Archives
-
Join 346 other subscribers
KSWFoodWorld
Blog Stats
- 450,653 Views
Category Archives: foodbourne outbreak
India – Evolution of Organic Food Safety Standards in India
Food safety is the key to achieve better public health. The high incidence of foodborne illness is a burden on public health and contributes significantly to the cost of health care. Though most of the foodborne illnesses are rare and often not reported in India, however, a nationwide study reported an alarming 13.2 per cent prevalence at the household level. Therefore there is a need for a comprehensive approach for safer and nutritious food for Indian citizens. Safer food promises a healthier lifestyle, longer lives, less costly healthcare and more resilient food industry.
The Indian food industry is regulated by the number of legislations covering licensing, sanitation, and permits. Food Safety and Standards Act 2006, established by the Government of India, was a vital step in the direction of developing the standards for food and regulating and monitoring the manufacture, processing, storage, distribution, sale, and import of food to ensure the availability of safe and nutritious food for human consumption.
Posted in food contamination, food death, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, Food Poisoning, Food Poisoning Death, Food Safety, Food Safety Alert, foodborne disease, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Research
USA – Outbreak Investigation of Listeria monocytogenes – Hispanic-style Fresh and Soft Cheeses (February 2021) – Update
The FDA, along with CDC and state and local partners, are investigating a multistate outbreak of Listeria monocytogenes infections linked to queso fresco cheeses made by El Abuelito Cheese, Inc.
On 2/19/2021, El Abuelito Cheese, Inc. announced their initial recall of products, and on 2/27/2021, they announced the expansion of their recall to cover additional products that are manufactured or handled in the same facility as the Queso Fresco products linked to this outbreak.
On 3/9/2021, the FDA received confirmation that recalled cheeses were also distributed to Rhode Island. States with confirmed distribution now include: AL, CT, FL, GA, IA, IL, IN, KS, KY, MA, MD, MI, MN, MO, MS, NC, NJ, NY, NE, OH, PA, RI, SC, TN, VA, and WI. View additional recall information.
Recommendation
Consumers, restaurants, and retailers should not eat, sell, or serve any recalled Queso Fresco, Quesillo (Oaxaca, string cheese), or Requeson (ricotta) cheeses.
Recalled brands by cheese type include:
- Queso Fresco: El Abuelito, Rio Grande, Rio Lindo
- Quesillo: El Abuelito, El Viejito, El Paisano, El Sabrosito, La Cima, Quesos Finos, San Carlos, Ideal Brands
- Requeson: El Abuelito, El Viejito
FDA recommends that anyone who purchased or received any recalled Queso Fresco, Quesillo, or Requeson cheeses use extra vigilance in cleaning and sanitizing any surfaces and containers that may have come in contact with these products to reduce the risk of cross-contamination. Listeria can survive in refrigerated temperatures and can easily spread to other foods and surfaces.
Some of the recalled cheeses were sold in bulk quantities and could have been repackaged by retailers. Ask your retailer if any Queso Fresco or Quesillo cheese you buy was repackaged from the cheeses recalled by El Abuelito. If you are unable to obtain an answer, do not buy it and throw away the potentially recalled cheese you have at home.
If you are at higher risk for severe Listeria infection (if you are pregnant, aged 65 or older, or have a weakened immune system due to certain medical conditions or treatments), call your healthcare provider right away if you have these symptoms after eating any Queso Fresco, Quesillo, or Requeson cheeses produced by El Abuelito:
- Pregnant people typically experience only fever, fatigue, and muscle aches. However, Listeria infection during pregnancy can lead to miscarriage, stillbirth, premature delivery, or life-threatening infection of the newborn.
- People who are not pregnant may experience headache, stiff neck, confusion, loss of balance, and convulsions, in addition to fever and muscle aches.
Follow these five steps to clean your refrigerator, containers, and surfaces that may have touched the cheeses. Listeria can survive in the refrigerator and can easily spread to other foods and surfaces.
Product Images
Recall Information
On 2/19/2021, El Abuelito Cheese, Inc. announced their initial recall of products, and on 2/27/2021, they announced the expansion of their recall to cover additional products. The recall announcements include the full product list and descriptions.
