The outbreak is characterised by an unusually high proportion of children being hospitalised, some with severe clinical symptoms such as bloody diarrhoea. Based on interviews with patients and initial analytical epidemiological studies, specific chocolate products have been identified as the likely route of infection. Affected cases have been identified through advanced molecular typing techniques. As this method of testing is not routinely performed in all countries, some cases may be undetected.
Product recalls have been launched in several countries to date, including Belgium, France, Germany, Ireland, Luxembourg, Netherlands, Norway, and the UK, to prevent the consumption of products potentially contaminated with Salmonella. Further investigations are being conducted by public health and food safety authorities in countries where cases are reported, to identify the cause and the extent of the contamination, and to ensure contaminated products are not put on the market.
ECDC and EFSA are assessing the available data from these countries and preparing a rapid outbreak assessment to be published next week. Questions regarding ongoing product recalls should be addressed to national food safety authorities.
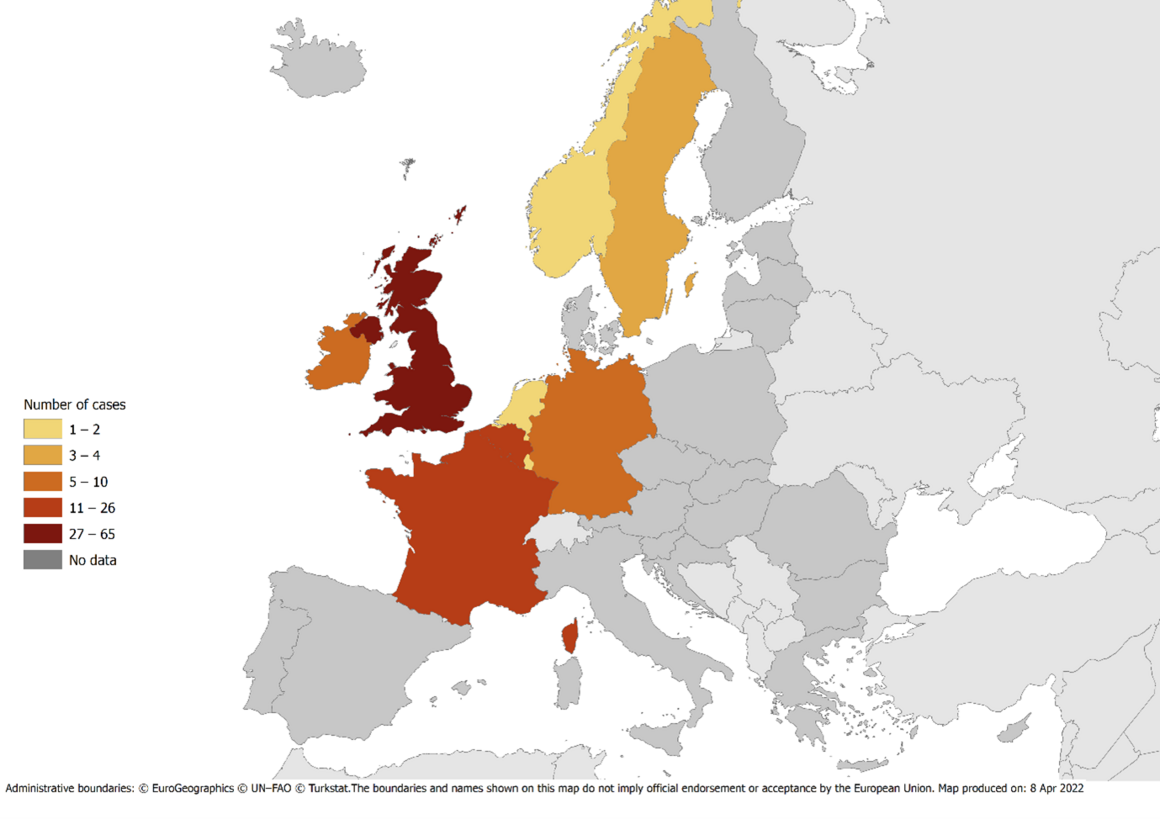
Number of confirmed and probable cases* with monophasic S. Typhimurium infection by country, EU/EEA and the UK, as of 8 April 2022