FDA
Audience
Consumers who have recently purchased Little Hatch’s:
- Jalapeno Cream Cheese Dip (13.5 oz or 14 oz)
- Queso (13.5 oz)
- Spicy Queso (13.5 oz)
- Roasted Chili Salsa Medium (13.5 oz)
- Roasted Chili Salsa Hot (13.5 oz)
Product
- Little Hatch’s ready to eat foods: Jalapeno Cream Cheese Dip, Queso, Spicy Queso, Roasted Chili Salsa Medium and Roasted Chili Salsa Hot, sold in 13.5 oz or 14 oz containers in the refrigerated section of grocery stores
- Little Hatch’s products are manufactured by Interstate Food Products, LLC and distributed to:
- Whole Foods Market Distribution Center, Denver, CO
- Whole Foods Market Rocky Mountain Regional states – CO, KS, MO, NM, UT, TX, WY
- Natural Grocers, Denver, CO
- Lucky Market, Denver, CO
Purpose
The FDA advises consumers not to purchase or eat Little Hatch’s ready to eat Jalapeno Cream Cheese Dip, Queso, Spicy Queso, Roasted Chili Salsa Medium and Roasted Chili Salsa Hot sold in 13.5 oz or 14 oz containers due to a possible Listeria monocytogenes contamination. Listeria monocytogenes is a species of disease-causing bacteria, which causes an infection called listeriosis. A listeriosis infection can have serious adverse effects for women who are or may become pregnant, the elderly, and persons with weakened immune systems.
Summary of Problem and Scope
The FDA detected Listeria monocytogenes in retail samples of Jalapeno Cream Cheese Dip, Queso and Spicy Queso and subsequently initiated an inspection at the manufacturing facility. The FDA confirmed Listeria monocytogenes in 23 of 149 samples taken from processing, packaging, and storage areas at the facility, including various food-contact surfaces.
On May 20 2021, Interstate Food Products, initiated a voluntary recall of “Little Hatch’s” brand Jalapeno Cream Cheese, Queso, and Spicy Queso products with specific sell by dates that the FDA tested and found positive for Listeria monocytogenes. On June 15, 2021, Interstate Food Products indicated to the FDA that they may need to further expand the recall to include “Little Hatch’s” brand Roasted Chili Salsa Hot after conducting their own testing and confirming additional positive Listeria monocytogenes findings.
FDA Actions
The FDA is issuing this alert because the agency is concerned with the firm’s ongoing Listeria monocytogenes contamination. The FDA is continuing its efforts to remove Little Hatch’s product from the market.
Recommendations for Consumers
- Contact your healthcare providers immediately if you are experiencing illness after consuming these products.
- Contact your healthcare providers if you have recently consumed these products and are concerned about your health.
- Consumers who have purchased these products should throw the food away and follow these steps:
- Wash the inside walls and shelves of the refrigerator, cutting boards and countertops, and utensils that may have had contact with contaminated foods; then sanitize them with a solution of one tablespoon of chlorine bleach to one gallon of hot water; dry with a clean cloth or paper towel that has not been previously used.
- Wipe up spills in the refrigerator immediately and clean the refrigerator regularly.
- Wash hands with warm water and soap for at least 20 seconds before and after handling food and following any cleaning and sanitation process.
- Pregnant women, the elderly and those with weakened immune systems should avoid certain foods, including raw fish, which carry a higher risk for Listeria monocytogenes.
Reporting Problems to the FDA
To report a complaint or adverse event (illness or injury), you can
Visit www.fda.gov/fcic for additional consumer and industry assistance.





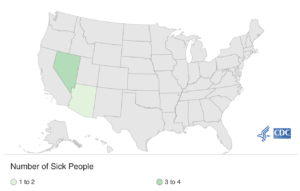 As of June 25, 2021, six people infected with the outbreak strain of Salmonella Weltevreden have been reported from two states – Arizona and Nevada (see
As of June 25, 2021, six people infected with the outbreak strain of Salmonella Weltevreden have been reported from two states – Arizona and Nevada (see 