Facing up to the challenge
We understand that we have a role to play to reduce the level of Campylobacter in the supply chain and to help raise awareness with our customers as to how they can handle fresh poultry in a safe manner.
The Food Standards Agency (FSA) has identified Campylobacter as a key priority and is working with those directly in the industry to tackle it. Aldi is dedicated to supporting the FSA in this goal, which is why we are a signatory of the Acting on Campylobacter Together (ACT) campaign.
As well as working with the FSA (and other industry bodies), we understand that we need to take a lead with our suppliers to deliver against the FSA target.
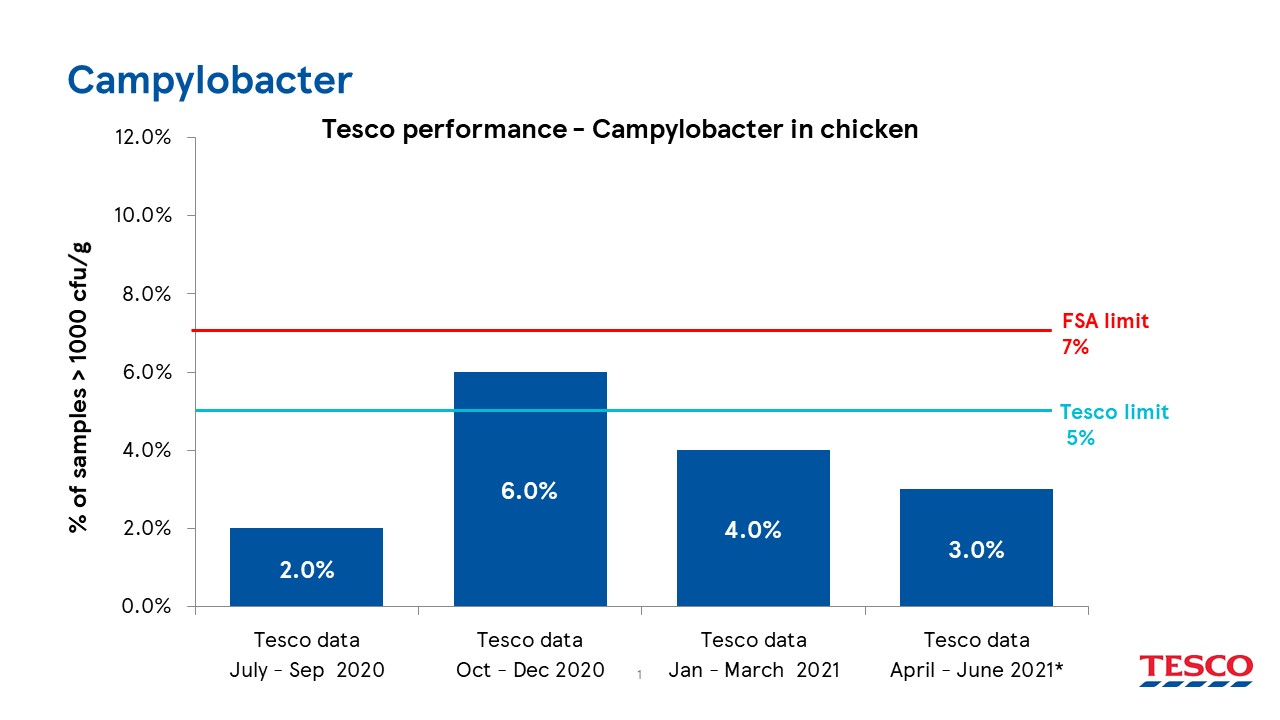
Aldi monitors the levels of Campylobacter carefully by compiling regular sets of independently verified data which is shared with the FSA via the BRC for the purposes of industry reporting. The results for Q2 2021 (April to June) show that 4.2% of birds were in the >1,000 cfu/g category. Our results are below the FSA target of less than 7% of birds in the >1,000 cfu/g category.