least 20 seconds. Rinse your hands under clean, running water.
- Dry hands off with a clean towel or air dry them.
Clean and sanitize any surfaces that have touched raw turkey and its juices and will later touch food such as kitchen counters, sinks, stoves, tabletops, etc.
Avoid Cross-Contamination
Cross-contamination is the spread of bacteria from raw meat and poultry onto ready-to-eat food, surfaces, and utensils. One way to avoid this is by using separate cutting boards — one for raw meat and poultry, and another for fruits and vegetables. Our recent study found that sinks are the most contaminated areas of the kitchen. USDA recommends against washing your raw poultry due to the risk of splashing bacteria throughout your kitchen. Clean and sanitize any areas that will come into contact with the turkey before and after cooking.
Thaw the Turkey Safely
Never thaw your turkey in hot water or leave it on a countertop. There are three ways to safely thaw a turkey: in the refrigerator, in cold water and in the microwave.
- Refrigerator thawing: Turkey can be safely thawed in a refrigerator to allow for slow and safe thawing. When thawing in a refrigerator, allow roughly 24 hours for every four to five pounds of turkey. After thawing, a turkey is safe in a refrigerator for one to two days.
- Cold water thawing: The cold water thawing method will thaw your turkey faster but will require more attention. When thawing in a cold-water bath, allow 30 minutes per pound and submerge the turkey in its original wrapping to avoid cross-contamination. Change the water every 30 minutes until the turkey is thawed. The turkey must be cooked immediately after thawing.
- Microwave thawing: To thaw a turkey that fits in the microwave, follow manufacturer’s recommendations. Cook it immediately after thawing because some areas of the food may become warm and begin to cook during the thawing process, bringing the food to the “Danger Zone.”
It’s safe to cook a completely frozen turkey; however, it will take at least 50 percent longer to fully cook.
Cook Thoroughly
Your turkey is safe to eat once it reaches an internal temperature of 165 F. Insert a food thermometer into the thickest part of the breast, the innermost part of the wing and the innermost part of the thigh to check its internal temperature. USDA recommends using a food thermometer even if the turkey has a pop-up temperature indicator to ensure it has reached 165 F in the three previously stated places.
Stuffing your Turkey
USDA recommends against stuffing your turkey since this often leads to bacteria growth. However, if you plan to stuff your turkey, follow these steps:
- Prepare the wet and dry ingredients for the stuffing separately from each other and refrigerate until ready to use. Mix wet and dry ingredients just before filling the bird’s cavity.
- Do not stuff whole poultry and leave in the refrigerator before cooking.
- Stuff the turkey loosely — about 3/4 cup of stuffing per pound.
- Immediately place the stuffed, raw turkey in an oven set no lower than 325 F.
- A stuffed turkey will take longer to cook. Once it has finished cooking, place a food thermometer in the center of the stuffing to ensure it has reached a safe internal temperature of 165 F.
- Let the cooked turkey stand 20 minutes before removing the stuffing.
For more information on turkey stuffing, visit Turkey Basics: Stuffing.
The Two-Hour Rule
Don’t leave your food sitting out too long! Refrigerate all perishable foods sitting out at room temperature within two hours of being cooked, or one hour if the temperature is 90 F or above. After two hours, perishable food will enter the “Danger Zone” (between 40 F and 140 F), which is where bacteria can multiply quickly and cause the food to become unsafe. Discard all foods that have been left out for more than two hours. Remember the rule — keep hot foods hot and cold foods cold.
- Transporting hot foods — Wrap dishes in insulated containers to keep their temperature above 140 F.
- Transporting cold foods — Place items in a cooler with ice or gel packs to keep them at or below 40 F.
When serving food to groups, keep hot food hot and keep cold food cold by using chafing dishes or crock pots and ice trays. Hot items should remain above 140 F and cold items should remain below 40 F.
Leftovers
Store leftovers in small shallow containers and put them in the refrigerator. Thanksgiving leftovers are safe to eat up to four days in the refrigerator. In the freezer, leftovers are safely frozen indefinitely but will keep best quality from two to six months.
Resources
For Thanksgiving food safety questions, call the USDA Meat and Poultry Hotline at 1-888-MPHotline (1-888-674-6854), email MPHotline@usda.gov or chat live at ask.usda.gov from 10 a.m. to 6 p.m. Eastern Time, Monday through Friday.
Do you have any last-minute turkey day questions? The Meat and Poultry Hotline will be open on Thanksgiving Day from 8 a.m. to 2 p.m. EST.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Safety, Food Safety Alert, Food Safety Management, food safety training, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research
Food Safety Aspects of Edible Insects
A recent review of available scientific literature suggests that, when cooked or processed in certain ways, edible insects can be a safe food product. Food safety considerations for the commodity were explored in the review, including microbiological contaminants, anti-nutritive factors, pesticide residues, toxic heavy metals, mycotoxins, and allergens.
The article outlined various food safety aspects of edible insects, stating that the commodity’s microbiological and anti-nutritive characteristics are of greatest concern. In general, research has demonstrated high counts of microorganisms to be present in fresh insects; however, with the appropriate thermal treatment, microbial loads can be eliminated. As with other foods, the efficacy of heat treatment on edible insects depends on factors such as the type, intensity, and duration of treatment, as well as the treated food composition. Solar and oven drying were underlined by the review as potential heat treatment methods.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research, Uncategorized
Research – Propionate and Butyrate Inhibit Biofilm Formation of Salmonella Typhimurium Grown in Laboratory Media and Food Models
Abstract
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Research, Salmonella


