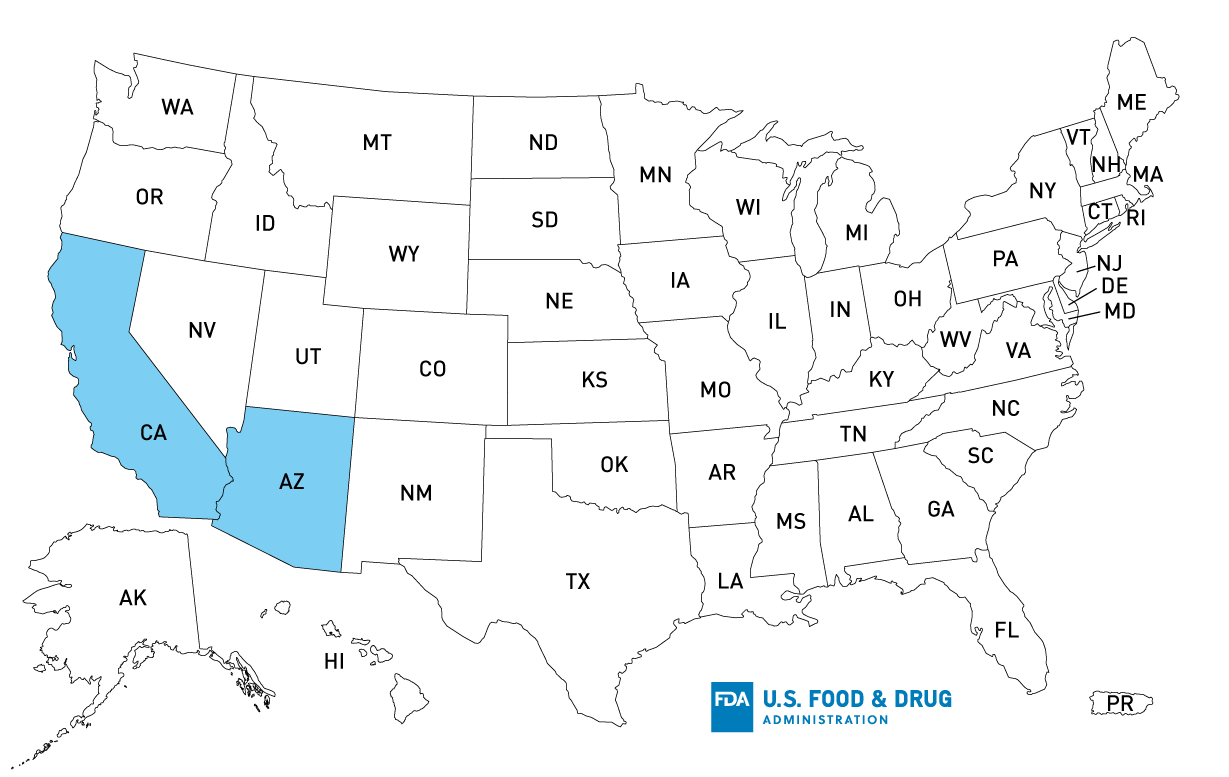
The FDA, along with CDC and state and local partners, is investigating a multistate outbreak of Salmonella Litchfield infections linked to fresh, raw salmon supplied to restaurants in California and Arizona by Mariscos Bahia, Inc.
Based on epidemiologic information provided by CDC and interviews conducted by state and local public health officials, of 16 people interviewed, 12 reported eating sushi, sashimi, or poke. Of those interviewed, 11 people remembered details about the type of fish consumed and 9 report eating raw salmon before getting sick. The FDA’s investigation traced the distribution of fresh, raw salmon back to Mariscos Bahia, Inc.
In addition, the FDA collected an environmental sample that included multiple swabs at Mariscos Bahia, Inc. (Pico Rivera, CA). Multiple environmental swabs collected at the facility are positive for Salmonella and subsequent Whole Genome Sequencing (WGS) analysis is ongoing. The WGS completed to date indicates the Salmonella detected in at least one of the swabs from the facility matches the outbreak strain. While epidemiological evidence indicates that ill people consumed fresh, raw salmon processed at this firm, the presence of Salmonella in the processing environment indicates that additional types of fish processed in the same area of the facility could also be contaminated which includes fresh, raw halibut, Chilean seabass, tuna, and swordfish. Salmon, halibut, Chilean seabass, tuna, and swordfish processed in Marisco Bahia Inc.’s Pico Rivera, CA, facility could have also been sent to the Mariscos Bahia, Inc. facilities in Phoenix, AZ and then sent to restaurants.
The firm is cooperating with the FDA investigation and has agreed to initiate a voluntary recall. As a part of the firm’s voluntary recall, the firm will contact its direct customers who received recalled product.
The FDA’s investigation is ongoing. Updates to this advisory will be provided as they become available.
Recommendation
According to Mariscos Bahia, Inc., seafood was only sold directly to restaurants in California and Arizona and would not be available for purchase by consumers in stores.
Restaurants should check with their suppliers and not sell or serve salmon, halibut, Chilean seabass, tuna, and swordfish received fresh, not frozen from Mariscos Bahia, Inc. (Pico Rivera, CA and Phoenix, AZ) on or after June 14, 2022. If restaurants received these fish and then froze it, they should not sell or serve it. Restaurants should also be sure to wash and sanitize locations where these fish from Mariscos Bahia, Inc. were stored or prepared.
Consumers eating salmon, halibut, Chilean seabass, tuna, and swordfish at a restaurant in California or Arizona should ask whether the fish is from Mariscos Bahia, Inc and was received fresh, not frozen.