Consumers, restaurants, and retailers should not eat, sell, or serve any recalled Queso Fresco, Quesillo (Oaxaca, string cheese), or Requeson (ricotta) cheeses.
The firm’s recall does not include any additional products with the El Abuelito Cheese, Inc. label because they are not manufactured or handled in the same facility; this includes El Abuelito Meat, Inc., panela cheese, cotija cheese, mole, crema centroamericana, and crema mexicana. Updates will be provided as they become available.
FDA has posted lists of retailers that may have received Hispanic-styles cheeses from the El Abuelito Cheese, Inc. facility in Paterson N.J. It is possible that these lists may not include all retailers who have received these cheeses; however, these lists represents the best information currently available to the FDA.
- Retail Establishments that Received El Abuelito Brand Queso Fresco, Quesillo, and Requeson Products
- Retail Establishments that Received Private Label Brand Queso Fresco (Rio Grande, Rio Lindo), Quesillo (El Viejito, El Paisano, El Sabrosito, La Cima, Quesos Finos, San Carlos, Ideal Brands), and Requeson Products (El Viejito)
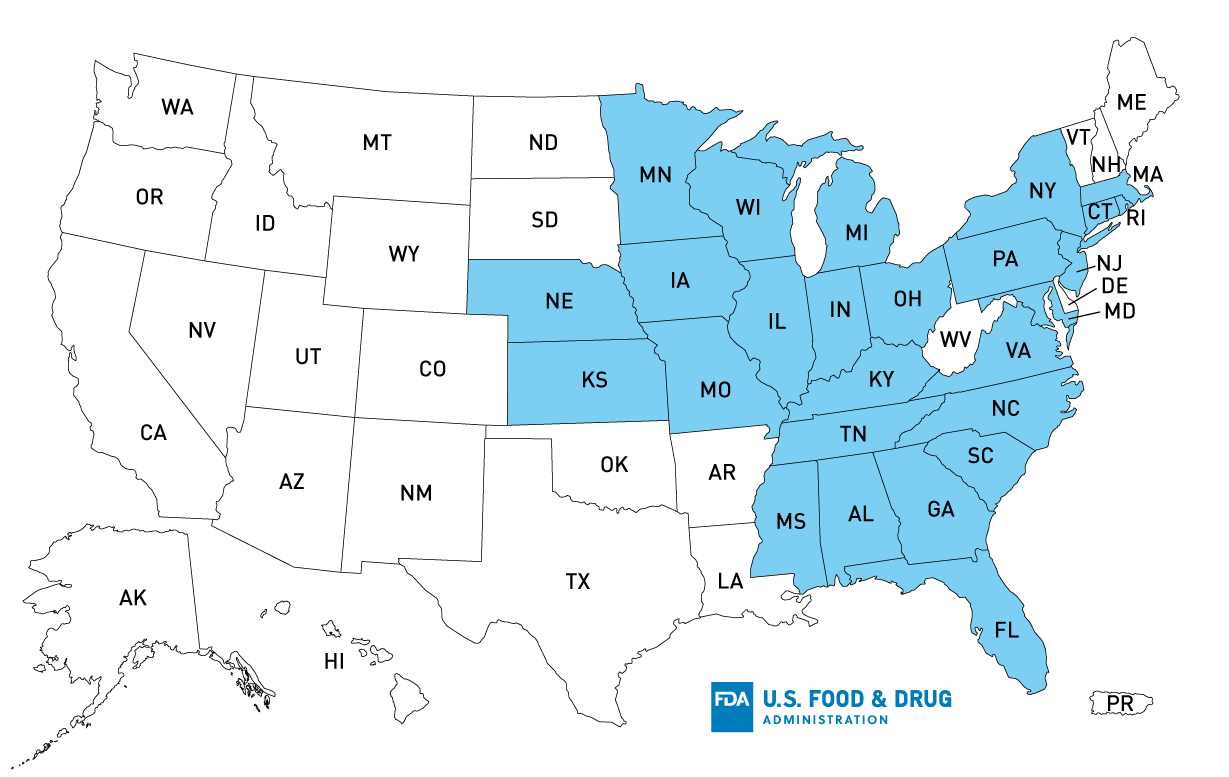
Map of U.S. Distribution of Recalled Queso Fresco, Quesillo, and Requeson Cheeseso
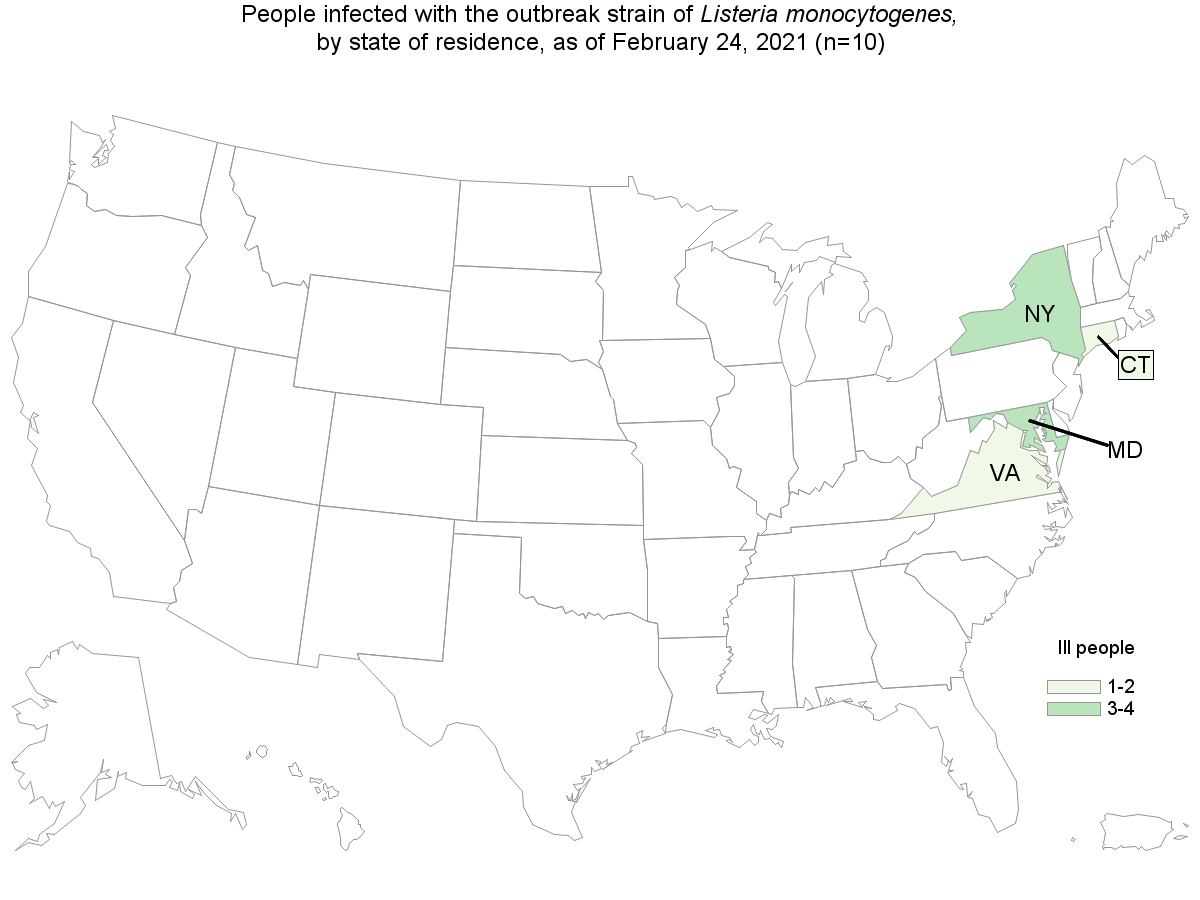
Case Count Map Provided by CDC
Case Counts
Total Illnesses: 11
Hospitalizations: 10
Deaths: 1
Last Illness Date: 2/14/2021
States with Cases: CT (1), MD (4), NY (4), and VA (2)
Product Distribution*: AL, CT, FL, GA, IA, IL, IN, KS, KY, MA, MD, MI, MN, MO, MS, NC, NJ, NY, NE, OH, PA, RI, SC, TN, VA, WI
*States with confirmed distribution; product could have been distributed further
Useful Links
- Food Safety Tips for Retailers and Consumers During an Outbreak
- Food Safety Resources for Produce Shippers and Carriers During a Foodborne Illness Outbreak
- Who to Contact
- What is Listeria?
