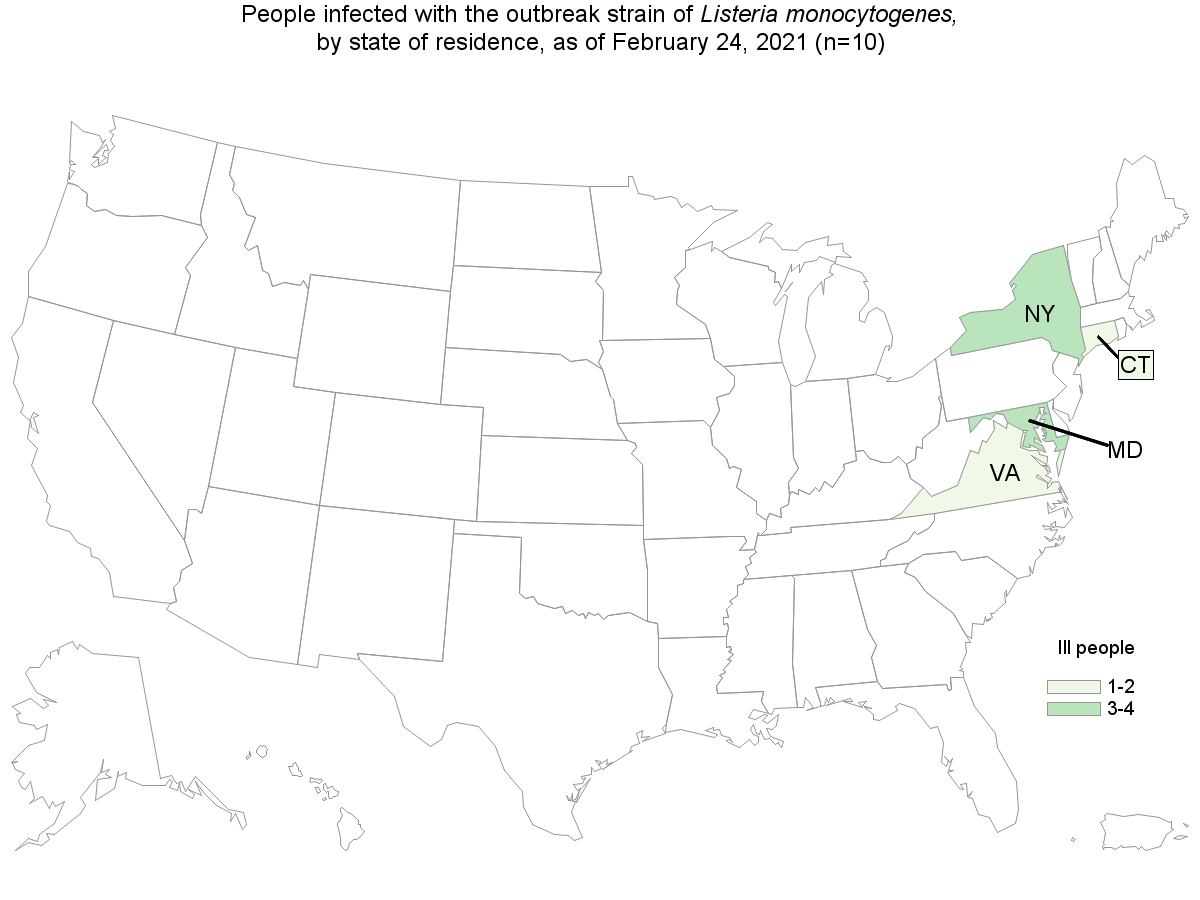
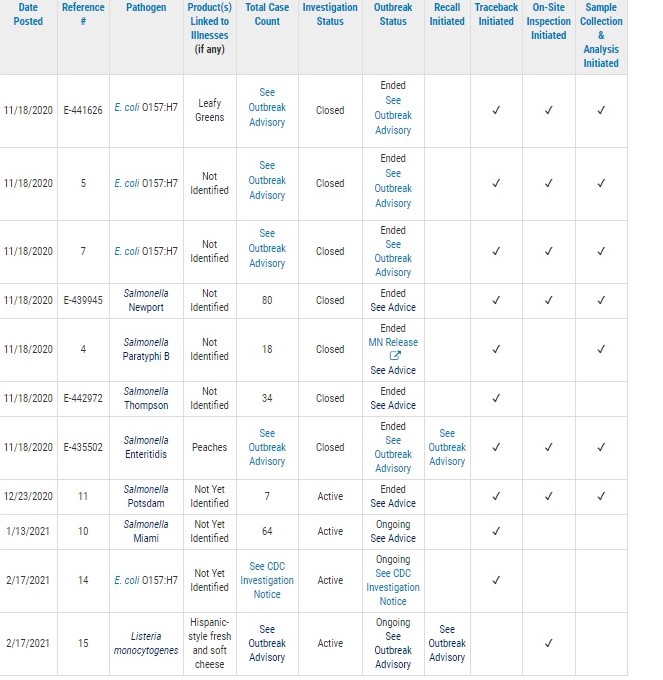
The FDA, along with CDC and state and local partners, are investigating a multistate outbreak of Listeria monocytogenes infections linked to queso fresco cheeses made by El Abuelito Cheese, Inc.
