Information on some of the most common bacteria and viruses that cause foodborne illnesses is provided below:
Archives
-
Join 347 other subscribers
KSWFoodWorld
Blog Stats
- 441,658 Views
Information on some of the most common bacteria and viruses that cause foodborne illnesses is provided below:
Norwegian surveillance has found a low level of flour samples positive for Shiga toxin-producing E. coli (STEC).
The Norwegian Food Safety Authority (Mattilsynet) commissioned a survey of STEC in wheat flour to gather data on the problem.
A total of 151 samples of flour were collected from retailers in 2021 and analyzed in 2022. Enriched samples were examined for the presence of selected genetic markers. Attempts to isolate STEC were carried out from samples that were positive for Shiga toxin (stx) 1 and/or stx2. Isolates identified as STEC were further characterized using whole genome sequencing.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, STEC, STEC E.coli
Five people are sick in France, two seriously, and one in Belgium after drinking a brand of raw fermented milk.
In France, four children and one adult have been infected by Shiga toxin-producing E. coli (STEC) O26:H11. They fell ill between the end of March and the beginning of April this year.
Santé publique France has been investigating two cases of Hemolytic Uremic Syndrome (HUS) in the Hauts-de-France and Île-de France regions. The latter was in the context of a family outbreak. The suspected food was fermented raw milk. HUS is a severe complication associated with E. coli infections that causes kidney failure.
“The sequencing of the strains isolated within these outbreaks confirmed the same genomic profile. Food investigations made it possible to identify, for the case in Hauts-de-France, the place of purchase and to sample milk on sale at the time of the inspections. It was fermented raw milk made in Belgium,” agency officials told Food Safety News.
Posted in Decontamination Microbial, E.coli O26, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, STEC, STEC E.coli
| Reason for alert | Paralytic Shellfish Poisoning (PSP) |
| Date warning issued | Extended 18 May 2023 |
| Affected area | Firth of Thames. |
| Shellfish affected | Mussels, oysters, tuatua, pipi, toheroa, cockles, scallops, catseyes, kina (sea urchin) and all other bivalve shellfish.
Note, cooking shellfish does not remove the toxin. Pāua, crab and crayfish may still be eaten if the gut has been completely removed prior to cooking, as toxins accumulate in the gut. If the gut is not removed its contents could contaminate the meat during the cooking process. |
| Symptoms | Symptoms typically appear between 10 minutes and 3 hours after ingestion and may include:
|
| Other information | Paralytic shellfish toxins have been detected in shellfish from the Kaipara Harbour at levels over the safe limit of 0.8mg/kg set by MPI. Ongoing testing will continue and any changes will be communicated accordingly. |
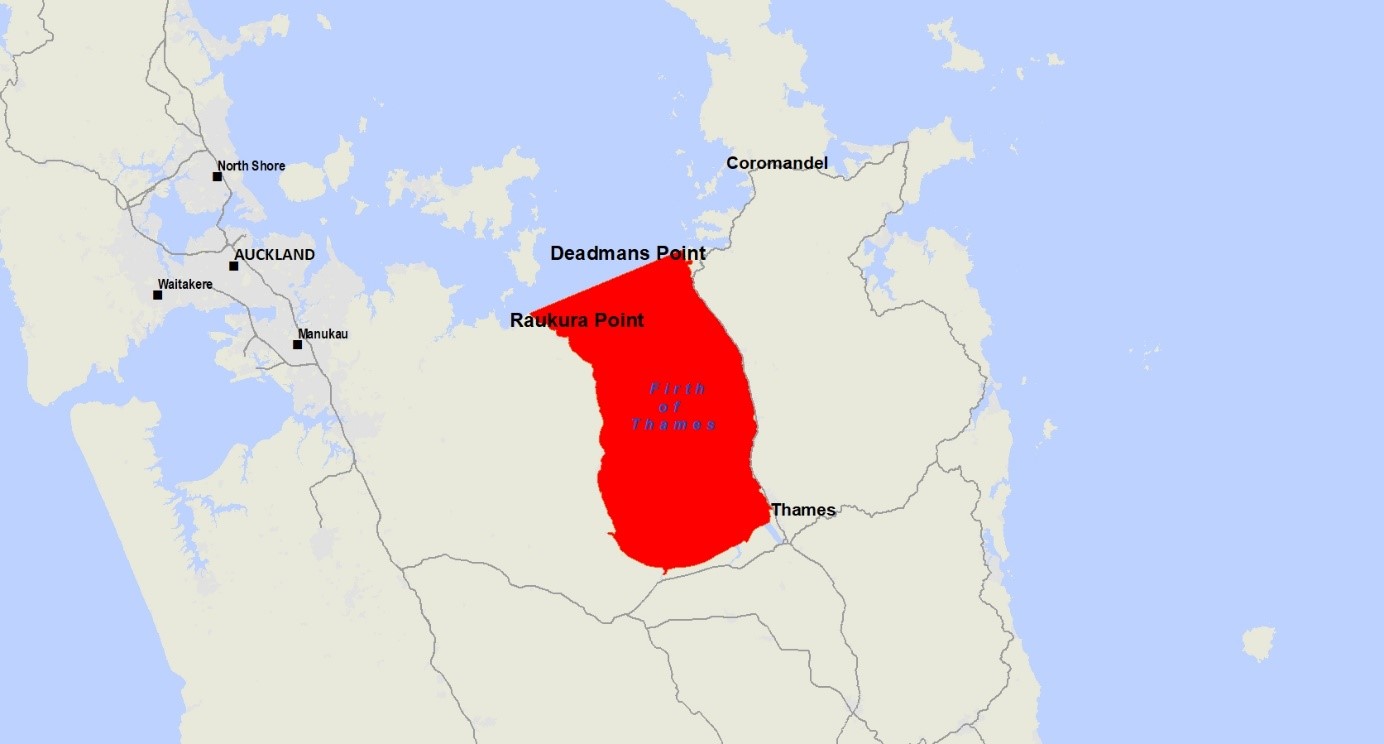
We test shellfish and seawater for toxic algae every week from popular shellfish gathering areas around New Zealand. If the shellfish are not safe to eat, we issue public health warnings and put up signs at affected beaches.
