FSA
The Food Standards Agency (FSA), Food Standards Scotland (FSS) with Ipsos MORI have published a survey of consumer practices relating to coated frozen chicken products.
This survey identifies behaviours which could increase people’s risk to foodborne disease. It was commissioned as a result of a Salmonella incident linked to frozen chicken products such as nuggets, goujons, dippers, poppers and kievs. While these products may appear cooked on the outside, they often contain raw chicken and so they must be cooked thoroughly to help kill Salmonella bacteria.
Findings show that two thirds of adults aged 16-75 (67%) say they have recently cooked or eaten coated frozen chicken products at home. These products are particularly popular with younger adults, with 88% of those aged 16-24 having recently consumed them or cooked them at home. Participants were also more likely to have cooked or eaten these products if they have children aged 15 or under in their household (86%).
The survey also included questions on the storage and handling of these products pre and post-cooking:
- Almost two thirds of those who cook these products (62%) say uncooked coated frozen chicken products at least sometimes come into contact with other surfaces such as worktops and plates
- Over half of those who cook these products (58%) say they always wash their hands after handling coated frozen chicken products
- Almost a quarter of consumers who personally cook products say they defrost them before cooking (23%), 62% say they do not. Among those who defrost products, half say they leave them at room temperature (53%)
Most participants who use an oven to cook coated frozen chicken products say they sometimes cook them together with other products, such as chips or vegetables (84%). Cooking these chicken products at a lower temperature or for a shorter time than advised may mean they are not thoroughly cooked before serving.
Narriman Looch, Head of Animal Feed and Foodborne Disease Control Branch said: ‘It’s important to understand that frozen chicken products often contain raw chicken, even though they may look pre-cooked on the outside. While additional measures have been put in place by food businesses to improve the safety of these products, consumers need to handle these products as they should other raw meat products. Cooking food at the right temperature and for the right amount of time will kill any Salmonella bacteria that may be in food. Therefore, we are urging consumers to follow cooking instructions for these products to protect themselves and their families.’
Food safety tips for frozen breaded chicken products:
- Treat these products as raw chicken, ensuring they are steaming hot after cooking and surfaces they have touched are cleaned to avoid the spread of bacteria
- Make sure the oven is up to temperature before cooking
- Check the instructions on packaging and cook at the correct temperature and for the time stated
- Wash your hands, utensils and clean surfaces after handling these products
- If products require defrosting, follow the storage instructions on packaging and always defrost in the fridge
About this poll
The FSA and FSS commissioned an online survey via three waves of Ipsos MORI’s online omnibus of 5,599 adults (aged 16-75) living in the UK. Of these 3,740 had cooked or eaten coated frozen chicken products recently and went on to complete the full survey. The data was weighted to be representative of the UK adult population aged 16 – 75.
The full report is available in the research section of our website.
About the outbreak
FSA and FSS are continuing to work with Public Health England (PHE) and devolved public health authorities as well as our international food safety partners, via the United Nations’ World Health Organization, (WHO) and the Food and Agriculture Organization’s (FAO’s) International Food Safety Network (INFOSAN), to address the causes of the outbreak at source to prevent further cases of Salmonella Enteritidis.
Between January 2020 and May 2021 there have been 511 cases of Salmonellosis in the UK caused by two strains of Salmonella Enteritidis and linked to consumption of frozen, raw, breaded chicken products.
Authorities in Poland and UK retailers have taken action to reduce the risk from these products. Where non-compliant or unsafe food has been identified by the UK, action has been taken to protect consumers.
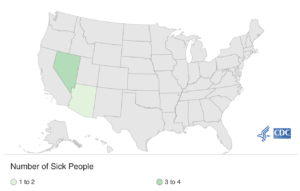 As of June 25, 2021, six people infected with the outbreak strain of Salmonella Weltevreden have been reported from two states – Arizona and Nevada (see map). Illnesses started on dates ranging from February 26, 2021, to April 25, 2021 (see timeline).
As of June 25, 2021, six people infected with the outbreak strain of Salmonella Weltevreden have been reported from two states – Arizona and Nevada (see map). Illnesses started on dates ranging from February 26, 2021, to April 25, 2021 (see timeline).

