ECDC
Hepatitis A cases in 2021 were at their lowest levels since EU-level hepatitis A surveillance began in 2007, while five other food and waterborne diseases are rising towards pre-pandemic levels. The information is revealed in the Annual Epidemiological Report 2021, of which six chapters are published today by ECDC.
The chapters cover diseases causing the highest number of food- and waterborne infections in the EU/EEA, namely campylobacteriosis, salmonellosis, yersiniosis, shigatoxigenic Escherichia coli infection, listeriosis, and hepatitis A.
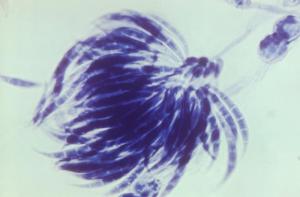
In the EU/EEA, the hepatitis A notification rate was exceptionally low in 2021, with 0.92 cases per 100 000 population, compared to 2.2 in 2019. This can be attributed primarily to the COVID-19 pandemic and restrictions, including reduced international travel.
However, a sharp decline in the trend of hepatitis A cases has also been evident in the EU/EEA over the last five years. Additional factors contributing to this may be the heightened awareness of hepatitis A transmission, increased preventive measures such as practising good hygiene and increased vaccine uptake among at-risk groups. Increased natural immunity in at-risk groups following a large multi-country outbreak occurring in 2017 and 2018 may also be of importance.
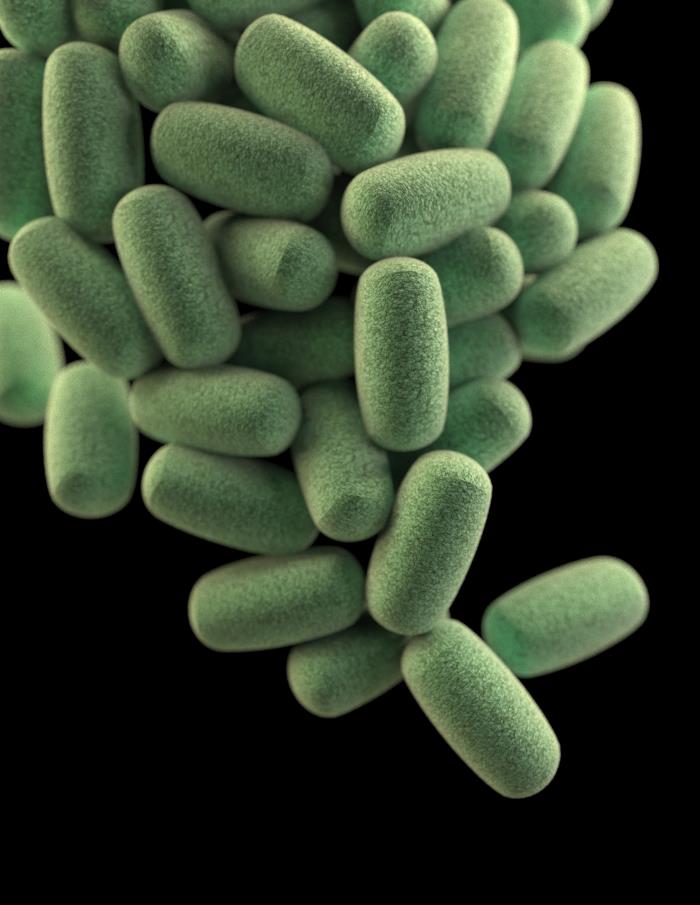
In 2020, the number of cases of campylobacteriosis and salmonellosis, the two most commonly reported gastrointestinal infections in the EU/EEA, decreased notably due to the COVID-19 pandemic. Unlike hepatitis A, these appeared to increase in 2021, but the levels are still well below those of the pre-pandemic years. This could partly be an effect of reduced travel as travel-related infections were at their lowest in 2021.
Listeriosis, shigatoxigenic Escherichia coli infections and yersiniosis trends decreased less notably in 2020 and the number of cases returned to the pre-pandemic levels in 2021. This might be due to the more severe symptoms caused particularly by listeriosis and shigatoxigenic Escherichia coli infections, which are then more likely to be diagnosed and reported. Additionally, many of the cases are acquired within the EU/EEA, and the numbers are not as affected by international travel restrictions.
In 2021, although the COVID-19 pandemic was still ongoing, the gradual reduction of COVID-19 restriction measures, along with the return to normal daily life (social events, doctor’s visits, travel), the reopening of bars, restaurants and catering facilities (i.e. schools, workplaces), may explain the increase in cases of the five food- and waterborne diseases.