- CDC’s Outbreak Page
- El Abuelito Recalls Queso Fresco Products Because of Possible Health Risk (Spanish)
- El Abuelito Expands Recall to Include Queso Fresco, Quesillo, and Requeson Products Because of Possible Health Risk
Posted in FDA, food bourne outbreak, food contamination, food death, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Alert, Food Testing, foodborne disease, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Listeria, Listeria monocytogenes, outbreak
Norway – Norway reports Salmonella outbreak, 10 people hospitalised
The Norwegian Institute of Public Health (NIPH) is reporting a Salmonella outbreak which is geographically spread over large parts of country.
Twenty cases have been reported–12 confirmed and 8 suspected cases. The same genetic profile have been detected in all 12 confirmed cases. Preliminary analyzes of samples from the 8 suspected cases indicate that these also carry the outbreak strain.
Those affected are aged from 11 to 91 years, median age is 59 years. 60% are women. The infected live in Viken (9), Oslo (3), Innlandet (2), Vestfold and Telemark (1), Agder (1), Rogaland (1), Vestland (1), Møre og Romsdal (1) and Nordland (1). 10 of the cases have been hospitalized.
“The infected live in many different counties. Therefore, we believe that they are infected through a food that is widely distributed”, says doctor Hilde Marie Lund at the department of infection control and emergency preparedness.
Posted in food bourne outbreak, food contamination, Food Hazard, Food Hygiene, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Poisoning, food recall, Food Safety, Food Safety Alert, Food Testing, foodborne disease, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Poisoning
France – Collective food poisoning suspected to be linked to the consumption of oysters contaminated by Norovirus
Several collective food poisoning infections possibly linked to the consumption of contaminated oysters have been reported since mid-February 2021 in several regions of France.
Since mid-February 2021, 46 mandatory declarations (DO) of collective food poisoning (TIAC) suspected of being linked to the consumption of oysters have been sent to Public Health France and / or to the General Directorate of food .
The meal dates at the origin of these toxi-infections are between 02/11/2021 and 02/25/2021 with a majority of meals reported on 02/14 (21 TIAC, 46%). All these TIACs took place in the context of a family meal with between 2 and 8 patients. A total of 164 patients were recorded and two people were hospitalized.
Several departments affected, in particular the West region
These TIACs mainly took place in New Aquitaine (23 in the department 33, 7 in the 17, 4 in the 40 and 2 in the 64), 5 in Pays de la Loire, 3 in Occitanie, 1 in Brittany and 1 in Bourgogne-Franche-Comté. For 36 of these TIACs, the origin of the oysters is known: Arcachon basin for 24 TIAC, Hossegor lake for 5, Marennes d’Oléron for 6 and Baie de Plouharnel for 1.
The investigations carried out
Stool analyzes carried out by the National Reference Center for Gastroenteritis Viruses in patients following 2 TIACs confirmed the presence of norovirus.
Shellfish collected from individuals who were sick after consuming oysters as well as from suppliers were analyzed by reference laboratories and laboratories approved by the Ministry of Agriculture and Food: noroviruses were identified . Noroviruses have also been detected in several production areas of consumed oysters.
The contamination of shellfish by norovirus for other TIACs is also suspected in view of the symptoms of sick people, mainly diarrhea and vomiting, and the incubation times between the consumption of shellfish and the onset of symptoms found during investigations of patients. TIAC. The torrential rains observed at the beginning of February may have favored the contamination of the environment / production areas and therefore of shellfish.
Actions taken since case detection
Four areas are currently closed by prefectural decrees temporarily prohibiting fishing, collection, transport, purification, shipping, storage, distribution, marketing and release for human consumption. shellfish following the discovery of the contamination of shellfish by noroviruses: the Arcachon basin (Gironde) since 02/18/2021, Hossegor lake (Landes) since 03/02/2021, the Chenaux du Payré (Vendée) since 25/02 and the bay of Plouharnel (Morbihan) since 03/03/2021.