As part of this outbreak investigation, the Connecticut Department of Public Health collected product samples of El Abuelito-brand Hispanic-style fresh and soft cheeses from a store where a sick person bought cheeses. On 2/19/2021, Whole Genome Sequencing (WGS) analysis conducted by the Connecticut State Laboratory determined that the Listeria monocytogenes found in the samples is a match to the outbreak strain. At this time, El Abuelito Cheese, Inc. has ceased production and distribution of all products processed or handled in the same facility as the Queso Fresco.
The FDA has initiated an on-site inspection of the facility. On 2/24/2021, the firm notified customers via letter that it was expanding the recall announced on 2/19/2021. The expanded recall includes El Abuelito, Rio Grande, and Rio Lindo brand queso frescos. It also includes El Abuelito-brand Quesillo (Oaxaca, string cheese), and Requeson (Ricotta) cheeses that are manufactured or handled in the same facility as the Queso Fresco products linked to this outbreak.
At this time, FDA is recommending that in addition to the recalled queso fresco cheeses, consumers, restaurants, and retailers should not eat, sell, or serve any El Abuelito-brand Quesillo (Oaxaca, string cheese) or Requeson (Ricotta) cheeses.
The FDA’s recommendation does not include any additional products with the El Abuelito Cheese, Inc. label because they are not manufactured or handled in the same facility; this includes El Abuelito Meat, Inc., Panela cheese, cotija cheese, mole, crema centroamericana, and crema mexicana. Updates will be provided as they become available.
Recommendation
Consumers, restaurants, and retailers should not eat, sell, or serve any recalled El Abuelito, Rio Grande, or Rio Lindo brand queso fresco cheeses. Additionally, they should not eat, sell, or serve any El Abuelito brand Quesillo (Oaxaca, string cheese) or Requeson (Ricotta) cheeses.
FDA recommends that anyone who purchased or received any El Abuelito brand Quesillo, Requeson, or recalled Queso Fresco cheeses use extra vigilance in cleaning and sanitizing any surfaces and containers that may have come in contact with these products to reduce the risk of cross-contamination. Listeria can survive in refrigerated temperatures and can easily spread to other foods and surfaces.
If you are at higher risk for severe Listeria illness (if you are pregnant, aged 65 or older, or have a weakened immune system due to certain medical conditions or treatments) do not eat any recalled El Abuelito, Rio Grande, or Rio Lindo brand Queso Fresco cheeses and do not eat any brand of quesillo or requeson cheeses until we learn more about whether other brands of cheeses may be affected.
- Ask your retailer if any queso fresco cheese you buy is supplied by El Abuelito. If you are unable to obtain an answer, do not buy it and throw away the queso fresco cheese you have at home.
- Call your healthcare provider right away if you have these symptoms after eating any queso fresco, quesillo, or requeson cheeses:
- Pregnant people typically experience only fever, fatigue, and muscle aches. However, Listeria infection during pregnancy can lead to miscarriage, stillbirth, premature delivery, or life-threatening infection of the newborn.
- People who are not pregnant may experience headache, stiff neck, confusion, loss of balance, and convulsions, in addition to fever and muscle aches.
- Follow these five steps to clean your refrigerator, containers, and surfaces that may have touched the cheeses. Listeria can survive in the refrigerator and can easily spread to other foods and surfaces.