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, MPI, paralytic shellfish poisoning, Shellfish, shellfish toxin
Nongpoh, May 12: Dozens of villagers from Nongladew village in Ri Bhoi district of Meghalaya fell ill after attending a funeral service in Mariampur under Goalpara District of Assam. As many as 41 villagers had attended the funeral rituals of their relative on May 9. However, on Wednesday night (May 10), 31 of them returned home and fell ill, prompting immediate action from health officials.
The villagers had consumed fish, potato, and dal during the funeral service, and many of them complained of illness when they returned home. While the exact cause of the illness is not known, the villagers suspect the fish, which they believe was poisoned, to be the reason for their condition
Posted in Decontamination Microbial, Food Illness, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Food Poisoning, Foodborne Illness, foodborne outbreak, foodbourne outbreak, Illness, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, outbreak, Poisoning
Posted in Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, Listeria, Listeria monocytogenes, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Salmonella, STEC, STEC E.coli
A new study suggests that Escherichia coli infection from contaminated meat products may be responsible for hundreds of thousands of urinary tract infections in the U.S. each year.
A team of scientists led by George Washington University (GWU) Milken Institute School of Public Health researchers have developed a new genomic approach for tracking the origins of E. coli infections. Using this method, the team estimated that between 480,000 and 640,000 UTIs in the United States each year may be caused by foodborne E. coli strains.
According to GWU, E. coli is the most common cause of UTIs, causing upwards of 85 percent of cases each year. Women are at greater risk of developing UTIs, which can range from simple bladder infections to life-threatening bloodstream infections. At present, only specific types of diarrhea-causing E. coli, such as E. coli O157:H7, are rigorously monitored by the U.S. Food and Drug Administration (FDA), but the new findings from GWU suggest that other strains may also pose serious health risks.
In the study, researchers collected raw chicken, turkey, and pork from major grocery store chains in Flagstaff, Arizona, and isolated E. coli from the meat samples. Simultaneously, researchers collected urine and blood E. coli isolates from patients hospitalized at the Flagstaff Medical Center for UTIs.
Posted in bacterial contamination, Contaminated water, Decontamination Microbial, E.coli, escherichia coli, food contamination, Food Micro Blog, Food Microbiology, Food Microbiology Blog, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk
Posted in Biofilm, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Salmonella
Climate change and its worldwide effects are undeniable. Temperature increase due to climate change may affect foodborne pathogen survival on fresh produce. This study aimed to present an evaluation of climate change impact regarding temperature rise situations, on attachment of different pathogenic Escherichia coli strains on cress grown under controlled conditions. EHEC O157:H7, EAEC O104:H4 and EPEC O26 were inoculated with initial inoculum concentration of 8 log MPN/mL at different stages during growth to observe how inoculation time (7, 14, 21 and 28 days post sowing; dps) and route (seed and leaves) affect pathogen load on fresh produce. This study revealed that temperature increase designed according to mitigation scenarios for climate change (+2, +4 and +6 °C) did not cause any considerable change in pathogen persistence on leaf at 30 dps (~4.5 to 7 log MPN/g). In plants contaminated at later stage (21 and 28 dps), higher bacterial populations were obtained for all temperatures studied. Our results show that E. coli translocated towards leaf portions from seed and established significant amount of pathogen load on leaf (~4 to 5.3 log MPN/g). Also, inoculated bacteria have tightly bound to leaf (~3.5 to 7 log MPN/g) and cannot be eliminated by washing. Although persistence of E. coli O157:H7, O104:H4 and O26 did not differ significantly according to temperature, the bacterial load on the leaves was above infectious dose for humans.
Posted in Climate change, Decontamination Microbial, E.coli O104, E.coli O157, E.coli O157:H7, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, STEC, STEC E.coli

Researchers at the University of Texas (UT) Southwestern Medical Center have discovered how foodborne pathogen Vibrio parahaemolyticus infects people after eating raw or undercooked shellfish. The findings could lead to new ways to treat illness caused by the enteric bacteria.
The study provides the first visual evidence of how a gut bacterial pathogen uses an “assembly method” to build syringe-like structures to inject toxins into intestinal cells, giving a new view of how enteric bacteria, when exposed to bile acids, efficiently respond and build a virulence system.
Posted in Antimicrobials, Decontamination Microbial, Food Micro Blog, Food Microbiology, Food Microbiology Blog, Food Microbiology Research, Food Microbiology Testing, microbial contamination, Microbial growth, Microbiological Risk Assessment, Microbiology, Microbiology Investigations, Microbiology Risk, Vibrio, Vibrio albensis, Vibrio alginolyticus, Vibrio cholera, vibrio cholerae, Vibrio parahaemolyticus, Vibrio vulnificans, Vibrio vulnificus