- Find out more: http://www.atlas-sanitaire-coquillages.fr/ (“Statutes” section)
Posted in food bourne outbreak, food contamination, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Alert, Food Testing, Food Virus, foodborne outbreak, foodbourne outbreak, Norovirus, outbreak, Virus
Research – Prevalence of Listeria species on food contact surfaces in Washington State apple packinghouses
The 2014 caramel apple listeriosis outbreak was traced back to cross-contamination between food contact surfaces (FCS) of equipment used for packing and fresh apples. For Washington State, the leading apple producer in the U.S with 79% of its total production directed to the fresh market, managing the risk of apple contamination with Listeria monocytogenes within the packing environment is crucial. The objectives of this study were to determine the prevalence of Listeria spp. on FCS in Washington State apple packinghouses over two packing seasons, and to identify those FCS types with the greatest likelihood to harbor Listeria spp. Five commercial apple packinghouses were visited quarterly over two consecutive year-long packing seasons. A range of 27 to 50 FCS were swabbed at each facility to detect Listeria spp. at two timings of sampling, (i) post-sanitation and (ii) in-process (three hours of packinghouse operation), following a modified protocol of the FDA’s Bacteriological Analytical Manual method. Among 2,988 samples tested, 4.6% (n=136) were positive for Listeria spp. Wax coating was the unit operation from which Listeria spp. were most frequently isolated. The FCS that showed the greatest prevalence of Listeria spp. were polishing brushes, stainless steel dividers and brushes under fans/blowers, and dryer rollers. The prevalence of Listeria spp. on FCS increased throughout apple storage time. The results of this study will aid apple packers in controlling for contamination and harborage of L. monocytogenes and improving cleaning and sanitation practices of the most Listeria-prevalent FCS.IMPORTANCE Since 2014, fresh apples have been linked to outbreaks and recalls associated with post-harvest cross-contamination with the foodborne pathogen L. monocytogenes These situations drive both public health burden and economic loss and underscore the need for continued scrutiny of packinghouse management to eliminate potential Listeria spp. niches. This research assesses the prevalence of Listeria spp. on FCS in apple packinghouses and identifies those FCS most likely to harbor Listeria spp. Such findings are essential for the apple packing industry striving to further understand and exhaustively mitigate the risk of contamination with L. monocytogenes to prevent future listeriosis outbreaks and recalls.
Posted in food contamination, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, Food Safety, Food Testing, foodborne disease, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Listeria, Listeria monocytogenes, listeriosis, Research
Germany – Safe Food: Protecting against foodborne infections in communal facilities
In its updated leaflet, the German Federal Institute for Risk Assessment (BfR) provides recommendations for the preparation of meals in communal facilities that regularly cater for particularly vulnerable groups of people.
Foodborne infections particularly endanger young children, pregnant women and very old or sick people. “Errors in the selection and preparation of food can have serious consequences for particularly vulnerable people and even lead to death,” says Professor Dr. Dr. Andreas Hensel, President of the German Federal Institute for Risk Assessment (BfR). “With the BfR leaflet “Safe Food”, we would like to support community facilities in serving safe food to these particularly sensitive groups of people as well.”
Link to the leaflet:
- https://www.bfr.bund.de/cm/350/sicher-verpflegt-besonders-empfindliche-personengruppen-in-gemeinschaftseinrichtungen.pdf
 (2.7 MB)
(2.7 MB)
(The english version will be updated soon)
Foodborne illness can occur when pathogens enter commercial kitchens via raw ingredients or infected staff, are spread by hygiene failures in kitchens, and enter prepared foods. Temperature errors contribute to the survival and multiplication of pathogens in food.
Avoiding pathogens such as salmonella or listeria is particularly important when catering for sensitive individuals. Good hygiene and the right choice of ingredients and recipes reduce foodborne infections. Adequate food quality, proper storage and preparation of food, and staff training are also essential.
Fruit and vegetables should be washed thoroughly and peeled if possible. Low-acid fruit, vegetables and leafy salads must be eaten immediately after cutting or should be kept in the refrigerator until consumption. To protect against listeriosis, it may be advisable to reheat raw, but also already heated, ready-to-eat food before serving.
Most pathogens are killed when the food is heated to 72 degrees for at least two minutes in all parts during cooking. This requirement should be followed to prepare safe food.
While bacteria are killed when heated, bacterial spores can survive high temperatures. Such spores are able to germinate and the vegetative bacteria can multiply and form toxins. Keeping food hot until it is served at a minimum of 60 degrees on all parts of the heated food can prevent spores from germinating and bacteria from multiplying.
Establishments that regularly cater for particularly vulnerable persons have a special responsibility when selecting their staff. They should be competent, experienced and regularly trained.
Posted in food bourne outbreak, food contamination, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Pathogen, Food Poisoning, Food Safety, Food Spoilage, Food Temperature Abuse, Food Testing, Food Toxin, foodborne disease, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Research
USA – El Abuelito Listeria Pregnancy Related Illnesses Added to Outbreak Total
Two El Abuelito Listeria pregnancy related illnesses were added to the listeriosis soft cheese outbreak total last week by the Centers for Disease Control and Prevention (CDC). That company’s queso fresco cheese was recalled earlier this month because lab tests conducted by the Connecticut Department of Health found the outbreak strain of Listeria monocytogenes in one sample of the product. Also last week, two more types of El Abuelito cheese were recalled: Quesillo (Oaxaca and string cheese) and Requeson (ricotta).
Posted in food bourne outbreak, food contamination, food death, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Alert, Food Testing, foodborne outbreak, foodbourne outbreak, Listeria, Listeria monocytogenes, outbreak
Taiwan – CDC issues Norovirus warning after Taiwan sees surge in cases

The health authorities are sounding the alarm over norovirus-induced gastroenteritis, with cases soaring over the past week.
Taiwan recorded over 138,000 cases of diarrhea between Feb. 21 and 27, reflecting an uptick in stomach illnesses following the Lunar New Year. Over the past four weeks, 87 diarrhea clusters have been reported nationwide, and 97 percent of the 58 cases where pathogens were identified pointed to norovirus as the culprit, according to the Taiwan Centers for Disease Control (CDC).
Members of the public are urged to improve their hygiene, as the virus is transmitted via the fecal-oral route, which involves contaminated food or water or contact with infected persons.
Posted in food bourne outbreak, food contamination, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, Food Safety, Food Safety Alert, Food Testing, Food Virus, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, Norovirus, outbreak, Virus, Water, water microbiology, Water Safety
USA – Outbreak Investigation of Listeria monocytogenes – Hispanic-style Fresh and Soft Cheeses (February 2021) – Update
Case Counts
Total Illnesses: 11
Hospitalizations: 10
Deaths: 1
Last Illness Date: 2/14/2021
States with Cases: CT (1), MD (4), NY (4), and VA (2)
Product Distribution*: CT, GA, IL, IN, MA, MD, NC, NJ, NY, PA, VA
*States with confirmed distribution; product could have been distributed further
Posted in food bourne outbreak, food contamination, food death, Food Hazard, Food Hygiene, Food Illness, Food Inspections, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Testing, Food Pathogen, food recall, Food Safety, Food Safety Alert, Food Testing, foodborne outbreak, foodbourne outbreak, Listeria, Listeria monocytogenes, outbreak
South Africa – Tiger Brands outbreak killed young mother, leaving her twin sisters to raise her daughter – Listeria monocytogenes
South African Nthabiseng Zaza liked traveling and gospel music. She liked shoes, especially designer brands like Michael Kors. “She was the life of the party,” Matlhogonolo said, Nthabiseng’s 26-year-old sister.
Nthabiseng was a person who loved family above all else. She always wanted to have kids and was blessed with a daughter, Onthathile, who turns 5 this month. Matlhogonolo Chantell and her twin sister Michell Masego Zaza are raising their sister’s daughter.
Onthathile doesn’t remember much of her mother, who at the age of 35 died from listeriosis in Oct. 2018. Her death was part of a Listeria outbreak in South Africa that was traced to Tiger Brand’s polony — processed deli meat similar to baloney.
However, it wasn’t until 2020 that the family found out what had caused their Nthabiseng’s mysterious illness. They knew only that many people in the country were getting sick.
Posted in Death, food bourne outbreak, food death, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, Listeria, Listeria monocytogenes, listeriosis, microbial contamination, Microbiology, outbreak, Research, south africa